- Link to facebook
- Link to linkedin
- Link to twitter
- Link to youtube
- Writing Tips

What is the Purpose of a Literature Review?

4-minute read
- 23rd October 2023
If you’re writing a research paper or dissertation , then you’ll most likely need to include a comprehensive literature review . In this post, we’ll review the purpose of literature reviews, why they are so significant, and the specific elements to include in one. Literature reviews can:
1. Provide a foundation for current research.
2. Define key concepts and theories.
3. Demonstrate critical evaluation.
4. Show how research and methodologies have evolved.
5. Identify gaps in existing research.
6. Support your argument.
Keep reading to enter the exciting world of literature reviews!
What is a Literature Review?
A literature review is a critical summary and evaluation of the existing research (e.g., academic journal articles and books) on a specific topic. It is typically included as a separate section or chapter of a research paper or dissertation, serving as a contextual framework for a study. Literature reviews can vary in length depending on the subject and nature of the study, with most being about equal length to other sections or chapters included in the paper. Essentially, the literature review highlights previous studies in the context of your research and summarizes your insights in a structured, organized format. Next, let’s look at the overall purpose of a literature review.
Find this useful?
Subscribe to our newsletter and get writing tips from our editors straight to your inbox.
Literature reviews are considered an integral part of research across most academic subjects and fields. The primary purpose of a literature review in your study is to:
Provide a Foundation for Current Research
Since the literature review provides a comprehensive evaluation of the existing research, it serves as a solid foundation for your current study. It’s a way to contextualize your work and show how your research fits into the broader landscape of your specific area of study.
Define Key Concepts and Theories
The literature review highlights the central theories and concepts that have arisen from previous research on your chosen topic. It gives your readers a more thorough understanding of the background of your study and why your research is particularly significant .
Demonstrate Critical Evaluation
A comprehensive literature review shows your ability to critically analyze and evaluate a broad range of source material. And since you’re considering and acknowledging the contribution of key scholars alongside your own, it establishes your own credibility and knowledge.
Show How Research and Methodologies Have Evolved
Another purpose of literature reviews is to provide a historical perspective and demonstrate how research and methodologies have changed over time, especially as data collection methods and technology have advanced. And studying past methodologies allows you, as the researcher, to understand what did and did not work and apply that knowledge to your own research.
Identify Gaps in Existing Research
Besides discussing current research and methodologies, the literature review should also address areas that are lacking in the existing literature. This helps further demonstrate the relevance of your own research by explaining why your study is necessary to fill the gaps.
Support Your Argument
A good literature review should provide evidence that supports your research questions and hypothesis. For example, your study may show that your research supports existing theories or builds on them in some way. Referencing previous related studies shows your work is grounded in established research and will ultimately be a contribution to the field.
Literature Review Editing Services
Ensure your literature review is polished and ready for submission by having it professionally proofread and edited by our expert team. Our literature review editing services will help your research stand out and make an impact. Not convinced yet? Send in your free sample today and see for yourself!
Share this article:
Post A New Comment
Got content that needs a quick turnaround? Let us polish your work. Explore our editorial business services.
5-minute read
Free Email Newsletter Template
Promoting a brand means sharing valuable insights to connect more deeply with your audience, and...
6-minute read
How to Write a Nonprofit Grant Proposal
If you’re seeking funding to support your charitable endeavors as a nonprofit organization, you’ll need...
9-minute read
How to Use Infographics to Boost Your Presentation
Is your content getting noticed? Capturing and maintaining an audience’s attention is a challenge when...
8-minute read
Why Interactive PDFs Are Better for Engagement
Are you looking to enhance engagement and captivate your audience through your professional documents? Interactive...
7-minute read
Seven Key Strategies for Voice Search Optimization
Voice search optimization is rapidly shaping the digital landscape, requiring content professionals to adapt their...
Five Creative Ways to Showcase Your Digital Portfolio
Are you a creative freelancer looking to make a lasting impression on potential clients or...

Make sure your writing is the best it can be with our expert English proofreading and editing.

Literature Review: Purpose of a Literature Review
- Literature Review
- Purpose of a Literature Review
- Work in Progress
- Compiling & Writing
- Books, Articles, & Web Pages
- Types of Literature Reviews
- Departmental Differences
- Citation Styles & Plagiarism
- Know the Difference! Systematic Review vs. Literature Review
The purpose of a literature review is to:
- Provide a foundation of knowledge on a topic
- Identify areas of prior scholarship to prevent duplication and give credit to other researchers
- Identify inconstancies: gaps in research, conflicts in previous studies, open questions left from other research
- Identify the need for additional research (justifying your research)
- Identify the relationship of works in the context of their contribution to the topic and other works
- Place your own research within the context of existing literature, making a case for why further study is needed.
Videos & Tutorials
VIDEO: What is the role of a literature review in research? What's it mean to "review" the literature? Get the big picture of what to expect as part of the process. This video is published under a Creative Commons 3.0 BY-NC-SA US license. License, credits, and contact information can be found here: https://www.lib.ncsu.edu/tutorials/litreview/
Elements in a Literature Review
- Elements in a Literature Review txt of infographic
- << Previous: Literature Review
- Next: Searching >>
- Last Updated: Sep 10, 2024 11:32 AM
- URL: https://uscupstate.libguides.com/Literature_Review
Purdue Online Writing Lab Purdue OWL® College of Liberal Arts
Writing a Literature Review

Welcome to the Purdue OWL
This page is brought to you by the OWL at Purdue University. When printing this page, you must include the entire legal notice.
Copyright ©1995-2018 by The Writing Lab & The OWL at Purdue and Purdue University. All rights reserved. This material may not be published, reproduced, broadcast, rewritten, or redistributed without permission. Use of this site constitutes acceptance of our terms and conditions of fair use.
A literature review is a document or section of a document that collects key sources on a topic and discusses those sources in conversation with each other (also called synthesis ). The lit review is an important genre in many disciplines, not just literature (i.e., the study of works of literature such as novels and plays). When we say “literature review” or refer to “the literature,” we are talking about the research ( scholarship ) in a given field. You will often see the terms “the research,” “the scholarship,” and “the literature” used mostly interchangeably.
Where, when, and why would I write a lit review?
There are a number of different situations where you might write a literature review, each with slightly different expectations; different disciplines, too, have field-specific expectations for what a literature review is and does. For instance, in the humanities, authors might include more overt argumentation and interpretation of source material in their literature reviews, whereas in the sciences, authors are more likely to report study designs and results in their literature reviews; these differences reflect these disciplines’ purposes and conventions in scholarship. You should always look at examples from your own discipline and talk to professors or mentors in your field to be sure you understand your discipline’s conventions, for literature reviews as well as for any other genre.
A literature review can be a part of a research paper or scholarly article, usually falling after the introduction and before the research methods sections. In these cases, the lit review just needs to cover scholarship that is important to the issue you are writing about; sometimes it will also cover key sources that informed your research methodology.
Lit reviews can also be standalone pieces, either as assignments in a class or as publications. In a class, a lit review may be assigned to help students familiarize themselves with a topic and with scholarship in their field, get an idea of the other researchers working on the topic they’re interested in, find gaps in existing research in order to propose new projects, and/or develop a theoretical framework and methodology for later research. As a publication, a lit review usually is meant to help make other scholars’ lives easier by collecting and summarizing, synthesizing, and analyzing existing research on a topic. This can be especially helpful for students or scholars getting into a new research area, or for directing an entire community of scholars toward questions that have not yet been answered.
What are the parts of a lit review?
Most lit reviews use a basic introduction-body-conclusion structure; if your lit review is part of a larger paper, the introduction and conclusion pieces may be just a few sentences while you focus most of your attention on the body. If your lit review is a standalone piece, the introduction and conclusion take up more space and give you a place to discuss your goals, research methods, and conclusions separately from where you discuss the literature itself.
Introduction:
- An introductory paragraph that explains what your working topic and thesis is
- A forecast of key topics or texts that will appear in the review
- Potentially, a description of how you found sources and how you analyzed them for inclusion and discussion in the review (more often found in published, standalone literature reviews than in lit review sections in an article or research paper)
- Summarize and synthesize: Give an overview of the main points of each source and combine them into a coherent whole
- Analyze and interpret: Don’t just paraphrase other researchers – add your own interpretations where possible, discussing the significance of findings in relation to the literature as a whole
- Critically Evaluate: Mention the strengths and weaknesses of your sources
- Write in well-structured paragraphs: Use transition words and topic sentence to draw connections, comparisons, and contrasts.
Conclusion:
- Summarize the key findings you have taken from the literature and emphasize their significance
- Connect it back to your primary research question
How should I organize my lit review?
Lit reviews can take many different organizational patterns depending on what you are trying to accomplish with the review. Here are some examples:
- Chronological : The simplest approach is to trace the development of the topic over time, which helps familiarize the audience with the topic (for instance if you are introducing something that is not commonly known in your field). If you choose this strategy, be careful to avoid simply listing and summarizing sources in order. Try to analyze the patterns, turning points, and key debates that have shaped the direction of the field. Give your interpretation of how and why certain developments occurred (as mentioned previously, this may not be appropriate in your discipline — check with a teacher or mentor if you’re unsure).
- Thematic : If you have found some recurring central themes that you will continue working with throughout your piece, you can organize your literature review into subsections that address different aspects of the topic. For example, if you are reviewing literature about women and religion, key themes can include the role of women in churches and the religious attitude towards women.
- Qualitative versus quantitative research
- Empirical versus theoretical scholarship
- Divide the research by sociological, historical, or cultural sources
- Theoretical : In many humanities articles, the literature review is the foundation for the theoretical framework. You can use it to discuss various theories, models, and definitions of key concepts. You can argue for the relevance of a specific theoretical approach or combine various theorical concepts to create a framework for your research.
What are some strategies or tips I can use while writing my lit review?
Any lit review is only as good as the research it discusses; make sure your sources are well-chosen and your research is thorough. Don’t be afraid to do more research if you discover a new thread as you’re writing. More info on the research process is available in our "Conducting Research" resources .
As you’re doing your research, create an annotated bibliography ( see our page on the this type of document ). Much of the information used in an annotated bibliography can be used also in a literature review, so you’ll be not only partially drafting your lit review as you research, but also developing your sense of the larger conversation going on among scholars, professionals, and any other stakeholders in your topic.
Usually you will need to synthesize research rather than just summarizing it. This means drawing connections between sources to create a picture of the scholarly conversation on a topic over time. Many student writers struggle to synthesize because they feel they don’t have anything to add to the scholars they are citing; here are some strategies to help you:
- It often helps to remember that the point of these kinds of syntheses is to show your readers how you understand your research, to help them read the rest of your paper.
- Writing teachers often say synthesis is like hosting a dinner party: imagine all your sources are together in a room, discussing your topic. What are they saying to each other?
- Look at the in-text citations in each paragraph. Are you citing just one source for each paragraph? This usually indicates summary only. When you have multiple sources cited in a paragraph, you are more likely to be synthesizing them (not always, but often
- Read more about synthesis here.
The most interesting literature reviews are often written as arguments (again, as mentioned at the beginning of the page, this is discipline-specific and doesn’t work for all situations). Often, the literature review is where you can establish your research as filling a particular gap or as relevant in a particular way. You have some chance to do this in your introduction in an article, but the literature review section gives a more extended opportunity to establish the conversation in the way you would like your readers to see it. You can choose the intellectual lineage you would like to be part of and whose definitions matter most to your thinking (mostly humanities-specific, but this goes for sciences as well). In addressing these points, you argue for your place in the conversation, which tends to make the lit review more compelling than a simple reporting of other sources.
Have a language expert improve your writing
Run a free plagiarism check in 10 minutes, generate accurate citations for free.
- Knowledge Base
Methodology
- How to Write a Literature Review | Guide, Examples, & Templates
How to Write a Literature Review | Guide, Examples, & Templates
Published on January 2, 2023 by Shona McCombes . Revised on September 11, 2023.
What is a literature review? A literature review is a survey of scholarly sources on a specific topic. It provides an overview of current knowledge, allowing you to identify relevant theories, methods, and gaps in the existing research that you can later apply to your paper, thesis, or dissertation topic .
There are five key steps to writing a literature review:
- Search for relevant literature
- Evaluate sources
- Identify themes, debates, and gaps
- Outline the structure
- Write your literature review
A good literature review doesn’t just summarize sources—it analyzes, synthesizes , and critically evaluates to give a clear picture of the state of knowledge on the subject.
Instantly correct all language mistakes in your text
Upload your document to correct all your mistakes in minutes
Table of contents
What is the purpose of a literature review, examples of literature reviews, step 1 – search for relevant literature, step 2 – evaluate and select sources, step 3 – identify themes, debates, and gaps, step 4 – outline your literature review’s structure, step 5 – write your literature review, free lecture slides, other interesting articles, frequently asked questions, introduction.
- Quick Run-through
- Step 1 & 2
When you write a thesis , dissertation , or research paper , you will likely have to conduct a literature review to situate your research within existing knowledge. The literature review gives you a chance to:
- Demonstrate your familiarity with the topic and its scholarly context
- Develop a theoretical framework and methodology for your research
- Position your work in relation to other researchers and theorists
- Show how your research addresses a gap or contributes to a debate
- Evaluate the current state of research and demonstrate your knowledge of the scholarly debates around your topic.
Writing literature reviews is a particularly important skill if you want to apply for graduate school or pursue a career in research. We’ve written a step-by-step guide that you can follow below.
Receive feedback on language, structure, and formatting
Professional editors proofread and edit your paper by focusing on:
- Academic style
- Vague sentences
- Style consistency
See an example

Writing literature reviews can be quite challenging! A good starting point could be to look at some examples, depending on what kind of literature review you’d like to write.
- Example literature review #1: “Why Do People Migrate? A Review of the Theoretical Literature” ( Theoretical literature review about the development of economic migration theory from the 1950s to today.)
- Example literature review #2: “Literature review as a research methodology: An overview and guidelines” ( Methodological literature review about interdisciplinary knowledge acquisition and production.)
- Example literature review #3: “The Use of Technology in English Language Learning: A Literature Review” ( Thematic literature review about the effects of technology on language acquisition.)
- Example literature review #4: “Learners’ Listening Comprehension Difficulties in English Language Learning: A Literature Review” ( Chronological literature review about how the concept of listening skills has changed over time.)
You can also check out our templates with literature review examples and sample outlines at the links below.
Download Word doc Download Google doc
Before you begin searching for literature, you need a clearly defined topic .
If you are writing the literature review section of a dissertation or research paper, you will search for literature related to your research problem and questions .
Make a list of keywords
Start by creating a list of keywords related to your research question. Include each of the key concepts or variables you’re interested in, and list any synonyms and related terms. You can add to this list as you discover new keywords in the process of your literature search.
- Social media, Facebook, Instagram, Twitter, Snapchat, TikTok
- Body image, self-perception, self-esteem, mental health
- Generation Z, teenagers, adolescents, youth
Search for relevant sources
Use your keywords to begin searching for sources. Some useful databases to search for journals and articles include:
- Your university’s library catalogue
- Google Scholar
- Project Muse (humanities and social sciences)
- Medline (life sciences and biomedicine)
- EconLit (economics)
- Inspec (physics, engineering and computer science)
You can also use boolean operators to help narrow down your search.
Make sure to read the abstract to find out whether an article is relevant to your question. When you find a useful book or article, you can check the bibliography to find other relevant sources.
You likely won’t be able to read absolutely everything that has been written on your topic, so it will be necessary to evaluate which sources are most relevant to your research question.
For each publication, ask yourself:
- What question or problem is the author addressing?
- What are the key concepts and how are they defined?
- What are the key theories, models, and methods?
- Does the research use established frameworks or take an innovative approach?
- What are the results and conclusions of the study?
- How does the publication relate to other literature in the field? Does it confirm, add to, or challenge established knowledge?
- What are the strengths and weaknesses of the research?
Make sure the sources you use are credible , and make sure you read any landmark studies and major theories in your field of research.
You can use our template to summarize and evaluate sources you’re thinking about using. Click on either button below to download.
Take notes and cite your sources
As you read, you should also begin the writing process. Take notes that you can later incorporate into the text of your literature review.
It is important to keep track of your sources with citations to avoid plagiarism . It can be helpful to make an annotated bibliography , where you compile full citation information and write a paragraph of summary and analysis for each source. This helps you remember what you read and saves time later in the process.
To begin organizing your literature review’s argument and structure, be sure you understand the connections and relationships between the sources you’ve read. Based on your reading and notes, you can look for:
- Trends and patterns (in theory, method or results): do certain approaches become more or less popular over time?
- Themes: what questions or concepts recur across the literature?
- Debates, conflicts and contradictions: where do sources disagree?
- Pivotal publications: are there any influential theories or studies that changed the direction of the field?
- Gaps: what is missing from the literature? Are there weaknesses that need to be addressed?
This step will help you work out the structure of your literature review and (if applicable) show how your own research will contribute to existing knowledge.
- Most research has focused on young women.
- There is an increasing interest in the visual aspects of social media.
- But there is still a lack of robust research on highly visual platforms like Instagram and Snapchat—this is a gap that you could address in your own research.
There are various approaches to organizing the body of a literature review. Depending on the length of your literature review, you can combine several of these strategies (for example, your overall structure might be thematic, but each theme is discussed chronologically).
Chronological
The simplest approach is to trace the development of the topic over time. However, if you choose this strategy, be careful to avoid simply listing and summarizing sources in order.
Try to analyze patterns, turning points and key debates that have shaped the direction of the field. Give your interpretation of how and why certain developments occurred.
If you have found some recurring central themes, you can organize your literature review into subsections that address different aspects of the topic.
For example, if you are reviewing literature about inequalities in migrant health outcomes, key themes might include healthcare policy, language barriers, cultural attitudes, legal status, and economic access.
Methodological
If you draw your sources from different disciplines or fields that use a variety of research methods , you might want to compare the results and conclusions that emerge from different approaches. For example:
- Look at what results have emerged in qualitative versus quantitative research
- Discuss how the topic has been approached by empirical versus theoretical scholarship
- Divide the literature into sociological, historical, and cultural sources
Theoretical
A literature review is often the foundation for a theoretical framework . You can use it to discuss various theories, models, and definitions of key concepts.
You might argue for the relevance of a specific theoretical approach, or combine various theoretical concepts to create a framework for your research.
Like any other academic text , your literature review should have an introduction , a main body, and a conclusion . What you include in each depends on the objective of your literature review.
The introduction should clearly establish the focus and purpose of the literature review.
Depending on the length of your literature review, you might want to divide the body into subsections. You can use a subheading for each theme, time period, or methodological approach.
As you write, you can follow these tips:
- Summarize and synthesize: give an overview of the main points of each source and combine them into a coherent whole
- Analyze and interpret: don’t just paraphrase other researchers — add your own interpretations where possible, discussing the significance of findings in relation to the literature as a whole
- Critically evaluate: mention the strengths and weaknesses of your sources
- Write in well-structured paragraphs: use transition words and topic sentences to draw connections, comparisons and contrasts
In the conclusion, you should summarize the key findings you have taken from the literature and emphasize their significance.
When you’ve finished writing and revising your literature review, don’t forget to proofread thoroughly before submitting. Not a language expert? Check out Scribbr’s professional proofreading services !
This article has been adapted into lecture slides that you can use to teach your students about writing a literature review.
Scribbr slides are free to use, customize, and distribute for educational purposes.
Open Google Slides Download PowerPoint
If you want to know more about the research process , methodology , research bias , or statistics , make sure to check out some of our other articles with explanations and examples.
- Sampling methods
- Simple random sampling
- Stratified sampling
- Cluster sampling
- Likert scales
- Reproducibility
Statistics
- Null hypothesis
- Statistical power
- Probability distribution
- Effect size
- Poisson distribution
Research bias
- Optimism bias
- Cognitive bias
- Implicit bias
- Hawthorne effect
- Anchoring bias
- Explicit bias
A literature review is a survey of scholarly sources (such as books, journal articles, and theses) related to a specific topic or research question .
It is often written as part of a thesis, dissertation , or research paper , in order to situate your work in relation to existing knowledge.
There are several reasons to conduct a literature review at the beginning of a research project:
- To familiarize yourself with the current state of knowledge on your topic
- To ensure that you’re not just repeating what others have already done
- To identify gaps in knowledge and unresolved problems that your research can address
- To develop your theoretical framework and methodology
- To provide an overview of the key findings and debates on the topic
Writing the literature review shows your reader how your work relates to existing research and what new insights it will contribute.
The literature review usually comes near the beginning of your thesis or dissertation . After the introduction , it grounds your research in a scholarly field and leads directly to your theoretical framework or methodology .
A literature review is a survey of credible sources on a topic, often used in dissertations , theses, and research papers . Literature reviews give an overview of knowledge on a subject, helping you identify relevant theories and methods, as well as gaps in existing research. Literature reviews are set up similarly to other academic texts , with an introduction , a main body, and a conclusion .
An annotated bibliography is a list of source references that has a short description (called an annotation ) for each of the sources. It is often assigned as part of the research process for a paper .
Cite this Scribbr article
If you want to cite this source, you can copy and paste the citation or click the “Cite this Scribbr article” button to automatically add the citation to our free Citation Generator.
McCombes, S. (2023, September 11). How to Write a Literature Review | Guide, Examples, & Templates. Scribbr. Retrieved September 16, 2024, from https://www.scribbr.com/dissertation/literature-review/
Is this article helpful?
Shona McCombes
Other students also liked, what is a theoretical framework | guide to organizing, what is a research methodology | steps & tips, how to write a research proposal | examples & templates, get unlimited documents corrected.
✔ Free APA citation check included ✔ Unlimited document corrections ✔ Specialized in correcting academic texts
- UConn Library
- Literature Review: The What, Why and How-to Guide
- Introduction
Literature Review: The What, Why and How-to Guide — Introduction
- Getting Started
- How to Pick a Topic
- Strategies to Find Sources
- Evaluating Sources & Lit. Reviews
- Tips for Writing Literature Reviews
- Writing Literature Review: Useful Sites
- Citation Resources
- Other Academic Writings
What are Literature Reviews?
So, what is a literature review? "A literature review is an account of what has been published on a topic by accredited scholars and researchers. In writing the literature review, your purpose is to convey to your reader what knowledge and ideas have been established on a topic, and what their strengths and weaknesses are. As a piece of writing, the literature review must be defined by a guiding concept (e.g., your research objective, the problem or issue you are discussing, or your argumentative thesis). It is not just a descriptive list of the material available, or a set of summaries." Taylor, D. The literature review: A few tips on conducting it . University of Toronto Health Sciences Writing Centre.
Goals of Literature Reviews
What are the goals of creating a Literature Review? A literature could be written to accomplish different aims:
- To develop a theory or evaluate an existing theory
- To summarize the historical or existing state of a research topic
- Identify a problem in a field of research
Baumeister, R. F., & Leary, M. R. (1997). Writing narrative literature reviews . Review of General Psychology , 1 (3), 311-320.
What kinds of sources require a Literature Review?
- A research paper assigned in a course
- A thesis or dissertation
- A grant proposal
- An article intended for publication in a journal
All these instances require you to collect what has been written about your research topic so that you can demonstrate how your own research sheds new light on the topic.
Types of Literature Reviews
What kinds of literature reviews are written?
Narrative review: The purpose of this type of review is to describe the current state of the research on a specific topic/research and to offer a critical analysis of the literature reviewed. Studies are grouped by research/theoretical categories, and themes and trends, strengths and weakness, and gaps are identified. The review ends with a conclusion section which summarizes the findings regarding the state of the research of the specific study, the gaps identify and if applicable, explains how the author's research will address gaps identify in the review and expand the knowledge on the topic reviewed.
- Example : Predictors and Outcomes of U.S. Quality Maternity Leave: A Review and Conceptual Framework: 10.1177/08948453211037398
Systematic review : "The authors of a systematic review use a specific procedure to search the research literature, select the studies to include in their review, and critically evaluate the studies they find." (p. 139). Nelson, L. K. (2013). Research in Communication Sciences and Disorders . Plural Publishing.
- Example : The effect of leave policies on increasing fertility: a systematic review: 10.1057/s41599-022-01270-w
Meta-analysis : "Meta-analysis is a method of reviewing research findings in a quantitative fashion by transforming the data from individual studies into what is called an effect size and then pooling and analyzing this information. The basic goal in meta-analysis is to explain why different outcomes have occurred in different studies." (p. 197). Roberts, M. C., & Ilardi, S. S. (2003). Handbook of Research Methods in Clinical Psychology . Blackwell Publishing.
- Example : Employment Instability and Fertility in Europe: A Meta-Analysis: 10.1215/00703370-9164737
Meta-synthesis : "Qualitative meta-synthesis is a type of qualitative study that uses as data the findings from other qualitative studies linked by the same or related topic." (p.312). Zimmer, L. (2006). Qualitative meta-synthesis: A question of dialoguing with texts . Journal of Advanced Nursing , 53 (3), 311-318.
- Example : Women’s perspectives on career successes and barriers: A qualitative meta-synthesis: 10.1177/05390184221113735
Literature Reviews in the Health Sciences
- UConn Health subject guide on systematic reviews Explanation of the different review types used in health sciences literature as well as tools to help you find the right review type
- << Previous: Getting Started
- Next: How to Pick a Topic >>
- Last Updated: Sep 21, 2022 2:16 PM
- URL: https://guides.lib.uconn.edu/literaturereview
Reference management. Clean and simple.
What is a literature review? [with examples]

What is a literature review?
The purpose of a literature review, how to write a literature review, the format of a literature review, general formatting rules, the length of a literature review, literature review examples, frequently asked questions about literature reviews, related articles.
A literature review is an assessment of the sources in a chosen topic of research.
In a literature review, you’re expected to report on the existing scholarly conversation, without adding new contributions.
If you are currently writing one, you've come to the right place. In the following paragraphs, we will explain:
- the objective of a literature review
- how to write a literature review
- the basic format of a literature review
Tip: It’s not always mandatory to add a literature review in a paper. Theses and dissertations often include them, whereas research papers may not. Make sure to consult with your instructor for exact requirements.
The four main objectives of a literature review are:
- Studying the references of your research area
- Summarizing the main arguments
- Identifying current gaps, stances, and issues
- Presenting all of the above in a text
Ultimately, the main goal of a literature review is to provide the researcher with sufficient knowledge about the topic in question so that they can eventually make an intervention.
The format of a literature review is fairly standard. It includes an:
- introduction that briefly introduces the main topic
- body that includes the main discussion of the key arguments
- conclusion that highlights the gaps and issues of the literature
➡️ Take a look at our guide on how to write a literature review to learn more about how to structure a literature review.
First of all, a literature review should have its own labeled section. You should indicate clearly in the table of contents where the literature can be found, and you should label this section as “Literature Review.”
➡️ For more information on writing a thesis, visit our guide on how to structure a thesis .
There is no set amount of words for a literature review, so the length depends on the research. If you are working with a large amount of sources, it will be long. If your paper does not depend entirely on references, it will be short.
Take a look at these three theses featuring great literature reviews:
- School-Based Speech-Language Pathologist's Perceptions of Sensory Food Aversions in Children [ PDF , see page 20]
- Who's Writing What We Read: Authorship in Criminological Research [ PDF , see page 4]
- A Phenomenological Study of the Lived Experience of Online Instructors of Theological Reflection at Christian Institutions Accredited by the Association of Theological Schools [ PDF , see page 56]
Literature reviews are most commonly found in theses and dissertations. However, you find them in research papers as well.
There is no set amount of words for a literature review, so the length depends on the research. If you are working with a large amount of sources, then it will be long. If your paper does not depend entirely on references, then it will be short.
No. A literature review should have its own independent section. You should indicate clearly in the table of contents where the literature review can be found, and label this section as “Literature Review.”
The main goal of a literature review is to provide the researcher with sufficient knowledge about the topic in question so that they can eventually make an intervention.

- University of Texas Libraries
Literature Reviews
- What is a literature review?
- Steps in the Literature Review Process
- Define your research question
- Determine inclusion and exclusion criteria
- Choose databases and search
- Review Results
- Synthesize Results
- Analyze Results
- Librarian Support
- Artificial Intelligence (AI) Tools
What is a Literature Review?
A literature or narrative review is a comprehensive review and analysis of the published literature on a specific topic or research question. The literature that is reviewed contains: books, articles, academic articles, conference proceedings, association papers, and dissertations. It contains the most pertinent studies and points to important past and current research and practices. It provides background and context, and shows how your research will contribute to the field.
A literature review should:
- Provide a comprehensive and updated review of the literature;
- Explain why this review has taken place;
- Articulate a position or hypothesis;
- Acknowledge and account for conflicting and corroborating points of view
From S age Research Methods
Purpose of a Literature Review
A literature review can be written as an introduction to a study to:
- Demonstrate how a study fills a gap in research
- Compare a study with other research that's been done
Or it can be a separate work (a research article on its own) which:
- Organizes or describes a topic
- Describes variables within a particular issue/problem
Limitations of a Literature Review
Some of the limitations of a literature review are:
- It's a snapshot in time. Unlike other reviews, this one has beginning, a middle and an end. There may be future developments that could make your work less relevant.
- It may be too focused. Some niche studies may miss the bigger picture.
- It can be difficult to be comprehensive. There is no way to make sure all the literature on a topic was considered.
- It is easy to be biased if you stick to top tier journals. There may be other places where people are publishing exemplary research. Look to open access publications and conferences to reflect a more inclusive collection. Also, make sure to include opposing views (and not just supporting evidence).
Source: Grant, Maria J., and Andrew Booth. “A Typology of Reviews: An Analysis of 14 Review Types and Associated Methodologies.” Health Information & Libraries Journal, vol. 26, no. 2, June 2009, pp. 91–108. Wiley Online Library, doi:10.1111/j.1471-1842.2009.00848.x.
Librarian Assistance
For help, please contact the librarian for your subject area. We have a guide to library specialists by subject .
- Last Updated: Aug 26, 2024 5:59 AM
- URL: https://guides.lib.utexas.edu/literaturereviews


Literature Review - what is a Literature Review, why it is important and how it is done
What are literature reviews, goals of literature reviews, types of literature reviews, about this guide/licence.
- Strategies to Find Sources
- Evaluating Literature Reviews and Sources
- Tips for Writing Literature Reviews
- Writing Literature Review: Useful Sites
- Citation Resources
- Other Academic Writings
- Useful Resources
Help is Just a Click Away
Search our FAQ Knowledge base, ask a question, chat, send comments...
Go to LibAnswers
What is a literature review? "A literature review is an account of what has been published on a topic by accredited scholars and researchers. In writing the literature review, your purpose is to convey to your reader what knowledge and ideas have been established on a topic, and what their strengths and weaknesses are. As a piece of writing, the literature review must be defined by a guiding concept (e.g., your research objective, the problem or issue you are discussing, or your argumentative thesis). It is not just a descriptive list of the material available, or a set of summaries. " - Quote from Taylor, D. (n.d) "The literature review: A few tips on conducting it"
Source NC State University Libraries. This video is published under a Creative Commons 3.0 BY-NC-SA US license.
What are the goals of creating a Literature Review?
- To develop a theory or evaluate an existing theory
- To summarize the historical or existing state of a research topic
- Identify a problem in a field of research
- Baumeister, R.F. & Leary, M.R. (1997). "Writing narrative literature reviews," Review of General Psychology , 1(3), 311-320.
When do you need to write a Literature Review?
- When writing a prospectus or a thesis/dissertation
- When writing a research paper
- When writing a grant proposal
In all these cases you need to dedicate a chapter in these works to showcase what have been written about your research topic and to point out how your own research will shed a new light into these body of scholarship.
Literature reviews are also written as standalone articles as a way to survey a particular research topic in-depth. This type of literature reviews look at a topic from a historical perspective to see how the understanding of the topic have change through time.
What kinds of literature reviews are written?
- Narrative Review: The purpose of this type of review is to describe the current state of the research on a specific topic/research and to offer a critical analysis of the literature reviewed. Studies are grouped by research/theoretical categories, and themes and trends, strengths and weakness, and gaps are identified. The review ends with a conclusion section which summarizes the findings regarding the state of the research of the specific study, the gaps identify and if applicable, explains how the author's research will address gaps identify in the review and expand the knowledge on the topic reviewed.
- Book review essays/ Historiographical review essays : This is a type of review that focus on a small set of research books on a particular topic " to locate these books within current scholarship, critical methodologies, and approaches" in the field. - LARR
- Systematic review : "The authors of a systematic review use a specific procedure to search the research literature, select the studies to include in their review, and critically evaluate the studies they find." (p. 139). Nelson, L.K. (2013). Research in Communication Sciences and Disorders . San Diego, CA: Plural Publishing.
- Meta-analysis : "Meta-analysis is a method of reviewing research findings in a quantitative fashion by transforming the data from individual studies into what is called an effect size and then pooling and analyzing this information. The basic goal in meta-analysis is to explain why different outcomes have occurred in different studies." (p. 197). Roberts, M.C. & Ilardi, S.S. (2003). Handbook of Research Methods in Clinical Psychology . Malden, MA: Blackwell Pub.
- Meta-synthesis : "Qualitative meta-synthesis is a type of qualitative study that uses as data the findings from other qualitative studies linked by the same or related topic." (p.312). Zimmer, L. (2006). "Qualitative meta-synthesis: A question of dialoguing with texts," Journal of Advanced Nursing , 53(3), 311-318.
Guide adapted from "Literature Review" , a guide developed by Marisol Ramos used under CC BY 4.0 /modified from original.
- Next: Strategies to Find Sources >>
- Last Updated: Jul 3, 2024 10:56 AM
- URL: https://lit.libguides.com/Literature-Review
The Library, Technological University of the Shannon: Midwest
Libraries | Research Guides
Literature reviews, what is a literature review, learning more about how to do a literature review.
- Planning the Review
- The Research Question
- Choosing Where to Search
- Organizing the Review
- Writing the Review
A literature review is a review and synthesis of existing research on a topic or research question. A literature review is meant to analyze the scholarly literature, make connections across writings and identify strengths, weaknesses, trends, and missing conversations. A literature review should address different aspects of a topic as it relates to your research question. A literature review goes beyond a description or summary of the literature you have read.
- Sage Research Methods Core This link opens in a new window SAGE Research Methods supports research at all levels by providing material to guide users through every step of the research process. SAGE Research Methods is the ultimate methods library with more than 1000 books, reference works, journal articles, and instructional videos by world-leading academics from across the social sciences, including the largest collection of qualitative methods books available online from any scholarly publisher. – Publisher
- Next: Planning the Review >>
- Last Updated: Jul 8, 2024 11:22 AM
- URL: https://libguides.northwestern.edu/literaturereviews
Service update: Some parts of the Library’s website will be down for maintenance on August 11.
Secondary menu
- Log in to your Library account
- Hours and Maps
- Connect from Off Campus
- UC Berkeley Home
Search form
Conducting a literature review: why do a literature review, why do a literature review.
- How To Find "The Literature"
- Found it -- Now What?
Besides the obvious reason for students -- because it is assigned! -- a literature review helps you explore the research that has come before you, to see how your research question has (or has not) already been addressed.
You identify:
- core research in the field
- experts in the subject area
- methodology you may want to use (or avoid)
- gaps in knowledge -- or where your research would fit in
It Also Helps You:
- Publish and share your findings
- Justify requests for grants and other funding
- Identify best practices to inform practice
- Set wider context for a program evaluation
- Compile information to support community organizing
Great brief overview, from NCSU
Want To Know More?
- Next: How To Find "The Literature" >>
- Last Updated: Apr 25, 2024 1:10 PM
- URL: https://guides.lib.berkeley.edu/litreview

What Is A Literature Review?
A plain-language explainer (with examples).
By: Derek Jansen (MBA) & Kerryn Warren (PhD) | June 2020 (Updated May 2023)
If you’re faced with writing a dissertation or thesis, chances are you’ve encountered the term “literature review” . If you’re on this page, you’re probably not 100% what the literature review is all about. The good news is that you’ve come to the right place.
Literature Review 101
- What (exactly) is a literature review
- What’s the purpose of the literature review chapter
- How to find high-quality resources
- How to structure your literature review chapter
- Example of an actual literature review
What is a literature review?
The word “literature review” can refer to two related things that are part of the broader literature review process. The first is the task of reviewing the literature – i.e. sourcing and reading through the existing research relating to your research topic. The second is the actual chapter that you write up in your dissertation, thesis or research project. Let’s look at each of them:
Reviewing the literature
The first step of any literature review is to hunt down and read through the existing research that’s relevant to your research topic. To do this, you’ll use a combination of tools (we’ll discuss some of these later) to find journal articles, books, ebooks, research reports, dissertations, theses and any other credible sources of information that relate to your topic. You’ll then summarise and catalogue these for easy reference when you write up your literature review chapter.
The literature review chapter
The second step of the literature review is to write the actual literature review chapter (this is usually the second chapter in a typical dissertation or thesis structure ). At the simplest level, the literature review chapter is an overview of the key literature that’s relevant to your research topic. This chapter should provide a smooth-flowing discussion of what research has already been done, what is known, what is unknown and what is contested in relation to your research topic. So, you can think of it as an integrated review of the state of knowledge around your research topic.

What’s the purpose of a literature review?
The literature review chapter has a few important functions within your dissertation, thesis or research project. Let’s take a look at these:
Purpose #1 – Demonstrate your topic knowledge
The first function of the literature review chapter is, quite simply, to show the reader (or marker) that you know what you’re talking about . In other words, a good literature review chapter demonstrates that you’ve read the relevant existing research and understand what’s going on – who’s said what, what’s agreed upon, disagreed upon and so on. This needs to be more than just a summary of who said what – it needs to integrate the existing research to show how it all fits together and what’s missing (which leads us to purpose #2, next).
Purpose #2 – Reveal the research gap that you’ll fill
The second function of the literature review chapter is to show what’s currently missing from the existing research, to lay the foundation for your own research topic. In other words, your literature review chapter needs to show that there are currently “missing pieces” in terms of the bigger puzzle, and that your study will fill one of those research gaps . By doing this, you are showing that your research topic is original and will help contribute to the body of knowledge. In other words, the literature review helps justify your research topic.
Purpose #3 – Lay the foundation for your conceptual framework
The third function of the literature review is to form the basis for a conceptual framework . Not every research topic will necessarily have a conceptual framework, but if your topic does require one, it needs to be rooted in your literature review.
For example, let’s say your research aims to identify the drivers of a certain outcome – the factors which contribute to burnout in office workers. In this case, you’d likely develop a conceptual framework which details the potential factors (e.g. long hours, excessive stress, etc), as well as the outcome (burnout). Those factors would need to emerge from the literature review chapter – they can’t just come from your gut!
So, in this case, the literature review chapter would uncover each of the potential factors (based on previous studies about burnout), which would then be modelled into a framework.
Purpose #4 – To inform your methodology
The fourth function of the literature review is to inform the choice of methodology for your own research. As we’ve discussed on the Grad Coach blog , your choice of methodology will be heavily influenced by your research aims, objectives and questions . Given that you’ll be reviewing studies covering a topic close to yours, it makes sense that you could learn a lot from their (well-considered) methodologies.
So, when you’re reviewing the literature, you’ll need to pay close attention to the research design , methodology and methods used in similar studies, and use these to inform your methodology. Quite often, you’ll be able to “borrow” from previous studies . This is especially true for quantitative studies , as you can use previously tried and tested measures and scales.

How do I find articles for my literature review?
Finding quality journal articles is essential to crafting a rock-solid literature review. As you probably already know, not all research is created equally, and so you need to make sure that your literature review is built on credible research .
We could write an entire post on how to find quality literature (actually, we have ), but a good starting point is Google Scholar . Google Scholar is essentially the academic equivalent of Google, using Google’s powerful search capabilities to find relevant journal articles and reports. It certainly doesn’t cover every possible resource, but it’s a very useful way to get started on your literature review journey, as it will very quickly give you a good indication of what the most popular pieces of research are in your field.
One downside of Google Scholar is that it’s merely a search engine – that is, it lists the articles, but oftentimes it doesn’t host the articles . So you’ll often hit a paywall when clicking through to journal websites.
Thankfully, your university should provide you with access to their library, so you can find the article titles using Google Scholar and then search for them by name in your university’s online library. Your university may also provide you with access to ResearchGate , which is another great source for existing research.
Remember, the correct search keywords will be super important to get the right information from the start. So, pay close attention to the keywords used in the journal articles you read and use those keywords to search for more articles. If you can’t find a spoon in the kitchen, you haven’t looked in the right drawer.
Need a helping hand?
How should I structure my literature review?
Unfortunately, there’s no generic universal answer for this one. The structure of your literature review will depend largely on your topic area and your research aims and objectives.
You could potentially structure your literature review chapter according to theme, group, variables , chronologically or per concepts in your field of research. We explain the main approaches to structuring your literature review here . You can also download a copy of our free literature review template to help you establish an initial structure.
In general, it’s also a good idea to start wide (i.e. the big-picture-level) and then narrow down, ending your literature review close to your research questions . However, there’s no universal one “right way” to structure your literature review. The most important thing is not to discuss your sources one after the other like a list – as we touched on earlier, your literature review needs to synthesise the research , not summarise it .
Ultimately, you need to craft your literature review so that it conveys the most important information effectively – it needs to tell a logical story in a digestible way. It’s no use starting off with highly technical terms and then only explaining what these terms mean later. Always assume your reader is not a subject matter expert and hold their hand through a journe y of the literature while keeping the functions of the literature review chapter (which we discussed earlier) front of mind.

Example of a literature review
In the video below, we walk you through a high-quality literature review from a dissertation that earned full distinction. This will give you a clearer view of what a strong literature review looks like in practice and hopefully provide some inspiration for your own.
Wrapping Up
In this post, we’ve (hopefully) answered the question, “ what is a literature review? “. We’ve also considered the purpose and functions of the literature review, as well as how to find literature and how to structure the literature review chapter. If you’re keen to learn more, check out the literature review section of the Grad Coach blog , as well as our detailed video post covering how to write a literature review .

Psst… there’s more!
This post is an extract from our bestselling short course, Literature Review Bootcamp . If you want to work smart, you don't want to miss this .
16 Comments
Thanks for this review. It narrates what’s not been taught as tutors are always in a early to finish their classes.
Thanks for the kind words, Becky. Good luck with your literature review 🙂
This website is amazing, it really helps break everything down. Thank you, I would have been lost without it.
This is review is amazing. I benefited from it a lot and hope others visiting this website will benefit too.
Timothy T. Chol [email protected]
Thank you very much for the guiding in literature review I learn and benefited a lot this make my journey smooth I’ll recommend this site to my friends
This was so useful. Thank you so much.
Hi, Concept was explained nicely by both of you. Thanks a lot for sharing it. It will surely help research scholars to start their Research Journey.
The review is really helpful to me especially during this period of covid-19 pandemic when most universities in my country only offer online classes. Great stuff
Great Brief Explanation, thanks
So helpful to me as a student
GradCoach is a fantastic site with brilliant and modern minds behind it.. I spent weeks decoding the substantial academic Jargon and grounding my initial steps on the research process, which could be shortened to a couple of days through the Gradcoach. Thanks again!
This is an amazing talk. I paved way for myself as a researcher. Thank you GradCoach!
Well-presented overview of the literature!
This was brilliant. So clear. Thank you
Submit a Comment Cancel reply
Your email address will not be published. Required fields are marked *
Save my name, email, and website in this browser for the next time I comment.
- Print Friendly
- Library Homepage
Literature Review: The What, Why and How-to Guide: Literature Reviews?
- Literature Reviews?
- Strategies to Finding Sources
- Keeping up with Research!
- Evaluating Sources & Literature Reviews
- Organizing for Writing
- Writing Literature Review
- Other Academic Writings
What is a Literature Review?
So, what is a literature review .
"A literature review is an account of what has been published on a topic by accredited scholars and researchers. In writing the literature review, your purpose is to convey to your reader what knowledge and ideas have been established on a topic, and what their strengths and weaknesses are. As a piece of writing, the literature review must be defined by a guiding concept (e.g., your research objective, the problem or issue you are discussing, or your argumentative thesis). It is not just a descriptive list of the material available or a set of summaries." - Quote from Taylor, D. (n.d)."The Literature Review: A Few Tips on Conducting it".
- Citation: "The Literature Review: A Few Tips on Conducting it"
What kinds of literature reviews are written?
Each field has a particular way to do reviews for academic research literature. In the social sciences and humanities the most common are:
- Narrative Reviews: The purpose of this type of review is to describe the current state of the research on a specific research topic and to offer a critical analysis of the literature reviewed. Studies are grouped by research/theoretical categories, and themes and trends, strengths and weaknesses, and gaps are identified. The review ends with a conclusion section that summarizes the findings regarding the state of the research of the specific study, the gaps identify and if applicable, explains how the author's research will address gaps identify in the review and expand the knowledge on the topic reviewed.
- Book review essays/ Historiographical review essays : A type of literature review typical in History and related fields, e.g., Latin American studies. For example, the Latin American Research Review explains that the purpose of this type of review is to “(1) to familiarize readers with the subject, approach, arguments, and conclusions found in a group of books whose common focus is a historical period; a country or region within Latin America; or a practice, development, or issue of interest to specialists and others; (2) to locate these books within current scholarship, critical methodologies, and approaches; and (3) to probe the relation of these new books to previous work on the subject, especially canonical texts. Unlike individual book reviews, the cluster reviews found in LARR seek to address the state of the field or discipline and not solely the works at issue.” - LARR
What are the Goals of Creating a Literature Review?
- To develop a theory or evaluate an existing theory
- To summarize the historical or existing state of a research topic
- Identify a problem in a field of research
- Baumeister, R.F. & Leary, M.R. (1997). "Writing narrative literature reviews," Review of General Psychology , 1(3), 311-320.
When do you need to write a Literature Review?
- When writing a prospectus or a thesis/dissertation
- When writing a research paper
- When writing a grant proposal
In all these cases you need to dedicate a chapter in these works to showcase what has been written about your research topic and to point out how your own research will shed new light into a body of scholarship.
Where I can find examples of Literature Reviews?
Note: In the humanities, even if they don't use the term "literature review", they may have a dedicated chapter that reviewed the "critical bibliography" or they incorporated that review in the introduction or first chapter of the dissertation, book, or article.
- UCSB electronic theses and dissertations In partnership with the Graduate Division, the UC Santa Barbara Library is making available theses and dissertations produced by UCSB students. Currently included in ADRL are theses and dissertations that were originally filed electronically, starting in 2011. In future phases of ADRL, all theses and dissertations created by UCSB students may be digitized and made available.
Where to Find Standalone Literature Reviews
Literature reviews are also written as standalone articles as a way to survey a particular research topic in-depth. This type of literature review looks at a topic from a historical perspective to see how the understanding of the topic has changed over time.
- Find e-Journals for Standalone Literature Reviews The best way to get familiar with and to learn how to write literature reviews is by reading them. You can use our Journal Search option to find journals that specialize in publishing literature reviews from major disciplines like anthropology, sociology, etc. Usually these titles are called, "Annual Review of [discipline name] OR [Discipline name] Review. This option works best if you know the title of the publication you are looking for. Below are some examples of these journals! more... less... Journal Search can be found by hovering over the link for Research on the library website.
Social Sciences
- Annual Review of Anthropology
- Annual Review of Political Science
- Annual Review of Sociology
- Ethnic Studies Review
Hard science and health sciences:
- Annual Review of Biomedical Data Science
- Annual Review of Materials Science
- Systematic Review From journal site: "The journal Systematic Reviews encompasses all aspects of the design, conduct, and reporting of systematic reviews" in the health sciences.
- << Previous: Overview
- Next: Strategies to Finding Sources >>
- Last Updated: Mar 5, 2024 11:44 AM
- URL: https://guides.library.ucsb.edu/litreview

What is a Literature Review? How to Write It (with Examples)

A literature review is a critical analysis and synthesis of existing research on a particular topic. It provides an overview of the current state of knowledge, identifies gaps, and highlights key findings in the literature. 1 The purpose of a literature review is to situate your own research within the context of existing scholarship, demonstrating your understanding of the topic and showing how your work contributes to the ongoing conversation in the field. Learning how to write a literature review is a critical tool for successful research. Your ability to summarize and synthesize prior research pertaining to a certain topic demonstrates your grasp on the topic of study, and assists in the learning process.
Table of Contents
What is the purpose of literature review , a. habitat loss and species extinction: , b. range shifts and phenological changes: , c. ocean acidification and coral reefs: , d. adaptive strategies and conservation efforts: .
- Choose a Topic and Define the Research Question:
- Decide on the Scope of Your Review:
- Select Databases for Searches:
- Conduct Searches and Keep Track:
- Review the Literature:
- Organize and Write Your Literature Review:
- How to write a literature review faster with Paperpal?
Frequently asked questions
What is a literature review .
A well-conducted literature review demonstrates the researcher’s familiarity with the existing literature, establishes the context for their own research, and contributes to scholarly conversations on the topic. One of the purposes of a literature review is also to help researchers avoid duplicating previous work and ensure that their research is informed by and builds upon the existing body of knowledge.

A literature review serves several important purposes within academic and research contexts. Here are some key objectives and functions of a literature review: 2
1. Contextualizing the Research Problem: The literature review provides a background and context for the research problem under investigation. It helps to situate the study within the existing body of knowledge.
2. Identifying Gaps in Knowledge: By identifying gaps, contradictions, or areas requiring further research, the researcher can shape the research question and justify the significance of the study. This is crucial for ensuring that the new research contributes something novel to the field.
Find academic papers related to your research topic faster. Try Research on Paperpal
3. Understanding Theoretical and Conceptual Frameworks: Literature reviews help researchers gain an understanding of the theoretical and conceptual frameworks used in previous studies. This aids in the development of a theoretical framework for the current research.
4. Providing Methodological Insights: Another purpose of literature reviews is that it allows researchers to learn about the methodologies employed in previous studies. This can help in choosing appropriate research methods for the current study and avoiding pitfalls that others may have encountered.
5. Establishing Credibility: A well-conducted literature review demonstrates the researcher’s familiarity with existing scholarship, establishing their credibility and expertise in the field. It also helps in building a solid foundation for the new research.
6. Informing Hypotheses or Research Questions: The literature review guides the formulation of hypotheses or research questions by highlighting relevant findings and areas of uncertainty in existing literature.
Literature review example
Let’s delve deeper with a literature review example: Let’s say your literature review is about the impact of climate change on biodiversity. You might format your literature review into sections such as the effects of climate change on habitat loss and species extinction, phenological changes, and marine biodiversity. Each section would then summarize and analyze relevant studies in those areas, highlighting key findings and identifying gaps in the research. The review would conclude by emphasizing the need for further research on specific aspects of the relationship between climate change and biodiversity. The following literature review template provides a glimpse into the recommended literature review structure and content, demonstrating how research findings are organized around specific themes within a broader topic.
Literature Review on Climate Change Impacts on Biodiversity:
Climate change is a global phenomenon with far-reaching consequences, including significant impacts on biodiversity. This literature review synthesizes key findings from various studies:
Climate change-induced alterations in temperature and precipitation patterns contribute to habitat loss, affecting numerous species (Thomas et al., 2004). The review discusses how these changes increase the risk of extinction, particularly for species with specific habitat requirements.
Observations of range shifts and changes in the timing of biological events (phenology) are documented in response to changing climatic conditions (Parmesan & Yohe, 2003). These shifts affect ecosystems and may lead to mismatches between species and their resources.
The review explores the impact of climate change on marine biodiversity, emphasizing ocean acidification’s threat to coral reefs (Hoegh-Guldberg et al., 2007). Changes in pH levels negatively affect coral calcification, disrupting the delicate balance of marine ecosystems.
Recognizing the urgency of the situation, the literature review discusses various adaptive strategies adopted by species and conservation efforts aimed at mitigating the impacts of climate change on biodiversity (Hannah et al., 2007). It emphasizes the importance of interdisciplinary approaches for effective conservation planning.
Strengthen your literature review with factual insights. Try Research on Paperpal for free!
How to write a good literature review
Writing a literature review involves summarizing and synthesizing existing research on a particular topic. A good literature review format should include the following elements.
Introduction: The introduction sets the stage for your literature review, providing context and introducing the main focus of your review.
- Opening Statement: Begin with a general statement about the broader topic and its significance in the field.
- Scope and Purpose: Clearly define the scope of your literature review. Explain the specific research question or objective you aim to address.
- Organizational Framework: Briefly outline the structure of your literature review, indicating how you will categorize and discuss the existing research.
- Significance of the Study: Highlight why your literature review is important and how it contributes to the understanding of the chosen topic.
- Thesis Statement: Conclude the introduction with a concise thesis statement that outlines the main argument or perspective you will develop in the body of the literature review.
Body: The body of the literature review is where you provide a comprehensive analysis of existing literature, grouping studies based on themes, methodologies, or other relevant criteria.
- Organize by Theme or Concept: Group studies that share common themes, concepts, or methodologies. Discuss each theme or concept in detail, summarizing key findings and identifying gaps or areas of disagreement.
- Critical Analysis: Evaluate the strengths and weaknesses of each study. Discuss the methodologies used, the quality of evidence, and the overall contribution of each work to the understanding of the topic.
- Synthesis of Findings: Synthesize the information from different studies to highlight trends, patterns, or areas of consensus in the literature.
- Identification of Gaps: Discuss any gaps or limitations in the existing research and explain how your review contributes to filling these gaps.
- Transition between Sections: Provide smooth transitions between different themes or concepts to maintain the flow of your literature review.
Write and Cite as yo u go with Paperpal Research. Start now for free!
Conclusion: The conclusion of your literature review should summarize the main findings, highlight the contributions of the review, and suggest avenues for future research.
- Summary of Key Findings: Recap the main findings from the literature and restate how they contribute to your research question or objective.
- Contributions to the Field: Discuss the overall contribution of your literature review to the existing knowledge in the field.
- Implications and Applications: Explore the practical implications of the findings and suggest how they might impact future research or practice.
- Recommendations for Future Research: Identify areas that require further investigation and propose potential directions for future research in the field.
- Final Thoughts: Conclude with a final reflection on the importance of your literature review and its relevance to the broader academic community.

Conducting a literature review
Conducting a literature review is an essential step in research that involves reviewing and analyzing existing literature on a specific topic. It’s important to know how to do a literature review effectively, so here are the steps to follow: 1
Choose a Topic and Define the Research Question:
- Select a topic that is relevant to your field of study.
- Clearly define your research question or objective. Determine what specific aspect of the topic do you want to explore?
Decide on the Scope of Your Review:
- Determine the timeframe for your literature review. Are you focusing on recent developments, or do you want a historical overview?
- Consider the geographical scope. Is your review global, or are you focusing on a specific region?
- Define the inclusion and exclusion criteria. What types of sources will you include? Are there specific types of studies or publications you will exclude?
Select Databases for Searches:
- Identify relevant databases for your field. Examples include PubMed, IEEE Xplore, Scopus, Web of Science, and Google Scholar.
- Consider searching in library catalogs, institutional repositories, and specialized databases related to your topic.
Conduct Searches and Keep Track:
- Develop a systematic search strategy using keywords, Boolean operators (AND, OR, NOT), and other search techniques.
- Record and document your search strategy for transparency and replicability.
- Keep track of the articles, including publication details, abstracts, and links. Use citation management tools like EndNote, Zotero, or Mendeley to organize your references.
Review the Literature:
- Evaluate the relevance and quality of each source. Consider the methodology, sample size, and results of studies.
- Organize the literature by themes or key concepts. Identify patterns, trends, and gaps in the existing research.
- Summarize key findings and arguments from each source. Compare and contrast different perspectives.
- Identify areas where there is a consensus in the literature and where there are conflicting opinions.
- Provide critical analysis and synthesis of the literature. What are the strengths and weaknesses of existing research?
Organize and Write Your Literature Review:
- Literature review outline should be based on themes, chronological order, or methodological approaches.
- Write a clear and coherent narrative that synthesizes the information gathered.
- Use proper citations for each source and ensure consistency in your citation style (APA, MLA, Chicago, etc.).
- Conclude your literature review by summarizing key findings, identifying gaps, and suggesting areas for future research.
Whether you’re exploring a new research field or finding new angles to develop an existing topic, sifting through hundreds of papers can take more time than you have to spare. But what if you could find science-backed insights with verified citations in seconds? That’s the power of Paperpal’s new Research feature!
How to write a literature review faster with Paperpal?
Paperpal, an AI writing assistant, integrates powerful academic search capabilities within its writing platform. With the Research | Cite feature, you get 100% factual insights, with citations backed by 250M+ verified research articles, directly within your writing interface. It also allows you auto-cite references in 10,000+ styles and save relevant references in your Citation Library. By eliminating the need to switch tabs to find answers to all your research questions, Paperpal saves time and helps you stay focused on your writing.
Here’s how to use the Research feature:
- Ask a question: Get started with a new document on paperpal.com. Click on the “Research | Cite” feature and type your question in plain English. Paperpal will scour over 250 million research articles, including conference papers and preprints, to provide you with accurate insights and citations.
- Review and Save: Paperpal summarizes the information, while citing sources and listing relevant reads. You can quickly scan the results to identify relevant references and save these directly to your built-in citations library for later access.
- Cite with Confidence: Paperpal makes it easy to incorporate relevant citations and references in 10,000+ styles into your writing, ensuring your arguments are well-supported by credible sources. This translates to a polished, well-researched literature review.
The literature review sample and detailed advice on writing and conducting a review will help you produce a well-structured report. But remember that a good literature review is an ongoing process, and it may be necessary to revisit and update it as your research progresses. By combining effortless research with an easy citation process, Paperpal Research streamlines the literature review process and empowers you to write faster and with more confidence. Try Paperpal Research now and see for yourself.
A literature review is a critical and comprehensive analysis of existing literature (published and unpublished works) on a specific topic or research question and provides a synthesis of the current state of knowledge in a particular field. A well-conducted literature review is crucial for researchers to build upon existing knowledge, avoid duplication of efforts, and contribute to the advancement of their field. It also helps researchers situate their work within a broader context and facilitates the development of a sound theoretical and conceptual framework for their studies.
Literature review is a crucial component of research writing, providing a solid background for a research paper’s investigation. The aim is to keep professionals up to date by providing an understanding of ongoing developments within a specific field, including research methods, and experimental techniques used in that field, and present that knowledge in the form of a written report. Also, the depth and breadth of the literature review emphasizes the credibility of the scholar in his or her field.
Before writing a literature review, it’s essential to undertake several preparatory steps to ensure that your review is well-researched, organized, and focused. This includes choosing a topic of general interest to you and doing exploratory research on that topic, writing an annotated bibliography, and noting major points, especially those that relate to the position you have taken on the topic.
Literature reviews and academic research papers are essential components of scholarly work but serve different purposes within the academic realm. 3 A literature review aims to provide a foundation for understanding the current state of research on a particular topic, identify gaps or controversies, and lay the groundwork for future research. Therefore, it draws heavily from existing academic sources, including books, journal articles, and other scholarly publications. In contrast, an academic research paper aims to present new knowledge, contribute to the academic discourse, and advance the understanding of a specific research question. Therefore, it involves a mix of existing literature (in the introduction and literature review sections) and original data or findings obtained through research methods.
Literature reviews are essential components of academic and research papers, and various strategies can be employed to conduct them effectively. If you want to know how to write a literature review for a research paper, here are four common approaches that are often used by researchers. Chronological Review: This strategy involves organizing the literature based on the chronological order of publication. It helps to trace the development of a topic over time, showing how ideas, theories, and research have evolved. Thematic Review: Thematic reviews focus on identifying and analyzing themes or topics that cut across different studies. Instead of organizing the literature chronologically, it is grouped by key themes or concepts, allowing for a comprehensive exploration of various aspects of the topic. Methodological Review: This strategy involves organizing the literature based on the research methods employed in different studies. It helps to highlight the strengths and weaknesses of various methodologies and allows the reader to evaluate the reliability and validity of the research findings. Theoretical Review: A theoretical review examines the literature based on the theoretical frameworks used in different studies. This approach helps to identify the key theories that have been applied to the topic and assess their contributions to the understanding of the subject. It’s important to note that these strategies are not mutually exclusive, and a literature review may combine elements of more than one approach. The choice of strategy depends on the research question, the nature of the literature available, and the goals of the review. Additionally, other strategies, such as integrative reviews or systematic reviews, may be employed depending on the specific requirements of the research.
The literature review format can vary depending on the specific publication guidelines. However, there are some common elements and structures that are often followed. Here is a general guideline for the format of a literature review: Introduction: Provide an overview of the topic. Define the scope and purpose of the literature review. State the research question or objective. Body: Organize the literature by themes, concepts, or chronology. Critically analyze and evaluate each source. Discuss the strengths and weaknesses of the studies. Highlight any methodological limitations or biases. Identify patterns, connections, or contradictions in the existing research. Conclusion: Summarize the key points discussed in the literature review. Highlight the research gap. Address the research question or objective stated in the introduction. Highlight the contributions of the review and suggest directions for future research.
Both annotated bibliographies and literature reviews involve the examination of scholarly sources. While annotated bibliographies focus on individual sources with brief annotations, literature reviews provide a more in-depth, integrated, and comprehensive analysis of existing literature on a specific topic. The key differences are as follows:
| Annotated Bibliography | Literature Review | |
| Purpose | List of citations of books, articles, and other sources with a brief description (annotation) of each source. | Comprehensive and critical analysis of existing literature on a specific topic. |
| Focus | Summary and evaluation of each source, including its relevance, methodology, and key findings. | Provides an overview of the current state of knowledge on a particular subject and identifies gaps, trends, and patterns in existing literature. |
| Structure | Each citation is followed by a concise paragraph (annotation) that describes the source’s content, methodology, and its contribution to the topic. | The literature review is organized thematically or chronologically and involves a synthesis of the findings from different sources to build a narrative or argument. |
| Length | Typically 100-200 words | Length of literature review ranges from a few pages to several chapters |
| Independence | Each source is treated separately, with less emphasis on synthesizing the information across sources. | The writer synthesizes information from multiple sources to present a cohesive overview of the topic. |
References
- Denney, A. S., & Tewksbury, R. (2013). How to write a literature review. Journal of criminal justice education , 24 (2), 218-234.
- Pan, M. L. (2016). Preparing literature reviews: Qualitative and quantitative approaches . Taylor & Francis.
- Cantero, C. (2019). How to write a literature review. San José State University Writing Center .
Paperpal is a comprehensive AI writing toolkit that helps students and researchers achieve 2x the writing in half the time. It leverages 22+ years of STM experience and insights from millions of research articles to provide in-depth academic writing, language editing, and submission readiness support to help you write better, faster.
Get accurate academic translations, rewriting support, grammar checks, vocabulary suggestions, and generative AI assistance that delivers human precision at machine speed. Try for free or upgrade to Paperpal Prime starting at US$19 a month to access premium features, including consistency, plagiarism, and 30+ submission readiness checks to help you succeed.
Experience the future of academic writing – Sign up to Paperpal and start writing for free!
Related Reads:
- Empirical Research: A Comprehensive Guide for Academics
- How to Write a Scientific Paper in 10 Steps
- How Long Should a Chapter Be?
- How to Use Paperpal to Generate Emails & Cover Letters?
6 Tips for Post-Doc Researchers to Take Their Career to the Next Level
Self-plagiarism in research: what it is and how to avoid it, you may also like, how to make a graphical abstract, academic integrity vs academic dishonesty: types & examples, dissertation printing and binding | types & comparison , what is a dissertation preface definition and examples , the ai revolution: authors’ role in upholding academic..., the future of academia: how ai tools are..., how to write a research proposal: (with examples..., how to write your research paper in apa..., how to choose a dissertation topic, how to write a phd research proposal.

University Libraries
Literature review.
- What is a Literature Review?
- What is Its Purpose?
- 1. Select a Topic
- 2. Set the Topic in Context
- 3. Types of Information Sources
- 4. Use Information Sources
- 5. Get the Information
- 6. Organize / Manage the Information
- 7. Position the Literature Review
- 8. Write the Literature Review

A literature review is a comprehensive summary of previous research on a topic. The literature review surveys scholarly articles, books, and other sources relevant to a particular area of research. The review should enumerate, describe, summarize, objectively evaluate and clarify this previous research. It should give a theoretical base for the research and help you (the author) determine the nature of your research. The literature review acknowledges the work of previous researchers, and in so doing, assures the reader that your work has been well conceived. It is assumed that by mentioning a previous work in the field of study, that the author has read, evaluated, and assimiliated that work into the work at hand.
A literature review creates a "landscape" for the reader, giving her or him a full understanding of the developments in the field. This landscape informs the reader that the author has indeed assimilated all (or the vast majority of) previous, significant works in the field into her or his research.
"In writing the literature review, the purpose is to convey to the reader what knowledge and ideas have been established on a topic, and what their strengths and weaknesses are. The literature review must be defined by a guiding concept (eg. your research objective, the problem or issue you are discussing, or your argumentative thesis). It is not just a descriptive list of the material available, or a set of summaries.( http://www.writing.utoronto.ca/advice/specific-types-of-writing/literature-review )
Recommended Reading
- Next: What is Its Purpose? >>
- Last Updated: Oct 2, 2023 12:34 PM
- USC Libraries
- Research Guides
Organizing Your Social Sciences Research Paper
- 5. The Literature Review
- Purpose of Guide
- Design Flaws to Avoid
- Independent and Dependent Variables
- Glossary of Research Terms
- Reading Research Effectively
- Narrowing a Topic Idea
- Broadening a Topic Idea
- Extending the Timeliness of a Topic Idea
- Academic Writing Style
- Applying Critical Thinking
- Choosing a Title
- Making an Outline
- Paragraph Development
- Research Process Video Series
- Executive Summary
- The C.A.R.S. Model
- Background Information
- The Research Problem/Question
- Theoretical Framework
- Citation Tracking
- Content Alert Services
- Evaluating Sources
- Primary Sources
- Secondary Sources
- Tiertiary Sources
- Scholarly vs. Popular Publications
- Qualitative Methods
- Quantitative Methods
- Insiderness
- Using Non-Textual Elements
- Limitations of the Study
- Common Grammar Mistakes
- Writing Concisely
- Avoiding Plagiarism
- Footnotes or Endnotes?
- Further Readings
- Generative AI and Writing
- USC Libraries Tutorials and Other Guides
- Bibliography
A literature review surveys prior research published in books, scholarly articles, and any other sources relevant to a particular issue, area of research, or theory, and by so doing, provides a description, summary, and critical evaluation of these works in relation to the research problem being investigated. Literature reviews are designed to provide an overview of sources you have used in researching a particular topic and to demonstrate to your readers how your research fits within existing scholarship about the topic.
Fink, Arlene. Conducting Research Literature Reviews: From the Internet to Paper . Fourth edition. Thousand Oaks, CA: SAGE, 2014.
Importance of a Good Literature Review
A literature review may consist of simply a summary of key sources, but in the social sciences, a literature review usually has an organizational pattern and combines both summary and synthesis, often within specific conceptual categories . A summary is a recap of the important information of the source, but a synthesis is a re-organization, or a reshuffling, of that information in a way that informs how you are planning to investigate a research problem. The analytical features of a literature review might:
- Give a new interpretation of old material or combine new with old interpretations,
- Trace the intellectual progression of the field, including major debates,
- Depending on the situation, evaluate the sources and advise the reader on the most pertinent or relevant research, or
- Usually in the conclusion of a literature review, identify where gaps exist in how a problem has been researched to date.
Given this, the purpose of a literature review is to:
- Place each work in the context of its contribution to understanding the research problem being studied.
- Describe the relationship of each work to the others under consideration.
- Identify new ways to interpret prior research.
- Reveal any gaps that exist in the literature.
- Resolve conflicts amongst seemingly contradictory previous studies.
- Identify areas of prior scholarship to prevent duplication of effort.
- Point the way in fulfilling a need for additional research.
- Locate your own research within the context of existing literature [very important].
Fink, Arlene. Conducting Research Literature Reviews: From the Internet to Paper. 2nd ed. Thousand Oaks, CA: Sage, 2005; Hart, Chris. Doing a Literature Review: Releasing the Social Science Research Imagination . Thousand Oaks, CA: Sage Publications, 1998; Jesson, Jill. Doing Your Literature Review: Traditional and Systematic Techniques . Los Angeles, CA: SAGE, 2011; Knopf, Jeffrey W. "Doing a Literature Review." PS: Political Science and Politics 39 (January 2006): 127-132; Ridley, Diana. The Literature Review: A Step-by-Step Guide for Students . 2nd ed. Los Angeles, CA: SAGE, 2012.
Types of Literature Reviews
It is important to think of knowledge in a given field as consisting of three layers. First, there are the primary studies that researchers conduct and publish. Second are the reviews of those studies that summarize and offer new interpretations built from and often extending beyond the primary studies. Third, there are the perceptions, conclusions, opinion, and interpretations that are shared informally among scholars that become part of the body of epistemological traditions within the field.
In composing a literature review, it is important to note that it is often this third layer of knowledge that is cited as "true" even though it often has only a loose relationship to the primary studies and secondary literature reviews. Given this, while literature reviews are designed to provide an overview and synthesis of pertinent sources you have explored, there are a number of approaches you could adopt depending upon the type of analysis underpinning your study.
Argumentative Review This form examines literature selectively in order to support or refute an argument, deeply embedded assumption, or philosophical problem already established in the literature. The purpose is to develop a body of literature that establishes a contrarian viewpoint. Given the value-laden nature of some social science research [e.g., educational reform; immigration control], argumentative approaches to analyzing the literature can be a legitimate and important form of discourse. However, note that they can also introduce problems of bias when they are used to make summary claims of the sort found in systematic reviews [see below].
Integrative Review Considered a form of research that reviews, critiques, and synthesizes representative literature on a topic in an integrated way such that new frameworks and perspectives on the topic are generated. The body of literature includes all studies that address related or identical hypotheses or research problems. A well-done integrative review meets the same standards as primary research in regard to clarity, rigor, and replication. This is the most common form of review in the social sciences.
Historical Review Few things rest in isolation from historical precedent. Historical literature reviews focus on examining research throughout a period of time, often starting with the first time an issue, concept, theory, phenomena emerged in the literature, then tracing its evolution within the scholarship of a discipline. The purpose is to place research in a historical context to show familiarity with state-of-the-art developments and to identify the likely directions for future research.
Methodological Review A review does not always focus on what someone said [findings], but how they came about saying what they say [method of analysis]. Reviewing methods of analysis provides a framework of understanding at different levels [i.e. those of theory, substantive fields, research approaches, and data collection and analysis techniques], how researchers draw upon a wide variety of knowledge ranging from the conceptual level to practical documents for use in fieldwork in the areas of ontological and epistemological consideration, quantitative and qualitative integration, sampling, interviewing, data collection, and data analysis. This approach helps highlight ethical issues which you should be aware of and consider as you go through your own study.
Systematic Review This form consists of an overview of existing evidence pertinent to a clearly formulated research question, which uses pre-specified and standardized methods to identify and critically appraise relevant research, and to collect, report, and analyze data from the studies that are included in the review. The goal is to deliberately document, critically evaluate, and summarize scientifically all of the research about a clearly defined research problem . Typically it focuses on a very specific empirical question, often posed in a cause-and-effect form, such as "To what extent does A contribute to B?" This type of literature review is primarily applied to examining prior research studies in clinical medicine and allied health fields, but it is increasingly being used in the social sciences.
Theoretical Review The purpose of this form is to examine the corpus of theory that has accumulated in regard to an issue, concept, theory, phenomena. The theoretical literature review helps to establish what theories already exist, the relationships between them, to what degree the existing theories have been investigated, and to develop new hypotheses to be tested. Often this form is used to help establish a lack of appropriate theories or reveal that current theories are inadequate for explaining new or emerging research problems. The unit of analysis can focus on a theoretical concept or a whole theory or framework.
NOTE: Most often the literature review will incorporate some combination of types. For example, a review that examines literature supporting or refuting an argument, assumption, or philosophical problem related to the research problem will also need to include writing supported by sources that establish the history of these arguments in the literature.
Baumeister, Roy F. and Mark R. Leary. "Writing Narrative Literature Reviews." Review of General Psychology 1 (September 1997): 311-320; Mark R. Fink, Arlene. Conducting Research Literature Reviews: From the Internet to Paper . 2nd ed. Thousand Oaks, CA: Sage, 2005; Hart, Chris. Doing a Literature Review: Releasing the Social Science Research Imagination . Thousand Oaks, CA: Sage Publications, 1998; Kennedy, Mary M. "Defining a Literature." Educational Researcher 36 (April 2007): 139-147; Petticrew, Mark and Helen Roberts. Systematic Reviews in the Social Sciences: A Practical Guide . Malden, MA: Blackwell Publishers, 2006; Torracro, Richard. "Writing Integrative Literature Reviews: Guidelines and Examples." Human Resource Development Review 4 (September 2005): 356-367; Rocco, Tonette S. and Maria S. Plakhotnik. "Literature Reviews, Conceptual Frameworks, and Theoretical Frameworks: Terms, Functions, and Distinctions." Human Ressource Development Review 8 (March 2008): 120-130; Sutton, Anthea. Systematic Approaches to a Successful Literature Review . Los Angeles, CA: Sage Publications, 2016.
Structure and Writing Style
I. Thinking About Your Literature Review
The structure of a literature review should include the following in support of understanding the research problem :
- An overview of the subject, issue, or theory under consideration, along with the objectives of the literature review,
- Division of works under review into themes or categories [e.g. works that support a particular position, those against, and those offering alternative approaches entirely],
- An explanation of how each work is similar to and how it varies from the others,
- Conclusions as to which pieces are best considered in their argument, are most convincing of their opinions, and make the greatest contribution to the understanding and development of their area of research.
The critical evaluation of each work should consider :
- Provenance -- what are the author's credentials? Are the author's arguments supported by evidence [e.g. primary historical material, case studies, narratives, statistics, recent scientific findings]?
- Methodology -- were the techniques used to identify, gather, and analyze the data appropriate to addressing the research problem? Was the sample size appropriate? Were the results effectively interpreted and reported?
- Objectivity -- is the author's perspective even-handed or prejudicial? Is contrary data considered or is certain pertinent information ignored to prove the author's point?
- Persuasiveness -- which of the author's theses are most convincing or least convincing?
- Validity -- are the author's arguments and conclusions convincing? Does the work ultimately contribute in any significant way to an understanding of the subject?
II. Development of the Literature Review
Four Basic Stages of Writing 1. Problem formulation -- which topic or field is being examined and what are its component issues? 2. Literature search -- finding materials relevant to the subject being explored. 3. Data evaluation -- determining which literature makes a significant contribution to the understanding of the topic. 4. Analysis and interpretation -- discussing the findings and conclusions of pertinent literature.
Consider the following issues before writing the literature review: Clarify If your assignment is not specific about what form your literature review should take, seek clarification from your professor by asking these questions: 1. Roughly how many sources would be appropriate to include? 2. What types of sources should I review (books, journal articles, websites; scholarly versus popular sources)? 3. Should I summarize, synthesize, or critique sources by discussing a common theme or issue? 4. Should I evaluate the sources in any way beyond evaluating how they relate to understanding the research problem? 5. Should I provide subheadings and other background information, such as definitions and/or a history? Find Models Use the exercise of reviewing the literature to examine how authors in your discipline or area of interest have composed their literature review sections. Read them to get a sense of the types of themes you might want to look for in your own research or to identify ways to organize your final review. The bibliography or reference section of sources you've already read, such as required readings in the course syllabus, are also excellent entry points into your own research. Narrow the Topic The narrower your topic, the easier it will be to limit the number of sources you need to read in order to obtain a good survey of relevant resources. Your professor will probably not expect you to read everything that's available about the topic, but you'll make the act of reviewing easier if you first limit scope of the research problem. A good strategy is to begin by searching the USC Libraries Catalog for recent books about the topic and review the table of contents for chapters that focuses on specific issues. You can also review the indexes of books to find references to specific issues that can serve as the focus of your research. For example, a book surveying the history of the Israeli-Palestinian conflict may include a chapter on the role Egypt has played in mediating the conflict, or look in the index for the pages where Egypt is mentioned in the text. Consider Whether Your Sources are Current Some disciplines require that you use information that is as current as possible. This is particularly true in disciplines in medicine and the sciences where research conducted becomes obsolete very quickly as new discoveries are made. However, when writing a review in the social sciences, a survey of the history of the literature may be required. In other words, a complete understanding the research problem requires you to deliberately examine how knowledge and perspectives have changed over time. Sort through other current bibliographies or literature reviews in the field to get a sense of what your discipline expects. You can also use this method to explore what is considered by scholars to be a "hot topic" and what is not.
III. Ways to Organize Your Literature Review
Chronology of Events If your review follows the chronological method, you could write about the materials according to when they were published. This approach should only be followed if a clear path of research building on previous research can be identified and that these trends follow a clear chronological order of development. For example, a literature review that focuses on continuing research about the emergence of German economic power after the fall of the Soviet Union. By Publication Order your sources by publication chronology, then, only if the order demonstrates a more important trend. For instance, you could order a review of literature on environmental studies of brown fields if the progression revealed, for example, a change in the soil collection practices of the researchers who wrote and/or conducted the studies. Thematic [“conceptual categories”] A thematic literature review is the most common approach to summarizing prior research in the social and behavioral sciences. Thematic reviews are organized around a topic or issue, rather than the progression of time, although the progression of time may still be incorporated into a thematic review. For example, a review of the Internet’s impact on American presidential politics could focus on the development of online political satire. While the study focuses on one topic, the Internet’s impact on American presidential politics, it would still be organized chronologically reflecting technological developments in media. The difference in this example between a "chronological" and a "thematic" approach is what is emphasized the most: themes related to the role of the Internet in presidential politics. Note that more authentic thematic reviews tend to break away from chronological order. A review organized in this manner would shift between time periods within each section according to the point being made. Methodological A methodological approach focuses on the methods utilized by the researcher. For the Internet in American presidential politics project, one methodological approach would be to look at cultural differences between the portrayal of American presidents on American, British, and French websites. Or the review might focus on the fundraising impact of the Internet on a particular political party. A methodological scope will influence either the types of documents in the review or the way in which these documents are discussed.
Other Sections of Your Literature Review Once you've decided on the organizational method for your literature review, the sections you need to include in the paper should be easy to figure out because they arise from your organizational strategy. In other words, a chronological review would have subsections for each vital time period; a thematic review would have subtopics based upon factors that relate to the theme or issue. However, sometimes you may need to add additional sections that are necessary for your study, but do not fit in the organizational strategy of the body. What other sections you include in the body is up to you. However, only include what is necessary for the reader to locate your study within the larger scholarship about the research problem.
Here are examples of other sections, usually in the form of a single paragraph, you may need to include depending on the type of review you write:
- Current Situation : Information necessary to understand the current topic or focus of the literature review.
- Sources Used : Describes the methods and resources [e.g., databases] you used to identify the literature you reviewed.
- History : The chronological progression of the field, the research literature, or an idea that is necessary to understand the literature review, if the body of the literature review is not already a chronology.
- Selection Methods : Criteria you used to select (and perhaps exclude) sources in your literature review. For instance, you might explain that your review includes only peer-reviewed [i.e., scholarly] sources.
- Standards : Description of the way in which you present your information.
- Questions for Further Research : What questions about the field has the review sparked? How will you further your research as a result of the review?
IV. Writing Your Literature Review
Once you've settled on how to organize your literature review, you're ready to write each section. When writing your review, keep in mind these issues.
Use Evidence A literature review section is, in this sense, just like any other academic research paper. Your interpretation of the available sources must be backed up with evidence [citations] that demonstrates that what you are saying is valid. Be Selective Select only the most important points in each source to highlight in the review. The type of information you choose to mention should relate directly to the research problem, whether it is thematic, methodological, or chronological. Related items that provide additional information, but that are not key to understanding the research problem, can be included in a list of further readings . Use Quotes Sparingly Some short quotes are appropriate if you want to emphasize a point, or if what an author stated cannot be easily paraphrased. Sometimes you may need to quote certain terminology that was coined by the author, is not common knowledge, or taken directly from the study. Do not use extensive quotes as a substitute for using your own words in reviewing the literature. Summarize and Synthesize Remember to summarize and synthesize your sources within each thematic paragraph as well as throughout the review. Recapitulate important features of a research study, but then synthesize it by rephrasing the study's significance and relating it to your own work and the work of others. Keep Your Own Voice While the literature review presents others' ideas, your voice [the writer's] should remain front and center. For example, weave references to other sources into what you are writing but maintain your own voice by starting and ending the paragraph with your own ideas and wording. Use Caution When Paraphrasing When paraphrasing a source that is not your own, be sure to represent the author's information or opinions accurately and in your own words. Even when paraphrasing an author’s work, you still must provide a citation to that work.
V. Common Mistakes to Avoid
These are the most common mistakes made in reviewing social science research literature.
- Sources in your literature review do not clearly relate to the research problem;
- You do not take sufficient time to define and identify the most relevant sources to use in the literature review related to the research problem;
- Relies exclusively on secondary analytical sources rather than including relevant primary research studies or data;
- Uncritically accepts another researcher's findings and interpretations as valid, rather than examining critically all aspects of the research design and analysis;
- Does not describe the search procedures that were used in identifying the literature to review;
- Reports isolated statistical results rather than synthesizing them in chi-squared or meta-analytic methods; and,
- Only includes research that validates assumptions and does not consider contrary findings and alternative interpretations found in the literature.
Cook, Kathleen E. and Elise Murowchick. “Do Literature Review Skills Transfer from One Course to Another?” Psychology Learning and Teaching 13 (March 2014): 3-11; Fink, Arlene. Conducting Research Literature Reviews: From the Internet to Paper . 2nd ed. Thousand Oaks, CA: Sage, 2005; Hart, Chris. Doing a Literature Review: Releasing the Social Science Research Imagination . Thousand Oaks, CA: Sage Publications, 1998; Jesson, Jill. Doing Your Literature Review: Traditional and Systematic Techniques . London: SAGE, 2011; Literature Review Handout. Online Writing Center. Liberty University; Literature Reviews. The Writing Center. University of North Carolina; Onwuegbuzie, Anthony J. and Rebecca Frels. Seven Steps to a Comprehensive Literature Review: A Multimodal and Cultural Approach . Los Angeles, CA: SAGE, 2016; Ridley, Diana. The Literature Review: A Step-by-Step Guide for Students . 2nd ed. Los Angeles, CA: SAGE, 2012; Randolph, Justus J. “A Guide to Writing the Dissertation Literature Review." Practical Assessment, Research, and Evaluation. vol. 14, June 2009; Sutton, Anthea. Systematic Approaches to a Successful Literature Review . Los Angeles, CA: Sage Publications, 2016; Taylor, Dena. The Literature Review: A Few Tips On Conducting It. University College Writing Centre. University of Toronto; Writing a Literature Review. Academic Skills Centre. University of Canberra.
Writing Tip
Break Out of Your Disciplinary Box!
Thinking interdisciplinarily about a research problem can be a rewarding exercise in applying new ideas, theories, or concepts to an old problem. For example, what might cultural anthropologists say about the continuing conflict in the Middle East? In what ways might geographers view the need for better distribution of social service agencies in large cities than how social workers might study the issue? You don’t want to substitute a thorough review of core research literature in your discipline for studies conducted in other fields of study. However, particularly in the social sciences, thinking about research problems from multiple vectors is a key strategy for finding new solutions to a problem or gaining a new perspective. Consult with a librarian about identifying research databases in other disciplines; almost every field of study has at least one comprehensive database devoted to indexing its research literature.
Frodeman, Robert. The Oxford Handbook of Interdisciplinarity . New York: Oxford University Press, 2010.
Another Writing Tip
Don't Just Review for Content!
While conducting a review of the literature, maximize the time you devote to writing this part of your paper by thinking broadly about what you should be looking for and evaluating. Review not just what scholars are saying, but how are they saying it. Some questions to ask:
- How are they organizing their ideas?
- What methods have they used to study the problem?
- What theories have been used to explain, predict, or understand their research problem?
- What sources have they cited to support their conclusions?
- How have they used non-textual elements [e.g., charts, graphs, figures, etc.] to illustrate key points?
When you begin to write your literature review section, you'll be glad you dug deeper into how the research was designed and constructed because it establishes a means for developing more substantial analysis and interpretation of the research problem.
Hart, Chris. Doing a Literature Review: Releasing the Social Science Research Imagination . Thousand Oaks, CA: Sage Publications, 1 998.
Yet Another Writing Tip
When Do I Know I Can Stop Looking and Move On?
Here are several strategies you can utilize to assess whether you've thoroughly reviewed the literature:
- Look for repeating patterns in the research findings . If the same thing is being said, just by different people, then this likely demonstrates that the research problem has hit a conceptual dead end. At this point consider: Does your study extend current research? Does it forge a new path? Or, does is merely add more of the same thing being said?
- Look at sources the authors cite to in their work . If you begin to see the same researchers cited again and again, then this is often an indication that no new ideas have been generated to address the research problem.
- Search Google Scholar to identify who has subsequently cited leading scholars already identified in your literature review [see next sub-tab]. This is called citation tracking and there are a number of sources that can help you identify who has cited whom, particularly scholars from outside of your discipline. Here again, if the same authors are being cited again and again, this may indicate no new literature has been written on the topic.
Onwuegbuzie, Anthony J. and Rebecca Frels. Seven Steps to a Comprehensive Literature Review: A Multimodal and Cultural Approach . Los Angeles, CA: Sage, 2016; Sutton, Anthea. Systematic Approaches to a Successful Literature Review . Los Angeles, CA: Sage Publications, 2016.
- << Previous: Theoretical Framework
- Next: Citation Tracking >>
- Last Updated: Sep 17, 2024 10:59 AM
- URL: https://libguides.usc.edu/writingguide
Frequently asked questions
What is the purpose of a literature review.
There are several reasons to conduct a literature review at the beginning of a research project:
- To familiarise yourself with the current state of knowledge on your topic
- To ensure that you’re not just repeating what others have already done
- To identify gaps in knowledge and unresolved problems that your research can address
- To develop your theoretical framework and methodology
- To provide an overview of the key findings and debates on the topic
Writing the literature review shows your reader how your work relates to existing research and what new insights it will contribute.
Frequently asked questions: Knowledge Base
Methodology refers to the overarching strategy and rationale of your research. Developing your methodology involves studying the research methods used in your field and the theories or principles that underpin them, in order to choose the approach that best matches your objectives.
Methods are the specific tools and procedures you use to collect and analyse data (e.g. interviews, experiments , surveys , statistical tests ).
In a dissertation or scientific paper, the methodology chapter or methods section comes after the introduction and before the results , discussion and conclusion .
Depending on the length and type of document, you might also include a literature review or theoretical framework before the methodology.
Quantitative research deals with numbers and statistics, while qualitative research deals with words and meanings.
Quantitative methods allow you to test a hypothesis by systematically collecting and analysing data, while qualitative methods allow you to explore ideas and experiences in depth.
Reliability and validity are both about how well a method measures something:
- Reliability refers to the consistency of a measure (whether the results can be reproduced under the same conditions).
- Validity refers to the accuracy of a measure (whether the results really do represent what they are supposed to measure).
If you are doing experimental research , you also have to consider the internal and external validity of your experiment.
A sample is a subset of individuals from a larger population. Sampling means selecting the group that you will actually collect data from in your research.
For example, if you are researching the opinions of students in your university, you could survey a sample of 100 students.
Statistical sampling allows you to test a hypothesis about the characteristics of a population. There are various sampling methods you can use to ensure that your sample is representative of the population as a whole.
A literature review is a survey of scholarly sources (such as books, journal articles, and theses) related to a specific topic or research question .
It is often written as part of a dissertation , thesis, research paper , or proposal .
The literature review usually comes near the beginning of your dissertation . After the introduction , it grounds your research in a scholarly field and leads directly to your theoretical framework or methodology .
Harvard referencing uses an author–date system. Sources are cited by the author’s last name and the publication year in brackets. Each Harvard in-text citation corresponds to an entry in the alphabetised reference list at the end of the paper.
Vancouver referencing uses a numerical system. Sources are cited by a number in parentheses or superscript. Each number corresponds to a full reference at the end of the paper.
| Harvard style | Vancouver style | |
|---|---|---|
| In-text citation | Each referencing style has different rules (Pears and Shields, 2019). | Each referencing style has different rules (1). |
| Reference list | Pears, R. and Shields, G. (2019). . 11th edn. London: MacMillan. | 1. Pears R, Shields G. Cite them right: The essential referencing guide. 11th ed. London: MacMillan; 2019. |
A Harvard in-text citation should appear in brackets every time you quote, paraphrase, or refer to information from a source.
The citation can appear immediately after the quotation or paraphrase, or at the end of the sentence. If you’re quoting, place the citation outside of the quotation marks but before any other punctuation like a comma or full stop.
In Harvard referencing, up to three author names are included in an in-text citation or reference list entry. When there are four or more authors, include only the first, followed by ‘ et al. ’
| In-text citation | Reference list | |
|---|---|---|
| 1 author | (Smith, 2014) | Smith, T. (2014) … |
| 2 authors | (Smith and Jones, 2014) | Smith, T. and Jones, F. (2014) … |
| 3 authors | (Smith, Jones and Davies, 2014) | Smith, T., Jones, F. and Davies, S. (2014) … |
| 4+ authors | (Smith , 2014) | Smith, T. (2014) … |
A bibliography should always contain every source you cited in your text. Sometimes a bibliography also contains other sources that you used in your research, but did not cite in the text.
MHRA doesn’t specify a rule about this, so check with your supervisor to find out exactly what should be included in your bibliography.
Footnote numbers should appear in superscript (e.g. 11 ). You can use the ‘Insert footnote’ button in Word to do this automatically; it’s in the ‘References’ tab at the top.
Footnotes always appear after the quote or paraphrase they relate to. MHRA generally recommends placing footnote numbers at the end of the sentence, immediately after any closing punctuation, like this. 12
In situations where this might be awkward or misleading, such as a long sentence containing multiple quotations, footnotes can also be placed at the end of a clause mid-sentence, like this; 13 note that they still come after any punctuation.
When a source has two or three authors, name all of them in your MHRA references . When there are four or more, use only the first name, followed by ‘and others’:
| Number of authors | Footnote example | Bibliography example |
|---|---|---|
| 1 author | David Smith | Smith, David |
| 2 authors | David Smith and Hugh Jones | Smith, David, and Hugh Jones |
| 3 authors | David Smith, Hugh Jones and Emily Wright | Smith, David, Hugh Jones and Emily Wright |
| 4+ authors | David Smith and others | Smith, David, and others |
Note that in the bibliography, only the author listed first has their name inverted. The names of additional authors and those of translators or editors are written normally.
A citation should appear wherever you use information or ideas from a source, whether by quoting or paraphrasing its content.
In Vancouver style , you have some flexibility about where the citation number appears in the sentence – usually directly after mentioning the author’s name is best, but simply placing it at the end of the sentence is an acceptable alternative, as long as it’s clear what it relates to.
In Vancouver style , when you refer to a source with multiple authors in your text, you should only name the first author followed by ‘et al.’. This applies even when there are only two authors.
In your reference list, include up to six authors. For sources with seven or more authors, list the first six followed by ‘et al.’.
The words ‘ dissertation ’ and ‘thesis’ both refer to a large written research project undertaken to complete a degree, but they are used differently depending on the country:
- In the UK, you write a dissertation at the end of a bachelor’s or master’s degree, and you write a thesis to complete a PhD.
- In the US, it’s the other way around: you may write a thesis at the end of a bachelor’s or master’s degree, and you write a dissertation to complete a PhD.
The main difference is in terms of scale – a dissertation is usually much longer than the other essays you complete during your degree.
Another key difference is that you are given much more independence when working on a dissertation. You choose your own dissertation topic , and you have to conduct the research and write the dissertation yourself (with some assistance from your supervisor).
Dissertation word counts vary widely across different fields, institutions, and levels of education:
- An undergraduate dissertation is typically 8,000–15,000 words
- A master’s dissertation is typically 12,000–50,000 words
- A PhD thesis is typically book-length: 70,000–100,000 words
However, none of these are strict guidelines – your word count may be lower or higher than the numbers stated here. Always check the guidelines provided by your university to determine how long your own dissertation should be.
At the bachelor’s and master’s levels, the dissertation is usually the main focus of your final year. You might work on it (alongside other classes) for the entirety of the final year, or for the last six months. This includes formulating an idea, doing the research, and writing up.
A PhD thesis takes a longer time, as the thesis is the main focus of the degree. A PhD thesis might be being formulated and worked on for the whole four years of the degree program. The writing process alone can take around 18 months.
References should be included in your text whenever you use words, ideas, or information from a source. A source can be anything from a book or journal article to a website or YouTube video.
If you don’t acknowledge your sources, you can get in trouble for plagiarism .
Your university should tell you which referencing style to follow. If you’re unsure, check with a supervisor. Commonly used styles include:
- Harvard referencing , the most commonly used style in UK universities.
- MHRA , used in humanities subjects.
- APA , used in the social sciences.
- Vancouver , used in biomedicine.
- OSCOLA , used in law.
Your university may have its own referencing style guide.
If you are allowed to choose which style to follow, we recommend Harvard referencing, as it is a straightforward and widely used style.
To avoid plagiarism , always include a reference when you use words, ideas or information from a source. This shows that you are not trying to pass the work of others off as your own.
You must also properly quote or paraphrase the source. If you’re not sure whether you’ve done this correctly, you can use the Scribbr Plagiarism Checker to find and correct any mistakes.
In Harvard style , when you quote directly from a source that includes page numbers, your in-text citation must include a page number. For example: (Smith, 2014, p. 33).
You can also include page numbers to point the reader towards a passage that you paraphrased . If you refer to the general ideas or findings of the source as a whole, you don’t need to include a page number.
When you want to use a quote but can’t access the original source, you can cite it indirectly. In the in-text citation , first mention the source you want to refer to, and then the source in which you found it. For example:
It’s advisable to avoid indirect citations wherever possible, because they suggest you don’t have full knowledge of the sources you’re citing. Only use an indirect citation if you can’t reasonably gain access to the original source.
In Harvard style referencing , to distinguish between two sources by the same author that were published in the same year, you add a different letter after the year for each source:
- (Smith, 2019a)
- (Smith, 2019b)
Add ‘a’ to the first one you cite, ‘b’ to the second, and so on. Do the same in your bibliography or reference list .
To create a hanging indent for your bibliography or reference list :
- Highlight all the entries
- Click on the arrow in the bottom-right corner of the ‘Paragraph’ tab in the top menu.
- In the pop-up window, under ‘Special’ in the ‘Indentation’ section, use the drop-down menu to select ‘Hanging’.
- Then close the window with ‘OK’.
Though the terms are sometimes used interchangeably, there is a difference in meaning:
- A reference list only includes sources cited in the text – every entry corresponds to an in-text citation .
- A bibliography also includes other sources which were consulted during the research but not cited.
It’s important to assess the reliability of information found online. Look for sources from established publications and institutions with expertise (e.g. peer-reviewed journals and government agencies).
The CRAAP test (currency, relevance, authority, accuracy, purpose) can aid you in assessing sources, as can our list of credible sources . You should generally avoid citing websites like Wikipedia that can be edited by anyone – instead, look for the original source of the information in the “References” section.
You can generally omit page numbers in your in-text citations of online sources which don’t have them. But when you quote or paraphrase a specific passage from a particularly long online source, it’s useful to find an alternate location marker.
For text-based sources, you can use paragraph numbers (e.g. ‘para. 4’) or headings (e.g. ‘under “Methodology”’). With video or audio sources, use a timestamp (e.g. ‘10:15’).
In the acknowledgements of your thesis or dissertation, you should first thank those who helped you academically or professionally, such as your supervisor, funders, and other academics.
Then you can include personal thanks to friends, family members, or anyone else who supported you during the process.
Yes, it’s important to thank your supervisor(s) in the acknowledgements section of your thesis or dissertation .
Even if you feel your supervisor did not contribute greatly to the final product, you still should acknowledge them, if only for a very brief thank you. If you do not include your supervisor, it may be seen as a snub.
The acknowledgements are generally included at the very beginning of your thesis or dissertation, directly after the title page and before the abstract .
In a thesis or dissertation, the acknowledgements should usually be no longer than one page. There is no minimum length.
You may acknowledge God in your thesis or dissertation acknowledgements , but be sure to follow academic convention by also thanking the relevant members of academia, as well as family, colleagues, and friends who helped you.
All level 1 and 2 headings should be included in your table of contents . That means the titles of your chapters and the main sections within them.
The contents should also include all appendices and the lists of tables and figures, if applicable, as well as your reference list .
Do not include the acknowledgements or abstract in the table of contents.
To automatically insert a table of contents in Microsoft Word, follow these steps:
- Apply heading styles throughout the document.
- In the references section in the ribbon, locate the Table of Contents group.
- Click the arrow next to the Table of Contents icon and select Custom Table of Contents.
- Select which levels of headings you would like to include in the table of contents.
Make sure to update your table of contents if you move text or change headings. To update, simply right click and select Update Field.
The table of contents in a thesis or dissertation always goes between your abstract and your introduction.
An abbreviation is a shortened version of an existing word, such as Dr for Doctor. In contrast, an acronym uses the first letter of each word to create a wholly new word, such as UNESCO (an acronym for the United Nations Educational, Scientific and Cultural Organization).
Your dissertation sometimes contains a list of abbreviations .
As a rule of thumb, write the explanation in full the first time you use an acronym or abbreviation. You can then proceed with the shortened version. However, if the abbreviation is very common (like UK or PC), then you can just use the abbreviated version straight away.
Be sure to add each abbreviation in your list of abbreviations !
If you only used a few abbreviations in your thesis or dissertation, you don’t necessarily need to include a list of abbreviations .
If your abbreviations are numerous, or if you think they won’t be known to your audience, it’s never a bad idea to add one. They can also improve readability, minimising confusion about abbreviations unfamiliar to your reader.
A list of abbreviations is a list of all the abbreviations you used in your thesis or dissertation. It should appear at the beginning of your document, immediately after your table of contents . It should always be in alphabetical order.
Fishbone diagrams have a few different names that are used interchangeably, including herringbone diagram, cause-and-effect diagram, and Ishikawa diagram.
These are all ways to refer to the same thing– a problem-solving approach that uses a fish-shaped diagram to model possible root causes of problems and troubleshoot solutions.
Fishbone diagrams (also called herringbone diagrams, cause-and-effect diagrams, and Ishikawa diagrams) are most popular in fields of quality management. They are also commonly used in nursing and healthcare, or as a brainstorming technique for students.
Some synonyms and near synonyms of among include:
- In the company of
- In the middle of
- Surrounded by
Some synonyms and near synonyms of between include:
- In the space separating
- In the time separating
In spite of is a preposition used to mean ‘ regardless of ‘, ‘notwithstanding’, or ‘even though’.
It’s always used in a subordinate clause to contrast with the information given in the main clause of a sentence (e.g., ‘Amy continued to watch TV, in spite of the time’).
Despite is a preposition used to mean ‘ regardless of ‘, ‘notwithstanding’, or ‘even though’.
It’s used in a subordinate clause to contrast with information given in the main clause of a sentence (e.g., ‘Despite the stress, Joe loves his job’).
‘Log in’ is a phrasal verb meaning ‘connect to an electronic device, system, or app’. The preposition ‘to’ is often used directly after the verb; ‘in’ and ‘to’ should be written as two separate words (e.g., ‘ log in to the app to update privacy settings’).
‘Log into’ is sometimes used instead of ‘log in to’, but this is generally considered incorrect (as is ‘login to’).
Some synonyms and near synonyms of ensure include:
- Make certain
Some synonyms and near synonyms of assure include:
Rest assured is an expression meaning ‘you can be certain’ (e.g., ‘Rest assured, I will find your cat’). ‘Assured’ is the adjectival form of the verb assure , meaning ‘convince’ or ‘persuade’.
Some synonyms and near synonyms for council include:
There are numerous synonyms and near synonyms for the two meanings of counsel :
| Direct | Direction |
| Guide | Guidance |
| Instruct | Instruction |
AI writing tools can be used to perform a variety of tasks.
Generative AI writing tools (like ChatGPT ) generate text based on human inputs and can be used for interactive learning, to provide feedback, or to generate research questions or outlines.
These tools can also be used to paraphrase or summarise text or to identify grammar and punctuation mistakes. Y ou can also use Scribbr’s free paraphrasing tool , summarising tool , and grammar checker , which are designed specifically for these purposes.
Using AI writing tools (like ChatGPT ) to write your essay is usually considered plagiarism and may result in penalisation, unless it is allowed by your university. Text generated by AI tools is based on existing texts and therefore cannot provide unique insights. Furthermore, these outputs sometimes contain factual inaccuracies or grammar mistakes.
However, AI writing tools can be used effectively as a source of feedback and inspiration for your writing (e.g., to generate research questions ). Other AI tools, like grammar checkers, can help identify and eliminate grammar and punctuation mistakes to enhance your writing.
The Scribbr Knowledge Base is a collection of free resources to help you succeed in academic research, writing, and citation. Every week, we publish helpful step-by-step guides, clear examples, simple templates, engaging videos, and more.
The Knowledge Base is for students at all levels. Whether you’re writing your first essay, working on your bachelor’s or master’s dissertation, or getting to grips with your PhD research, we’ve got you covered.
As well as the Knowledge Base, Scribbr provides many other tools and services to support you in academic writing and citation:
- Create your citations and manage your reference list with our free Reference Generators in APA and MLA style.
- Scan your paper for in-text citation errors and inconsistencies with our innovative APA Citation Checker .
- Avoid accidental plagiarism with our reliable Plagiarism Checker .
- Polish your writing and get feedback on structure and clarity with our Proofreading & Editing services .
Yes! We’re happy for educators to use our content, and we’ve even adapted some of our articles into ready-made lecture slides .
You are free to display, distribute, and adapt Scribbr materials in your classes or upload them in private learning environments like Blackboard. We only ask that you credit Scribbr for any content you use.
We’re always striving to improve the Knowledge Base. If you have an idea for a topic we should cover, or you notice a mistake in any of our articles, let us know by emailing [email protected] .
The consequences of plagiarism vary depending on the type of plagiarism and the context in which it occurs. For example, submitting a whole paper by someone else will have the most severe consequences, while accidental citation errors are considered less serious.
If you’re a student, then you might fail the course, be suspended or expelled, or be obligated to attend a workshop on plagiarism. It depends on whether it’s your first offence or you’ve done it before.
As an academic or professional, plagiarising seriously damages your reputation. You might also lose your research funding or your job, and you could even face legal consequences for copyright infringement.
Paraphrasing without crediting the original author is a form of plagiarism , because you’re presenting someone else’s ideas as if they were your own.
However, paraphrasing is not plagiarism if you correctly reference the source . This means including an in-text referencing and a full reference , formatted according to your required citation style (e.g., Harvard , Vancouver ).
As well as referencing your source, make sure that any paraphrased text is completely rewritten in your own words.
Accidental plagiarism is one of the most common examples of plagiarism . Perhaps you forgot to cite a source, or paraphrased something a bit too closely. Maybe you can’t remember where you got an idea from, and aren’t totally sure if it’s original or not.
These all count as plagiarism, even though you didn’t do it on purpose. When in doubt, make sure you’re citing your sources . Also consider running your work through a plagiarism checker tool prior to submission, which work by using advanced database software to scan for matches between your text and existing texts.
Scribbr’s Plagiarism Checker takes less than 10 minutes and can help you turn in your paper with confidence.
The accuracy depends on the plagiarism checker you use. Per our in-depth research , Scribbr is the most accurate plagiarism checker. Many free plagiarism checkers fail to detect all plagiarism or falsely flag text as plagiarism.
Plagiarism checkers work by using advanced database software to scan for matches between your text and existing texts. Their accuracy is determined by two factors: the algorithm (which recognises the plagiarism) and the size of the database (with which your document is compared).
To avoid plagiarism when summarising an article or other source, follow these two rules:
- Write the summary entirely in your own words by paraphrasing the author’s ideas.
- Reference the source with an in-text citation and a full reference so your reader can easily find the original text.
Plagiarism can be detected by your professor or readers if the tone, formatting, or style of your text is different in different parts of your paper, or if they’re familiar with the plagiarised source.
Many universities also use plagiarism detection software like Turnitin’s, which compares your text to a large database of other sources, flagging any similarities that come up.
It can be easier than you think to commit plagiarism by accident. Consider using a plagiarism checker prior to submitting your essay to ensure you haven’t missed any citations.
Some examples of plagiarism include:
- Copying and pasting a Wikipedia article into the body of an assignment
- Quoting a source without including a citation
- Not paraphrasing a source properly (e.g. maintaining wording too close to the original)
- Forgetting to cite the source of an idea
The most surefire way to avoid plagiarism is to always cite your sources . When in doubt, cite!
Global plagiarism means taking an entire work written by someone else and passing it off as your own. This can include getting someone else to write an essay or assignment for you, or submitting a text you found online as your own work.
Global plagiarism is one of the most serious types of plagiarism because it involves deliberately and directly lying about the authorship of a work. It can have severe consequences for students and professionals alike.
Verbatim plagiarism means copying text from a source and pasting it directly into your own document without giving proper credit.
If the structure and the majority of the words are the same as in the original source, then you are committing verbatim plagiarism. This is the case even if you delete a few words or replace them with synonyms.
If you want to use an author’s exact words, you need to quote the original source by putting the copied text in quotation marks and including an in-text citation .
Patchwork plagiarism , also called mosaic plagiarism, means copying phrases, passages, or ideas from various existing sources and combining them to create a new text. This includes slightly rephrasing some of the content, while keeping many of the same words and the same structure as the original.
While this type of plagiarism is more insidious than simply copying and pasting directly from a source, plagiarism checkers like Turnitin’s can still easily detect it.
To avoid plagiarism in any form, remember to reference your sources .
Yes, reusing your own work without citation is considered self-plagiarism . This can range from resubmitting an entire assignment to reusing passages or data from something you’ve handed in previously.
Self-plagiarism often has the same consequences as other types of plagiarism . If you want to reuse content you wrote in the past, make sure to check your university’s policy or consult your professor.
If you are reusing content or data you used in a previous assignment, make sure to cite yourself. You can cite yourself the same way you would cite any other source: simply follow the directions for the citation style you are using.
Keep in mind that reusing prior content can be considered self-plagiarism , so make sure you ask your instructor or consult your university’s handbook prior to doing so.
Most institutions have an internal database of previously submitted student assignments. Turnitin can check for self-plagiarism by comparing your paper against this database. If you’ve reused parts of an assignment you already submitted, it will flag any similarities as potential plagiarism.
Online plagiarism checkers don’t have access to your institution’s database, so they can’t detect self-plagiarism of unpublished work. If you’re worried about accidentally self-plagiarising, you can use Scribbr’s Self-Plagiarism Checker to upload your unpublished documents and check them for similarities.
Plagiarism has serious consequences and can be illegal in certain scenarios.
While most of the time plagiarism in an undergraduate setting is not illegal, plagiarism or self-plagiarism in a professional academic setting can lead to legal action, including copyright infringement and fraud. Many scholarly journals do not allow you to submit the same work to more than one journal, and if you do not credit a coauthor, you could be legally defrauding them.
Even if you aren’t breaking the law, plagiarism can seriously impact your academic career. While the exact consequences of plagiarism vary by institution and severity, common consequences include a lower grade, automatically failing a course, academic suspension or probation, and even expulsion.
Self-plagiarism means recycling work that you’ve previously published or submitted as an assignment. It’s considered academic dishonesty to present something as brand new when you’ve already gotten credit and perhaps feedback for it in the past.
If you want to refer to ideas or data from previous work, be sure to cite yourself.
Academic integrity means being honest, ethical, and thorough in your academic work. To maintain academic integrity, you should avoid misleading your readers about any part of your research and refrain from offences like plagiarism and contract cheating, which are examples of academic misconduct.
Academic dishonesty refers to deceitful or misleading behavior in an academic setting. Academic dishonesty can occur intentionally or unintentionally, and it varies in severity.
It can encompass paying for a pre-written essay, cheating on an exam, or committing plagiarism . It can also include helping others cheat, copying a friend’s homework answers, or even pretending to be sick to miss an exam.
Academic dishonesty doesn’t just occur in a classroom setting, but also in research and other academic-adjacent fields.
Consequences of academic dishonesty depend on the severity of the offence and your institution’s policy. They can range from a warning for a first offence to a failing grade in a course to expulsion from your university.
For those in certain fields, such as nursing, engineering, or lab sciences, not learning fundamentals properly can directly impact the health and safety of others. For those working in academia or research, academic dishonesty impacts your professional reputation, leading others to doubt your future work.
Academic dishonesty can be intentional or unintentional, ranging from something as simple as claiming to have read something you didn’t to copying your neighbour’s answers on an exam.
You can commit academic dishonesty with the best of intentions, such as helping a friend cheat on a paper. Severe academic dishonesty can include buying a pre-written essay or the answers to a multiple-choice test, or falsifying a medical emergency to avoid taking a final exam.
Plagiarism means presenting someone else’s work as your own without giving proper credit to the original author. In academic writing, plagiarism involves using words, ideas, or information from a source without including a citation .
Plagiarism can have serious consequences , even when it’s done accidentally. To avoid plagiarism, it’s important to keep track of your sources and cite them correctly.
Common knowledge does not need to be cited. However, you should be extra careful when deciding what counts as common knowledge.
Common knowledge encompasses information that the average educated reader would accept as true without needing the extra validation of a source or citation.
Common knowledge should be widely known, undisputed, and easily verified. When in doubt, always cite your sources.
Most online plagiarism checkers only have access to public databases, whose software doesn’t allow you to compare two documents for plagiarism.
However, in addition to our Plagiarism Checker , Scribbr also offers an Self-Plagiarism Checker . This is an add-on tool that lets you compare your paper with unpublished or private documents. This way you can rest assured that you haven’t unintentionally plagiarised or self-plagiarised .
Compare two sources for plagiarism
The research methods you use depend on the type of data you need to answer your research question .
- If you want to measure something or test a hypothesis , use quantitative methods . If you want to explore ideas, thoughts, and meanings, use qualitative methods .
- If you want to analyse a large amount of readily available data, use secondary data. If you want data specific to your purposes with control over how they are generated, collect primary data.
- If you want to establish cause-and-effect relationships between variables , use experimental methods. If you want to understand the characteristics of a research subject, use descriptive methods.
Methodology refers to the overarching strategy and rationale of your research project . It involves studying the methods used in your field and the theories or principles behind them, in order to develop an approach that matches your objectives.
Methods are the specific tools and procedures you use to collect and analyse data (e.g. experiments, surveys , and statistical tests ).
In shorter scientific papers, where the aim is to report the findings of a specific study, you might simply describe what you did in a methods section .
In a longer or more complex research project, such as a thesis or dissertation , you will probably include a methodology section , where you explain your approach to answering the research questions and cite relevant sources to support your choice of methods.
In mixed methods research , you use both qualitative and quantitative data collection and analysis methods to answer your research question .
Data collection is the systematic process by which observations or measurements are gathered in research. It is used in many different contexts by academics, governments, businesses, and other organisations.
There are various approaches to qualitative data analysis , but they all share five steps in common:
- Prepare and organise your data.
- Review and explore your data.
- Develop a data coding system.
- Assign codes to the data.
- Identify recurring themes.
The specifics of each step depend on the focus of the analysis. Some common approaches include textual analysis , thematic analysis , and discourse analysis .
There are five common approaches to qualitative research :
- Grounded theory involves collecting data in order to develop new theories.
- Ethnography involves immersing yourself in a group or organisation to understand its culture.
- Narrative research involves interpreting stories to understand how people make sense of their experiences and perceptions.
- Phenomenological research involves investigating phenomena through people’s lived experiences.
- Action research links theory and practice in several cycles to drive innovative changes.
Hypothesis testing is a formal procedure for investigating our ideas about the world using statistics. It is used by scientists to test specific predictions, called hypotheses , by calculating how likely it is that a pattern or relationship between variables could have arisen by chance.
Operationalisation means turning abstract conceptual ideas into measurable observations.
For example, the concept of social anxiety isn’t directly observable, but it can be operationally defined in terms of self-rating scores, behavioural avoidance of crowded places, or physical anxiety symptoms in social situations.
Before collecting data , it’s important to consider how you will operationalise the variables that you want to measure.
Triangulation in research means using multiple datasets, methods, theories and/or investigators to address a research question. It’s a research strategy that can help you enhance the validity and credibility of your findings.
Triangulation is mainly used in qualitative research , but it’s also commonly applied in quantitative research . Mixed methods research always uses triangulation.
These are four of the most common mixed methods designs :
- Convergent parallel: Quantitative and qualitative data are collected at the same time and analysed separately. After both analyses are complete, compare your results to draw overall conclusions.
- Embedded: Quantitative and qualitative data are collected at the same time, but within a larger quantitative or qualitative design. One type of data is secondary to the other.
- Explanatory sequential: Quantitative data is collected and analysed first, followed by qualitative data. You can use this design if you think your qualitative data will explain and contextualise your quantitative findings.
- Exploratory sequential: Qualitative data is collected and analysed first, followed by quantitative data. You can use this design if you think the quantitative data will confirm or validate your qualitative findings.
An observational study could be a good fit for your research if your research question is based on things you observe. If you have ethical, logistical, or practical concerns that make an experimental design challenging, consider an observational study. Remember that in an observational study, it is critical that there be no interference or manipulation of the research subjects. Since it’s not an experiment, there are no control or treatment groups either.
The key difference between observational studies and experiments is that, done correctly, an observational study will never influence the responses or behaviours of participants. Experimental designs will have a treatment condition applied to at least a portion of participants.
Exploratory research explores the main aspects of a new or barely researched question.
Explanatory research explains the causes and effects of an already widely researched question.
Experimental designs are a set of procedures that you plan in order to examine the relationship between variables that interest you.
To design a successful experiment, first identify:
- A testable hypothesis
- One or more independent variables that you will manipulate
- One or more dependent variables that you will measure
When designing the experiment, first decide:
- How your variable(s) will be manipulated
- How you will control for any potential confounding or lurking variables
- How many subjects you will include
- How you will assign treatments to your subjects
There are four main types of triangulation :
- Data triangulation : Using data from different times, spaces, and people
- Investigator triangulation : Involving multiple researchers in collecting or analysing data
- Theory triangulation : Using varying theoretical perspectives in your research
- Methodological triangulation : Using different methodologies to approach the same topic
Triangulation can help:
- Reduce bias that comes from using a single method, theory, or investigator
- Enhance validity by approaching the same topic with different tools
- Establish credibility by giving you a complete picture of the research problem
But triangulation can also pose problems:
- It’s time-consuming and labour-intensive, often involving an interdisciplinary team.
- Your results may be inconsistent or even contradictory.
A confounding variable , also called a confounder or confounding factor, is a third variable in a study examining a potential cause-and-effect relationship.
A confounding variable is related to both the supposed cause and the supposed effect of the study. It can be difficult to separate the true effect of the independent variable from the effect of the confounding variable.
In your research design , it’s important to identify potential confounding variables and plan how you will reduce their impact.
In a between-subjects design , every participant experiences only one condition, and researchers assess group differences between participants in various conditions.
In a within-subjects design , each participant experiences all conditions, and researchers test the same participants repeatedly for differences between conditions.
The word ‘between’ means that you’re comparing different conditions between groups, while the word ‘within’ means you’re comparing different conditions within the same group.
A quasi-experiment is a type of research design that attempts to establish a cause-and-effect relationship. The main difference between this and a true experiment is that the groups are not randomly assigned.
In experimental research, random assignment is a way of placing participants from your sample into different groups using randomisation. With this method, every member of the sample has a known or equal chance of being placed in a control group or an experimental group.
Quasi-experimental design is most useful in situations where it would be unethical or impractical to run a true experiment .
Quasi-experiments have lower internal validity than true experiments, but they often have higher external validity as they can use real-world interventions instead of artificial laboratory settings.
Within-subjects designs have many potential threats to internal validity , but they are also very statistically powerful .
Advantages:
- Only requires small samples
- Statistically powerful
- Removes the effects of individual differences on the outcomes
Disadvantages:
- Internal validity threats reduce the likelihood of establishing a direct relationship between variables
- Time-related effects, such as growth, can influence the outcomes
- Carryover effects mean that the specific order of different treatments affect the outcomes
Yes. Between-subjects and within-subjects designs can be combined in a single study when you have two or more independent variables (a factorial design). In a mixed factorial design, one variable is altered between subjects and another is altered within subjects.
In a factorial design, multiple independent variables are tested.
If you test two variables, each level of one independent variable is combined with each level of the other independent variable to create different conditions.
While a between-subjects design has fewer threats to internal validity , it also requires more participants for high statistical power than a within-subjects design .
- Prevents carryover effects of learning and fatigue.
- Shorter study duration.
- Needs larger samples for high power.
- Uses more resources to recruit participants, administer sessions, cover costs, etc.
- Individual differences may be an alternative explanation for results.
Samples are used to make inferences about populations . Samples are easier to collect data from because they are practical, cost-effective, convenient, and manageable.
Probability sampling means that every member of the target population has a known chance of being included in the sample.
Probability sampling methods include simple random sampling , systematic sampling , stratified sampling , and cluster sampling .
In non-probability sampling , the sample is selected based on non-random criteria, and not every member of the population has a chance of being included.
Common non-probability sampling methods include convenience sampling , voluntary response sampling, purposive sampling , snowball sampling , and quota sampling .
In multistage sampling , or multistage cluster sampling, you draw a sample from a population using smaller and smaller groups at each stage.
This method is often used to collect data from a large, geographically spread group of people in national surveys, for example. You take advantage of hierarchical groupings (e.g., from county to city to neighbourhood) to create a sample that’s less expensive and time-consuming to collect data from.
Sampling bias occurs when some members of a population are systematically more likely to be selected in a sample than others.
Simple random sampling is a type of probability sampling in which the researcher randomly selects a subset of participants from a population . Each member of the population has an equal chance of being selected. Data are then collected from as large a percentage as possible of this random subset.
The American Community Survey is an example of simple random sampling . In order to collect detailed data on the population of the US, the Census Bureau officials randomly select 3.5 million households per year and use a variety of methods to convince them to fill out the survey.
If properly implemented, simple random sampling is usually the best sampling method for ensuring both internal and external validity . However, it can sometimes be impractical and expensive to implement, depending on the size of the population to be studied,
If you have a list of every member of the population and the ability to reach whichever members are selected, you can use simple random sampling.
Cluster sampling is more time- and cost-efficient than other probability sampling methods , particularly when it comes to large samples spread across a wide geographical area.
However, it provides less statistical certainty than other methods, such as simple random sampling , because it is difficult to ensure that your clusters properly represent the population as a whole.
There are three types of cluster sampling : single-stage, double-stage and multi-stage clustering. In all three types, you first divide the population into clusters, then randomly select clusters for use in your sample.
- In single-stage sampling , you collect data from every unit within the selected clusters.
- In double-stage sampling , you select a random sample of units from within the clusters.
- In multi-stage sampling , you repeat the procedure of randomly sampling elements from within the clusters until you have reached a manageable sample.
Cluster sampling is a probability sampling method in which you divide a population into clusters, such as districts or schools, and then randomly select some of these clusters as your sample.
The clusters should ideally each be mini-representations of the population as a whole.
In multistage sampling , you can use probability or non-probability sampling methods.
For a probability sample, you have to probability sampling at every stage. You can mix it up by using simple random sampling , systematic sampling , or stratified sampling to select units at different stages, depending on what is applicable and relevant to your study.
Multistage sampling can simplify data collection when you have large, geographically spread samples, and you can obtain a probability sample without a complete sampling frame.
But multistage sampling may not lead to a representative sample, and larger samples are needed for multistage samples to achieve the statistical properties of simple random samples .
In stratified sampling , researchers divide subjects into subgroups called strata based on characteristics that they share (e.g., race, gender, educational attainment).
Once divided, each subgroup is randomly sampled using another probability sampling method .
You should use stratified sampling when your sample can be divided into mutually exclusive and exhaustive subgroups that you believe will take on different mean values for the variable that you’re studying.
Using stratified sampling will allow you to obtain more precise (with lower variance ) statistical estimates of whatever you are trying to measure.
For example, say you want to investigate how income differs based on educational attainment, but you know that this relationship can vary based on race. Using stratified sampling, you can ensure you obtain a large enough sample from each racial group, allowing you to draw more precise conclusions.
Yes, you can create a stratified sample using multiple characteristics, but you must ensure that every participant in your study belongs to one and only one subgroup. In this case, you multiply the numbers of subgroups for each characteristic to get the total number of groups.
For example, if you were stratifying by location with three subgroups (urban, rural, or suburban) and marital status with five subgroups (single, divorced, widowed, married, or partnered), you would have 3 × 5 = 15 subgroups.
There are three key steps in systematic sampling :
- Define and list your population , ensuring that it is not ordered in a cyclical or periodic order.
- Decide on your sample size and calculate your interval, k , by dividing your population by your target sample size.
- Choose every k th member of the population as your sample.
Systematic sampling is a probability sampling method where researchers select members of the population at a regular interval – for example, by selecting every 15th person on a list of the population. If the population is in a random order, this can imitate the benefits of simple random sampling .
Populations are used when a research question requires data from every member of the population. This is usually only feasible when the population is small and easily accessible.
A statistic refers to measures about the sample , while a parameter refers to measures about the population .
A sampling error is the difference between a population parameter and a sample statistic .
There are eight threats to internal validity : history, maturation, instrumentation, testing, selection bias , regression to the mean, social interaction, and attrition .
Internal validity is the extent to which you can be confident that a cause-and-effect relationship established in a study cannot be explained by other factors.
Attrition bias is a threat to internal validity . In experiments, differential rates of attrition between treatment and control groups can skew results.
This bias can affect the relationship between your independent and dependent variables . It can make variables appear to be correlated when they are not, or vice versa.
The external validity of a study is the extent to which you can generalise your findings to different groups of people, situations, and measures.
The two types of external validity are population validity (whether you can generalise to other groups of people) and ecological validity (whether you can generalise to other situations and settings).
There are seven threats to external validity : selection bias , history, experimenter effect, Hawthorne effect , testing effect, aptitude-treatment, and situation effect.
Attrition bias can skew your sample so that your final sample differs significantly from your original sample. Your sample is biased because some groups from your population are underrepresented.
With a biased final sample, you may not be able to generalise your findings to the original population that you sampled from, so your external validity is compromised.
Construct validity is about how well a test measures the concept it was designed to evaluate. It’s one of four types of measurement validity , which includes construct validity, face validity , and criterion validity.
There are two subtypes of construct validity.
- Convergent validity : The extent to which your measure corresponds to measures of related constructs
- Discriminant validity: The extent to which your measure is unrelated or negatively related to measures of distinct constructs
When designing or evaluating a measure, construct validity helps you ensure you’re actually measuring the construct you’re interested in. If you don’t have construct validity, you may inadvertently measure unrelated or distinct constructs and lose precision in your research.
Construct validity is often considered the overarching type of measurement validity , because it covers all of the other types. You need to have face validity , content validity, and criterion validity to achieve construct validity.
Statistical analyses are often applied to test validity with data from your measures. You test convergent validity and discriminant validity with correlations to see if results from your test are positively or negatively related to those of other established tests.
You can also use regression analyses to assess whether your measure is actually predictive of outcomes that you expect it to predict theoretically. A regression analysis that supports your expectations strengthens your claim of construct validity .
Face validity is about whether a test appears to measure what it’s supposed to measure. This type of validity is concerned with whether a measure seems relevant and appropriate for what it’s assessing only on the surface.
Face validity is important because it’s a simple first step to measuring the overall validity of a test or technique. It’s a relatively intuitive, quick, and easy way to start checking whether a new measure seems useful at first glance.
Good face validity means that anyone who reviews your measure says that it seems to be measuring what it’s supposed to. With poor face validity, someone reviewing your measure may be left confused about what you’re measuring and why you’re using this method.
It’s often best to ask a variety of people to review your measurements. You can ask experts, such as other researchers, or laypeople, such as potential participants, to judge the face validity of tests.
While experts have a deep understanding of research methods , the people you’re studying can provide you with valuable insights you may have missed otherwise.
There are many different types of inductive reasoning that people use formally or informally.
Here are a few common types:
- Inductive generalisation : You use observations about a sample to come to a conclusion about the population it came from.
- Statistical generalisation: You use specific numbers about samples to make statements about populations.
- Causal reasoning: You make cause-and-effect links between different things.
- Sign reasoning: You make a conclusion about a correlational relationship between different things.
- Analogical reasoning: You make a conclusion about something based on its similarities to something else.
Inductive reasoning is a bottom-up approach, while deductive reasoning is top-down.
Inductive reasoning takes you from the specific to the general, while in deductive reasoning, you make inferences by going from general premises to specific conclusions.
In inductive research , you start by making observations or gathering data. Then, you take a broad scan of your data and search for patterns. Finally, you make general conclusions that you might incorporate into theories.
Inductive reasoning is a method of drawing conclusions by going from the specific to the general. It’s usually contrasted with deductive reasoning, where you proceed from general information to specific conclusions.
Inductive reasoning is also called inductive logic or bottom-up reasoning.
Deductive reasoning is a logical approach where you progress from general ideas to specific conclusions. It’s often contrasted with inductive reasoning , where you start with specific observations and form general conclusions.
Deductive reasoning is also called deductive logic.
Deductive reasoning is commonly used in scientific research, and it’s especially associated with quantitative research .
In research, you might have come across something called the hypothetico-deductive method . It’s the scientific method of testing hypotheses to check whether your predictions are substantiated by real-world data.
A dependent variable is what changes as a result of the independent variable manipulation in experiments . It’s what you’re interested in measuring, and it ‘depends’ on your independent variable.
In statistics, dependent variables are also called:
- Response variables (they respond to a change in another variable)
- Outcome variables (they represent the outcome you want to measure)
- Left-hand-side variables (they appear on the left-hand side of a regression equation)
An independent variable is the variable you manipulate, control, or vary in an experimental study to explore its effects. It’s called ‘independent’ because it’s not influenced by any other variables in the study.
Independent variables are also called:
- Explanatory variables (they explain an event or outcome)
- Predictor variables (they can be used to predict the value of a dependent variable)
- Right-hand-side variables (they appear on the right-hand side of a regression equation)
A correlation is usually tested for two variables at a time, but you can test correlations between three or more variables.
On graphs, the explanatory variable is conventionally placed on the x -axis, while the response variable is placed on the y -axis.
- If you have quantitative variables , use a scatterplot or a line graph.
- If your response variable is categorical, use a scatterplot or a line graph.
- If your explanatory variable is categorical, use a bar graph.
The term ‘ explanatory variable ‘ is sometimes preferred over ‘ independent variable ‘ because, in real-world contexts, independent variables are often influenced by other variables. This means they aren’t totally independent.
Multiple independent variables may also be correlated with each other, so ‘explanatory variables’ is a more appropriate term.
The difference between explanatory and response variables is simple:
- An explanatory variable is the expected cause, and it explains the results.
- A response variable is the expected effect, and it responds to other variables.
There are 4 main types of extraneous variables :
- Demand characteristics : Environmental cues that encourage participants to conform to researchers’ expectations
- Experimenter effects : Unintentional actions by researchers that influence study outcomes
- Situational variables : Eenvironmental variables that alter participants’ behaviours
- Participant variables : Any characteristic or aspect of a participant’s background that could affect study results
An extraneous variable is any variable that you’re not investigating that can potentially affect the dependent variable of your research study.
A confounding variable is a type of extraneous variable that not only affects the dependent variable, but is also related to the independent variable.
‘Controlling for a variable’ means measuring extraneous variables and accounting for them statistically to remove their effects on other variables.
Researchers often model control variable data along with independent and dependent variable data in regression analyses and ANCOVAs . That way, you can isolate the control variable’s effects from the relationship between the variables of interest.
Control variables help you establish a correlational or causal relationship between variables by enhancing internal validity .
If you don’t control relevant extraneous variables , they may influence the outcomes of your study, and you may not be able to demonstrate that your results are really an effect of your independent variable .
A control variable is any variable that’s held constant in a research study. It’s not a variable of interest in the study, but it’s controlled because it could influence the outcomes.
In statistics, ordinal and nominal variables are both considered categorical variables .
Even though ordinal data can sometimes be numerical, not all mathematical operations can be performed on them.
In scientific research, concepts are the abstract ideas or phenomena that are being studied (e.g., educational achievement). Variables are properties or characteristics of the concept (e.g., performance at school), while indicators are ways of measuring or quantifying variables (e.g., yearly grade reports).
The process of turning abstract concepts into measurable variables and indicators is called operationalisation .
There are several methods you can use to decrease the impact of confounding variables on your research: restriction, matching, statistical control, and randomisation.
In restriction , you restrict your sample by only including certain subjects that have the same values of potential confounding variables.
In matching , you match each of the subjects in your treatment group with a counterpart in the comparison group. The matched subjects have the same values on any potential confounding variables, and only differ in the independent variable .
In statistical control , you include potential confounders as variables in your regression .
In randomisation , you randomly assign the treatment (or independent variable) in your study to a sufficiently large number of subjects, which allows you to control for all potential confounding variables.
A confounding variable is closely related to both the independent and dependent variables in a study. An independent variable represents the supposed cause , while the dependent variable is the supposed effect . A confounding variable is a third variable that influences both the independent and dependent variables.
Failing to account for confounding variables can cause you to wrongly estimate the relationship between your independent and dependent variables.
To ensure the internal validity of your research, you must consider the impact of confounding variables. If you fail to account for them, you might over- or underestimate the causal relationship between your independent and dependent variables , or even find a causal relationship where none exists.
Yes, but including more than one of either type requires multiple research questions .
For example, if you are interested in the effect of a diet on health, you can use multiple measures of health: blood sugar, blood pressure, weight, pulse, and many more. Each of these is its own dependent variable with its own research question.
You could also choose to look at the effect of exercise levels as well as diet, or even the additional effect of the two combined. Each of these is a separate independent variable .
To ensure the internal validity of an experiment , you should only change one independent variable at a time.
No. The value of a dependent variable depends on an independent variable, so a variable cannot be both independent and dependent at the same time. It must be either the cause or the effect, not both.
You want to find out how blood sugar levels are affected by drinking diet cola and regular cola, so you conduct an experiment .
- The type of cola – diet or regular – is the independent variable .
- The level of blood sugar that you measure is the dependent variable – it changes depending on the type of cola.
Determining cause and effect is one of the most important parts of scientific research. It’s essential to know which is the cause – the independent variable – and which is the effect – the dependent variable.
Quantitative variables are any variables where the data represent amounts (e.g. height, weight, or age).
Categorical variables are any variables where the data represent groups. This includes rankings (e.g. finishing places in a race), classifications (e.g. brands of cereal), and binary outcomes (e.g. coin flips).
You need to know what type of variables you are working with to choose the right statistical test for your data and interpret your results .
Discrete and continuous variables are two types of quantitative variables :
- Discrete variables represent counts (e.g., the number of objects in a collection).
- Continuous variables represent measurable amounts (e.g., water volume or weight).
You can think of independent and dependent variables in terms of cause and effect: an independent variable is the variable you think is the cause , while a dependent variable is the effect .
In an experiment, you manipulate the independent variable and measure the outcome in the dependent variable. For example, in an experiment about the effect of nutrients on crop growth:
- The independent variable is the amount of nutrients added to the crop field.
- The dependent variable is the biomass of the crops at harvest time.
Defining your variables, and deciding how you will manipulate and measure them, is an important part of experimental design .
Including mediators and moderators in your research helps you go beyond studying a simple relationship between two variables for a fuller picture of the real world. They are important to consider when studying complex correlational or causal relationships.
Mediators are part of the causal pathway of an effect, and they tell you how or why an effect takes place. Moderators usually help you judge the external validity of your study by identifying the limitations of when the relationship between variables holds.
If something is a mediating variable :
- It’s caused by the independent variable
- It influences the dependent variable
- When it’s taken into account, the statistical correlation between the independent and dependent variables is higher than when it isn’t considered
A confounder is a third variable that affects variables of interest and makes them seem related when they are not. In contrast, a mediator is the mechanism of a relationship between two variables: it explains the process by which they are related.
A mediator variable explains the process through which two variables are related, while a moderator variable affects the strength and direction of that relationship.
When conducting research, collecting original data has significant advantages:
- You can tailor data collection to your specific research aims (e.g., understanding the needs of your consumers or user testing your website).
- You can control and standardise the process for high reliability and validity (e.g., choosing appropriate measurements and sampling methods ).
However, there are also some drawbacks: data collection can be time-consuming, labour-intensive, and expensive. In some cases, it’s more efficient to use secondary data that has already been collected by someone else, but the data might be less reliable.
A structured interview is a data collection method that relies on asking questions in a set order to collect data on a topic. They are often quantitative in nature. Structured interviews are best used when:
- You already have a very clear understanding of your topic. Perhaps significant research has already been conducted, or you have done some prior research yourself, but you already possess a baseline for designing strong structured questions.
- You are constrained in terms of time or resources and need to analyse your data quickly and efficiently
- Your research question depends on strong parity between participants, with environmental conditions held constant
More flexible interview options include semi-structured interviews , unstructured interviews , and focus groups .
The interviewer effect is a type of bias that emerges when a characteristic of an interviewer (race, age, gender identity, etc.) influences the responses given by the interviewee.
There is a risk of an interviewer effect in all types of interviews , but it can be mitigated by writing really high-quality interview questions.
A semi-structured interview is a blend of structured and unstructured types of interviews. Semi-structured interviews are best used when:
- You have prior interview experience. Spontaneous questions are deceptively challenging, and it’s easy to accidentally ask a leading question or make a participant uncomfortable.
- Your research question is exploratory in nature. Participant answers can guide future research questions and help you develop a more robust knowledge base for future research.
An unstructured interview is the most flexible type of interview, but it is not always the best fit for your research topic.
Unstructured interviews are best used when:
- You are an experienced interviewer and have a very strong background in your research topic, since it is challenging to ask spontaneous, colloquial questions
- Your research question is exploratory in nature. While you may have developed hypotheses, you are open to discovering new or shifting viewpoints through the interview process.
- You are seeking descriptive data, and are ready to ask questions that will deepen and contextualise your initial thoughts and hypotheses
- Your research depends on forming connections with your participants and making them feel comfortable revealing deeper emotions, lived experiences, or thoughts
The four most common types of interviews are:
- Structured interviews : The questions are predetermined in both topic and order.
- Semi-structured interviews : A few questions are predetermined, but other questions aren’t planned.
- Unstructured interviews : None of the questions are predetermined.
- Focus group interviews : The questions are presented to a group instead of one individual.
A focus group is a research method that brings together a small group of people to answer questions in a moderated setting. The group is chosen due to predefined demographic traits, and the questions are designed to shed light on a topic of interest. It is one of four types of interviews .
Social desirability bias is the tendency for interview participants to give responses that will be viewed favourably by the interviewer or other participants. It occurs in all types of interviews and surveys , but is most common in semi-structured interviews , unstructured interviews , and focus groups .
Social desirability bias can be mitigated by ensuring participants feel at ease and comfortable sharing their views. Make sure to pay attention to your own body language and any physical or verbal cues, such as nodding or widening your eyes.
This type of bias in research can also occur in observations if the participants know they’re being observed. They might alter their behaviour accordingly.
As a rule of thumb, questions related to thoughts, beliefs, and feelings work well in focus groups . Take your time formulating strong questions, paying special attention to phrasing. Be careful to avoid leading questions , which can bias your responses.
Overall, your focus group questions should be:
- Open-ended and flexible
- Impossible to answer with ‘yes’ or ‘no’ (questions that start with ‘why’ or ‘how’ are often best)
- Unambiguous, getting straight to the point while still stimulating discussion
- Unbiased and neutral
The third variable and directionality problems are two main reasons why correlation isn’t causation .
The third variable problem means that a confounding variable affects both variables to make them seem causally related when they are not.
The directionality problem is when two variables correlate and might actually have a causal relationship, but it’s impossible to conclude which variable causes changes in the other.
Controlled experiments establish causality, whereas correlational studies only show associations between variables.
- In an experimental design , you manipulate an independent variable and measure its effect on a dependent variable. Other variables are controlled so they can’t impact the results.
- In a correlational design , you measure variables without manipulating any of them. You can test whether your variables change together, but you can’t be sure that one variable caused a change in another.
In general, correlational research is high in external validity while experimental research is high in internal validity .
A correlation coefficient is a single number that describes the strength and direction of the relationship between your variables.
Different types of correlation coefficients might be appropriate for your data based on their levels of measurement and distributions . The Pearson product-moment correlation coefficient (Pearson’s r ) is commonly used to assess a linear relationship between two quantitative variables.
A correlational research design investigates relationships between two variables (or more) without the researcher controlling or manipulating any of them. It’s a non-experimental type of quantitative research .
A correlation reflects the strength and/or direction of the association between two or more variables.
- A positive correlation means that both variables change in the same direction.
- A negative correlation means that the variables change in opposite directions.
- A zero correlation means there’s no relationship between the variables.
Longitudinal studies can last anywhere from weeks to decades, although they tend to be at least a year long.
The 1970 British Cohort Study , which has collected data on the lives of 17,000 Brits since their births in 1970, is one well-known example of a longitudinal study .
Longitudinal studies are better to establish the correct sequence of events, identify changes over time, and provide insight into cause-and-effect relationships, but they also tend to be more expensive and time-consuming than other types of studies.
Longitudinal studies and cross-sectional studies are two different types of research design . In a cross-sectional study you collect data from a population at a specific point in time; in a longitudinal study you repeatedly collect data from the same sample over an extended period of time.
| Longitudinal study | Cross-sectional study |
|---|---|
| observations | Observations at a in time |
| Observes the multiple times | Observes (a ‘cross-section’) in the population |
| Follows in participants over time | Provides of society at a given point |
Cross-sectional studies cannot establish a cause-and-effect relationship or analyse behaviour over a period of time. To investigate cause and effect, you need to do a longitudinal study or an experimental study .
Cross-sectional studies are less expensive and time-consuming than many other types of study. They can provide useful insights into a population’s characteristics and identify correlations for further research.
Sometimes only cross-sectional data are available for analysis; other times your research question may only require a cross-sectional study to answer it.
A hypothesis states your predictions about what your research will find. It is a tentative answer to your research question that has not yet been tested. For some research projects, you might have to write several hypotheses that address different aspects of your research question.
A hypothesis is not just a guess. It should be based on existing theories and knowledge. It also has to be testable, which means you can support or refute it through scientific research methods (such as experiments, observations, and statistical analysis of data).
A research hypothesis is your proposed answer to your research question. The research hypothesis usually includes an explanation (‘ x affects y because …’).
A statistical hypothesis, on the other hand, is a mathematical statement about a population parameter. Statistical hypotheses always come in pairs: the null and alternative hypotheses. In a well-designed study , the statistical hypotheses correspond logically to the research hypothesis.
Individual Likert-type questions are generally considered ordinal data , because the items have clear rank order, but don’t have an even distribution.
Overall Likert scale scores are sometimes treated as interval data. These scores are considered to have directionality and even spacing between them.
The type of data determines what statistical tests you should use to analyse your data.
A Likert scale is a rating scale that quantitatively assesses opinions, attitudes, or behaviours. It is made up of four or more questions that measure a single attitude or trait when response scores are combined.
To use a Likert scale in a survey , you present participants with Likert-type questions or statements, and a continuum of items, usually with five or seven possible responses, to capture their degree of agreement.
A questionnaire is a data collection tool or instrument, while a survey is an overarching research method that involves collecting and analysing data from people using questionnaires.
A true experiment (aka a controlled experiment) always includes at least one control group that doesn’t receive the experimental treatment.
However, some experiments use a within-subjects design to test treatments without a control group. In these designs, you usually compare one group’s outcomes before and after a treatment (instead of comparing outcomes between different groups).
For strong internal validity , it’s usually best to include a control group if possible. Without a control group, it’s harder to be certain that the outcome was caused by the experimental treatment and not by other variables.
An experimental group, also known as a treatment group, receives the treatment whose effect researchers wish to study, whereas a control group does not. They should be identical in all other ways.
In a controlled experiment , all extraneous variables are held constant so that they can’t influence the results. Controlled experiments require:
- A control group that receives a standard treatment, a fake treatment, or no treatment
- Random assignment of participants to ensure the groups are equivalent
Depending on your study topic, there are various other methods of controlling variables .
Questionnaires can be self-administered or researcher-administered.
Self-administered questionnaires can be delivered online or in paper-and-pen formats, in person or by post. All questions are standardised so that all respondents receive the same questions with identical wording.
Researcher-administered questionnaires are interviews that take place by phone, in person, or online between researchers and respondents. You can gain deeper insights by clarifying questions for respondents or asking follow-up questions.
You can organise the questions logically, with a clear progression from simple to complex, or randomly between respondents. A logical flow helps respondents process the questionnaire easier and quicker, but it may lead to bias. Randomisation can minimise the bias from order effects.
Closed-ended, or restricted-choice, questions offer respondents a fixed set of choices to select from. These questions are easier to answer quickly.
Open-ended or long-form questions allow respondents to answer in their own words. Because there are no restrictions on their choices, respondents can answer in ways that researchers may not have otherwise considered.
Naturalistic observation is a qualitative research method where you record the behaviours of your research subjects in real-world settings. You avoid interfering or influencing anything in a naturalistic observation.
You can think of naturalistic observation as ‘people watching’ with a purpose.
Naturalistic observation is a valuable tool because of its flexibility, external validity , and suitability for topics that can’t be studied in a lab setting.
The downsides of naturalistic observation include its lack of scientific control , ethical considerations , and potential for bias from observers and subjects.
You can use several tactics to minimise observer bias .
- Use masking (blinding) to hide the purpose of your study from all observers.
- Triangulate your data with different data collection methods or sources.
- Use multiple observers and ensure inter-rater reliability.
- Train your observers to make sure data is consistently recorded between them.
- Standardise your observation procedures to make sure they are structured and clear.
The observer-expectancy effect occurs when researchers influence the results of their own study through interactions with participants.
Researchers’ own beliefs and expectations about the study results may unintentionally influence participants through demand characteristics .
Observer bias occurs when a researcher’s expectations, opinions, or prejudices influence what they perceive or record in a study. It usually affects studies when observers are aware of the research aims or hypotheses. This type of research bias is also called detection bias or ascertainment bias .
Data cleaning is necessary for valid and appropriate analyses. Dirty data contain inconsistencies or errors , but cleaning your data helps you minimise or resolve these.
Without data cleaning, you could end up with a Type I or II error in your conclusion. These types of erroneous conclusions can be practically significant with important consequences, because they lead to misplaced investments or missed opportunities.
Data cleaning involves spotting and resolving potential data inconsistencies or errors to improve your data quality. An error is any value (e.g., recorded weight) that doesn’t reflect the true value (e.g., actual weight) of something that’s being measured.
In this process, you review, analyse, detect, modify, or remove ‘dirty’ data to make your dataset ‘clean’. Data cleaning is also called data cleansing or data scrubbing.
Data cleaning takes place between data collection and data analyses. But you can use some methods even before collecting data.
For clean data, you should start by designing measures that collect valid data. Data validation at the time of data entry or collection helps you minimize the amount of data cleaning you’ll need to do.
After data collection, you can use data standardisation and data transformation to clean your data. You’ll also deal with any missing values, outliers, and duplicate values.
Clean data are valid, accurate, complete, consistent, unique, and uniform. Dirty data include inconsistencies and errors.
Dirty data can come from any part of the research process, including poor research design , inappropriate measurement materials, or flawed data entry.
Random assignment is used in experiments with a between-groups or independent measures design. In this research design, there’s usually a control group and one or more experimental groups. Random assignment helps ensure that the groups are comparable.
In general, you should always use random assignment in this type of experimental design when it is ethically possible and makes sense for your study topic.
Random selection, or random sampling , is a way of selecting members of a population for your study’s sample.
In contrast, random assignment is a way of sorting the sample into control and experimental groups.
Random sampling enhances the external validity or generalisability of your results, while random assignment improves the internal validity of your study.
To implement random assignment , assign a unique number to every member of your study’s sample .
Then, you can use a random number generator or a lottery method to randomly assign each number to a control or experimental group. You can also do so manually, by flipping a coin or rolling a die to randomly assign participants to groups.
Exploratory research is often used when the issue you’re studying is new or when the data collection process is challenging for some reason.
You can use exploratory research if you have a general idea or a specific question that you want to study but there is no preexisting knowledge or paradigm with which to study it.
Exploratory research is a methodology approach that explores research questions that have not previously been studied in depth. It is often used when the issue you’re studying is new, or the data collection process is challenging in some way.
Explanatory research is used to investigate how or why a phenomenon occurs. Therefore, this type of research is often one of the first stages in the research process , serving as a jumping-off point for future research.
Explanatory research is a research method used to investigate how or why something occurs when only a small amount of information is available pertaining to that topic. It can help you increase your understanding of a given topic.
Blinding means hiding who is assigned to the treatment group and who is assigned to the control group in an experiment .
Blinding is important to reduce bias (e.g., observer bias , demand characteristics ) and ensure a study’s internal validity .
If participants know whether they are in a control or treatment group , they may adjust their behaviour in ways that affect the outcome that researchers are trying to measure. If the people administering the treatment are aware of group assignment, they may treat participants differently and thus directly or indirectly influence the final results.
- In a single-blind study , only the participants are blinded.
- In a double-blind study , both participants and experimenters are blinded.
- In a triple-blind study , the assignment is hidden not only from participants and experimenters, but also from the researchers analysing the data.
Many academic fields use peer review , largely to determine whether a manuscript is suitable for publication. Peer review enhances the credibility of the published manuscript.
However, peer review is also common in non-academic settings. The United Nations, the European Union, and many individual nations use peer review to evaluate grant applications. It is also widely used in medical and health-related fields as a teaching or quality-of-care measure.
Peer assessment is often used in the classroom as a pedagogical tool. Both receiving feedback and providing it are thought to enhance the learning process, helping students think critically and collaboratively.
Peer review can stop obviously problematic, falsified, or otherwise untrustworthy research from being published. It also represents an excellent opportunity to get feedback from renowned experts in your field.
It acts as a first defence, helping you ensure your argument is clear and that there are no gaps, vague terms, or unanswered questions for readers who weren’t involved in the research process.
Peer-reviewed articles are considered a highly credible source due to this stringent process they go through before publication.
In general, the peer review process follows the following steps:
- First, the author submits the manuscript to the editor.
- Reject the manuscript and send it back to author, or
- Send it onward to the selected peer reviewer(s)
- Next, the peer review process occurs. The reviewer provides feedback, addressing any major or minor issues with the manuscript, and gives their advice regarding what edits should be made.
- Lastly, the edited manuscript is sent back to the author. They input the edits, and resubmit it to the editor for publication.
Peer review is a process of evaluating submissions to an academic journal. Utilising rigorous criteria, a panel of reviewers in the same subject area decide whether to accept each submission for publication.
For this reason, academic journals are often considered among the most credible sources you can use in a research project – provided that the journal itself is trustworthy and well regarded.
Anonymity means you don’t know who the participants are, while confidentiality means you know who they are but remove identifying information from your research report. Both are important ethical considerations .
You can only guarantee anonymity by not collecting any personally identifying information – for example, names, phone numbers, email addresses, IP addresses, physical characteristics, photos, or videos.
You can keep data confidential by using aggregate information in your research report, so that you only refer to groups of participants rather than individuals.
Research misconduct means making up or falsifying data, manipulating data analyses, or misrepresenting results in research reports. It’s a form of academic fraud.
These actions are committed intentionally and can have serious consequences; research misconduct is not a simple mistake or a point of disagreement but a serious ethical failure.
Research ethics matter for scientific integrity, human rights and dignity, and collaboration between science and society. These principles make sure that participation in studies is voluntary, informed, and safe.
Ethical considerations in research are a set of principles that guide your research designs and practices. These principles include voluntary participation, informed consent, anonymity, confidentiality, potential for harm, and results communication.
Scientists and researchers must always adhere to a certain code of conduct when collecting data from others .
These considerations protect the rights of research participants, enhance research validity , and maintain scientific integrity.
A systematic review is secondary research because it uses existing research. You don’t collect new data yourself.
The two main types of social desirability bias are:
- Self-deceptive enhancement (self-deception): The tendency to see oneself in a favorable light without realizing it.
- Impression managemen t (other-deception): The tendency to inflate one’s abilities or achievement in order to make a good impression on other people.
Demand characteristics are aspects of experiments that may give away the research objective to participants. Social desirability bias occurs when participants automatically try to respond in ways that make them seem likeable in a study, even if it means misrepresenting how they truly feel.
Participants may use demand characteristics to infer social norms or experimenter expectancies and act in socially desirable ways, so you should try to control for demand characteristics wherever possible.
Response bias refers to conditions or factors that take place during the process of responding to surveys, affecting the responses. One type of response bias is social desirability bias .
When your population is large in size, geographically dispersed, or difficult to contact, it’s necessary to use a sampling method .
This allows you to gather information from a smaller part of the population, i.e. the sample, and make accurate statements by using statistical analysis. A few sampling methods include simple random sampling , convenience sampling , and snowball sampling .
Stratified and cluster sampling may look similar, but bear in mind that groups created in cluster sampling are heterogeneous , so the individual characteristics in the cluster vary. In contrast, groups created in stratified sampling are homogeneous , as units share characteristics.
Relatedly, in cluster sampling you randomly select entire groups and include all units of each group in your sample. However, in stratified sampling, you select some units of all groups and include them in your sample. In this way, both methods can ensure that your sample is representative of the target population .
A sampling frame is a list of every member in the entire population . It is important that the sampling frame is as complete as possible, so that your sample accurately reflects your population.
Convenience sampling and quota sampling are both non-probability sampling methods. They both use non-random criteria like availability, geographical proximity, or expert knowledge to recruit study participants.
However, in convenience sampling, you continue to sample units or cases until you reach the required sample size.
In quota sampling, you first need to divide your population of interest into subgroups (strata) and estimate their proportions (quota) in the population. Then you can start your data collection , using convenience sampling to recruit participants, until the proportions in each subgroup coincide with the estimated proportions in the population.
Random sampling or probability sampling is based on random selection. This means that each unit has an equal chance (i.e., equal probability) of being included in the sample.
On the other hand, convenience sampling involves stopping people at random, which means that not everyone has an equal chance of being selected depending on the place, time, or day you are collecting your data.
Stratified sampling and quota sampling both involve dividing the population into subgroups and selecting units from each subgroup. The purpose in both cases is to select a representative sample and/or to allow comparisons between subgroups.
The main difference is that in stratified sampling, you draw a random sample from each subgroup ( probability sampling ). In quota sampling you select a predetermined number or proportion of units, in a non-random manner ( non-probability sampling ).
Snowball sampling is best used in the following cases:
- If there is no sampling frame available (e.g., people with a rare disease)
- If the population of interest is hard to access or locate (e.g., people experiencing homelessness)
- If the research focuses on a sensitive topic (e.g., extra-marital affairs)
Snowball sampling relies on the use of referrals. Here, the researcher recruits one or more initial participants, who then recruit the next ones.
Participants share similar characteristics and/or know each other. Because of this, not every member of the population has an equal chance of being included in the sample, giving rise to sampling bias .
Snowball sampling is a non-probability sampling method , where there is not an equal chance for every member of the population to be included in the sample .
This means that you cannot use inferential statistics and make generalisations – often the goal of quantitative research . As such, a snowball sample is not representative of the target population, and is usually a better fit for qualitative research .
Snowball sampling is a non-probability sampling method . Unlike probability sampling (which involves some form of random selection ), the initial individuals selected to be studied are the ones who recruit new participants.
Because not every member of the target population has an equal chance of being recruited into the sample, selection in snowball sampling is non-random.
Reproducibility and replicability are related terms.
- Reproducing research entails reanalysing the existing data in the same manner.
- Replicating (or repeating ) the research entails reconducting the entire analysis, including the collection of new data .
- A successful reproduction shows that the data analyses were conducted in a fair and honest manner.
- A successful replication shows that the reliability of the results is high.
The reproducibility and replicability of a study can be ensured by writing a transparent, detailed method section and using clear, unambiguous language.
Convergent validity and discriminant validity are both subtypes of construct validity . Together, they help you evaluate whether a test measures the concept it was designed to measure.
- Convergent validity indicates whether a test that is designed to measure a particular construct correlates with other tests that assess the same or similar construct.
- Discriminant validity indicates whether two tests that should not be highly related to each other are indeed not related
You need to assess both in order to demonstrate construct validity. Neither one alone is sufficient for establishing construct validity.
Construct validity has convergent and discriminant subtypes. They assist determine if a test measures the intended notion.
Content validity shows you how accurately a test or other measurement method taps into the various aspects of the specific construct you are researching.
In other words, it helps you answer the question: “does the test measure all aspects of the construct I want to measure?” If it does, then the test has high content validity.
The higher the content validity, the more accurate the measurement of the construct.
If the test fails to include parts of the construct, or irrelevant parts are included, the validity of the instrument is threatened, which brings your results into question.
Construct validity refers to how well a test measures the concept (or construct) it was designed to measure. Assessing construct validity is especially important when you’re researching concepts that can’t be quantified and/or are intangible, like introversion. To ensure construct validity your test should be based on known indicators of introversion ( operationalisation ).
On the other hand, content validity assesses how well the test represents all aspects of the construct. If some aspects are missing or irrelevant parts are included, the test has low content validity.
Face validity and content validity are similar in that they both evaluate how suitable the content of a test is. The difference is that face validity is subjective, and assesses content at surface level.
When a test has strong face validity, anyone would agree that the test’s questions appear to measure what they are intended to measure.
For example, looking at a 4th grade math test consisting of problems in which students have to add and multiply, most people would agree that it has strong face validity (i.e., it looks like a math test).
On the other hand, content validity evaluates how well a test represents all the aspects of a topic. Assessing content validity is more systematic and relies on expert evaluation. of each question, analysing whether each one covers the aspects that the test was designed to cover.
A 4th grade math test would have high content validity if it covered all the skills taught in that grade. Experts(in this case, math teachers), would have to evaluate the content validity by comparing the test to the learning objectives.
- Discriminant validity indicates whether two tests that should not be highly related to each other are indeed not related. This type of validity is also called divergent validity .
Criterion validity and construct validity are both types of measurement validity . In other words, they both show you how accurately a method measures something.
While construct validity is the degree to which a test or other measurement method measures what it claims to measure, criterion validity is the degree to which a test can predictively (in the future) or concurrently (in the present) measure something.
Construct validity is often considered the overarching type of measurement validity . You need to have face validity , content validity , and criterion validity in order to achieve construct validity.
Attrition refers to participants leaving a study. It always happens to some extent – for example, in randomised control trials for medical research.
Differential attrition occurs when attrition or dropout rates differ systematically between the intervention and the control group . As a result, the characteristics of the participants who drop out differ from the characteristics of those who stay in the study. Because of this, study results may be biased .
Criterion validity evaluates how well a test measures the outcome it was designed to measure. An outcome can be, for example, the onset of a disease.
Criterion validity consists of two subtypes depending on the time at which the two measures (the criterion and your test) are obtained:
- Concurrent validity is a validation strategy where the the scores of a test and the criterion are obtained at the same time
- Predictive validity is a validation strategy where the criterion variables are measured after the scores of the test
Validity tells you how accurately a method measures what it was designed to measure. There are 4 main types of validity :
- Construct validity : Does the test measure the construct it was designed to measure?
- Face validity : Does the test appear to be suitable for its objectives ?
- Content validity : Does the test cover all relevant parts of the construct it aims to measure.
- Criterion validity : Do the results accurately measure the concrete outcome they are designed to measure?
Convergent validity shows how much a measure of one construct aligns with other measures of the same or related constructs .
On the other hand, concurrent validity is about how a measure matches up to some known criterion or gold standard, which can be another measure.
Although both types of validity are established by calculating the association or correlation between a test score and another variable , they represent distinct validation methods.
The purpose of theory-testing mode is to find evidence in order to disprove, refine, or support a theory. As such, generalisability is not the aim of theory-testing mode.
Due to this, the priority of researchers in theory-testing mode is to eliminate alternative causes for relationships between variables . In other words, they prioritise internal validity over external validity , including ecological validity .
Inclusion and exclusion criteria are typically presented and discussed in the methodology section of your thesis or dissertation .
Inclusion and exclusion criteria are predominantly used in non-probability sampling . In purposive sampling and snowball sampling , restrictions apply as to who can be included in the sample .
Scope of research is determined at the beginning of your research process , prior to the data collection stage. Sometimes called “scope of study,” your scope delineates what will and will not be covered in your project. It helps you focus your work and your time, ensuring that you’ll be able to achieve your goals and outcomes.
Defining a scope can be very useful in any research project, from a research proposal to a thesis or dissertation . A scope is needed for all types of research: quantitative , qualitative , and mixed methods .
To define your scope of research, consider the following:
- Budget constraints or any specifics of grant funding
- Your proposed timeline and duration
- Specifics about your population of study, your proposed sample size , and the research methodology you’ll pursue
- Any inclusion and exclusion criteria
- Any anticipated control , extraneous , or confounding variables that could bias your research if not accounted for properly.
To make quantitative observations , you need to use instruments that are capable of measuring the quantity you want to observe. For example, you might use a ruler to measure the length of an object or a thermometer to measure its temperature.
Quantitative observations involve measuring or counting something and expressing the result in numerical form, while qualitative observations involve describing something in non-numerical terms, such as its appearance, texture, or color.
The Scribbr Reference Generator is developed using the open-source Citation Style Language (CSL) project and Frank Bennett’s citeproc-js . It’s the same technology used by dozens of other popular citation tools, including Mendeley and Zotero.
You can find all the citation styles and locales used in the Scribbr Reference Generator in our publicly accessible repository on Github .
To paraphrase effectively, don’t just take the original sentence and swap out some of the words for synonyms. Instead, try:
- Reformulating the sentence (e.g., change active to passive , or start from a different point)
- Combining information from multiple sentences into one
- Leaving out information from the original that isn’t relevant to your point
- Using synonyms where they don’t distort the meaning
The main point is to ensure you don’t just copy the structure of the original text, but instead reformulate the idea in your own words.
Plagiarism means using someone else’s words or ideas and passing them off as your own. Paraphrasing means putting someone else’s ideas into your own words.
So when does paraphrasing count as plagiarism?
- Paraphrasing is plagiarism if you don’t properly credit the original author.
- Paraphrasing is plagiarism if your text is too close to the original wording (even if you cite the source). If you directly copy a sentence or phrase, you should quote it instead.
- Paraphrasing is not plagiarism if you put the author’s ideas completely into your own words and properly reference the source .
To present information from other sources in academic writing , it’s best to paraphrase in most cases. This shows that you’ve understood the ideas you’re discussing and incorporates them into your text smoothly.
It’s appropriate to quote when:
- Changing the phrasing would distort the meaning of the original text
- You want to discuss the author’s language choices (e.g., in literary analysis )
- You’re presenting a precise definition
- You’re looking in depth at a specific claim
A quote is an exact copy of someone else’s words, usually enclosed in quotation marks and credited to the original author or speaker.
Every time you quote a source , you must include a correctly formatted in-text citation . This looks slightly different depending on the citation style .
For example, a direct quote in APA is cited like this: ‘This is a quote’ (Streefkerk, 2020, p. 5).
Every in-text citation should also correspond to a full reference at the end of your paper.
In scientific subjects, the information itself is more important than how it was expressed, so quoting should generally be kept to a minimum. In the arts and humanities, however, well-chosen quotes are often essential to a good paper.
In social sciences, it varies. If your research is mainly quantitative , you won’t include many quotes, but if it’s more qualitative , you may need to quote from the data you collected .
As a general guideline, quotes should take up no more than 5–10% of your paper. If in doubt, check with your instructor or supervisor how much quoting is appropriate in your field.
If you’re quoting from a text that paraphrases or summarises other sources and cites them in parentheses , APA recommends retaining the citations as part of the quote:
- Smith states that ‘the literature on this topic (Jones, 2015; Sill, 2019; Paulson, 2020) shows no clear consensus’ (Smith, 2019, p. 4).
Footnote or endnote numbers that appear within quoted text should be omitted.
If you want to cite an indirect source (one you’ve only seen quoted in another source), either locate the original source or use the phrase ‘as cited in’ in your citation.
A block quote is a long quote formatted as a separate ‘block’ of text. Instead of using quotation marks , you place the quote on a new line, and indent the entire quote to mark it apart from your own words.
APA uses block quotes for quotes that are 40 words or longer.
A credible source should pass the CRAAP test and follow these guidelines:
- The information should be up to date and current.
- The author and publication should be a trusted authority on the subject you are researching.
- The sources the author cited should be easy to find, clear, and unbiased.
- For a web source, the URL and layout should signify that it is trustworthy.
Common examples of primary sources include interview transcripts , photographs, novels, paintings, films, historical documents, and official statistics.
Anything you directly analyze or use as first-hand evidence can be a primary source, including qualitative or quantitative data that you collected yourself.
Common examples of secondary sources include academic books, journal articles , reviews, essays , and textbooks.
Anything that summarizes, evaluates or interprets primary sources can be a secondary source. If a source gives you an overview of background information or presents another researcher’s ideas on your topic, it is probably a secondary source.
To determine if a source is primary or secondary, ask yourself:
- Was the source created by someone directly involved in the events you’re studying (primary), or by another researcher (secondary)?
- Does the source provide original information (primary), or does it summarize information from other sources (secondary)?
- Are you directly analyzing the source itself (primary), or only using it for background information (secondary)?
Some types of sources are nearly always primary: works of art and literature, raw statistical data, official documents and records, and personal communications (e.g. letters, interviews ). If you use one of these in your research, it is probably a primary source.
Primary sources are often considered the most credible in terms of providing evidence for your argument, as they give you direct evidence of what you are researching. However, it’s up to you to ensure the information they provide is reliable and accurate.
Always make sure to properly cite your sources to avoid plagiarism .
A fictional movie is usually a primary source. A documentary can be either primary or secondary depending on the context.
If you are directly analysing some aspect of the movie itself – for example, the cinematography, narrative techniques, or social context – the movie is a primary source.
If you use the movie for background information or analysis about your topic – for example, to learn about a historical event or a scientific discovery – the movie is a secondary source.
Whether it’s primary or secondary, always properly cite the movie in the citation style you are using. Learn how to create an MLA movie citation or an APA movie citation .
Articles in newspapers and magazines can be primary or secondary depending on the focus of your research.
In historical studies, old articles are used as primary sources that give direct evidence about the time period. In social and communication studies, articles are used as primary sources to analyse language and social relations (for example, by conducting content analysis or discourse analysis ).
If you are not analysing the article itself, but only using it for background information or facts about your topic, then the article is a secondary source.
In academic writing , there are three main situations where quoting is the best choice:
- To analyse the author’s language (e.g., in a literary analysis essay )
- To give evidence from primary sources
- To accurately present a precise definition or argument
Don’t overuse quotes; your own voice should be dominant. If you just want to provide information from a source, it’s usually better to paraphrase or summarise .
Your list of tables and figures should go directly after your table of contents in your thesis or dissertation.
Lists of figures and tables are often not required, and they aren’t particularly common. They specifically aren’t required for APA Style, though you should be careful to follow their other guidelines for figures and tables .
If you have many figures and tables in your thesis or dissertation, include one may help you stay organised. Your educational institution may require them, so be sure to check their guidelines.
Copyright information can usually be found wherever the table or figure was published. For example, for a diagram in a journal article , look on the journal’s website or the database where you found the article. Images found on sites like Flickr are listed with clear copyright information.
If you find that permission is required to reproduce the material, be sure to contact the author or publisher and ask for it.
A list of figures and tables compiles all of the figures and tables that you used in your thesis or dissertation and displays them with the page number where they can be found.
APA doesn’t require you to include a list of tables or a list of figures . However, it is advisable to do so if your text is long enough to feature a table of contents and it includes a lot of tables and/or figures .
A list of tables and list of figures appear (in that order) after your table of contents, and are presented in a similar way.
A glossary is a collection of words pertaining to a specific topic. In your thesis or dissertation, it’s a list of all terms you used that may not immediately be obvious to your reader. Your glossary only needs to include terms that your reader may not be familiar with, and is intended to enhance their understanding of your work.
Definitional terms often fall into the category of common knowledge , meaning that they don’t necessarily have to be cited. This guidance can apply to your thesis or dissertation glossary as well.
However, if you’d prefer to cite your sources , you can follow guidance for citing dictionary entries in MLA or APA style for your glossary.
A glossary is a collection of words pertaining to a specific topic. In your thesis or dissertation, it’s a list of all terms you used that may not immediately be obvious to your reader. In contrast, an index is a list of the contents of your work organised by page number.
Glossaries are not mandatory, but if you use a lot of technical or field-specific terms, it may improve readability to add one to your thesis or dissertation. Your educational institution may also require them, so be sure to check their specific guidelines.
A glossary is a collection of words pertaining to a specific topic. In your thesis or dissertation, it’s a list of all terms you used that may not immediately be obvious to your reader. In contrast, dictionaries are more general collections of words.
The title page of your thesis or dissertation should include your name, department, institution, degree program, and submission date.
The title page of your thesis or dissertation goes first, before all other content or lists that you may choose to include.
Usually, no title page is needed in an MLA paper . A header is generally included at the top of the first page instead. The exceptions are when:
- Your instructor requires one, or
- Your paper is a group project
In those cases, you should use a title page instead of a header, listing the same information but on a separate page.
When you mention different chapters within your text, it’s considered best to use Roman numerals for most citation styles. However, the most important thing here is to remain consistent whenever using numbers in your dissertation .
A thesis or dissertation outline is one of the most critical first steps in your writing process. It helps you to lay out and organise your ideas and can provide you with a roadmap for deciding what kind of research you’d like to undertake.
Generally, an outline contains information on the different sections included in your thesis or dissertation, such as:
- Your anticipated title
- Your abstract
- Your chapters (sometimes subdivided into further topics like literature review, research methods, avenues for future research, etc.)
While a theoretical framework describes the theoretical underpinnings of your work based on existing research, a conceptual framework allows you to draw your own conclusions, mapping out the variables you may use in your study and the interplay between them.
A literature review and a theoretical framework are not the same thing and cannot be used interchangeably. While a theoretical framework describes the theoretical underpinnings of your work, a literature review critically evaluates existing research relating to your topic. You’ll likely need both in your dissertation .
A theoretical framework can sometimes be integrated into a literature review chapter , but it can also be included as its own chapter or section in your dissertation . As a rule of thumb, if your research involves dealing with a lot of complex theories, it’s a good idea to include a separate theoretical framework chapter.
An abstract is a concise summary of an academic text (such as a journal article or dissertation ). It serves two main purposes:
- To help potential readers determine the relevance of your paper for their own research.
- To communicate your key findings to those who don’t have time to read the whole paper.
Abstracts are often indexed along with keywords on academic databases, so they make your work more easily findable. Since the abstract is the first thing any reader sees, it’s important that it clearly and accurately summarises the contents of your paper.
The abstract is the very last thing you write. You should only write it after your research is complete, so that you can accurately summarize the entirety of your thesis or paper.
Avoid citing sources in your abstract . There are two reasons for this:
- The abstract should focus on your original research, not on the work of others.
- The abstract should be self-contained and fully understandable without reference to other sources.
There are some circumstances where you might need to mention other sources in an abstract: for example, if your research responds directly to another study or focuses on the work of a single theorist. In general, though, don’t include citations unless absolutely necessary.
The abstract appears on its own page, after the title page and acknowledgements but before the table of contents .
Results are usually written in the past tense , because they are describing the outcome of completed actions.
The results chapter or section simply and objectively reports what you found, without speculating on why you found these results. The discussion interprets the meaning of the results, puts them in context, and explains why they matter.
In qualitative research , results and discussion are sometimes combined. But in quantitative research , it’s considered important to separate the objective results from your interpretation of them.
Formulating a main research question can be a difficult task. Overall, your question should contribute to solving the problem that you have defined in your problem statement .
However, it should also fulfill criteria in three main areas:
- Researchability
- Feasibility and specificity
- Relevance and originality
The best way to remember the difference between a research plan and a research proposal is that they have fundamentally different audiences. A research plan helps you, the researcher, organize your thoughts. On the other hand, a dissertation proposal or research proposal aims to convince others (e.g., a supervisor, a funding body, or a dissertation committee) that your research topic is relevant and worthy of being conducted.
A noun is a word that represents a person, thing, concept, or place (e.g., ‘John’, ‘house’, ‘affinity’, ‘river’). Most sentences contain at least one noun or pronoun .
Nouns are often, but not always, preceded by an article (‘the’, ‘a’, or ‘an’) and/or another determiner such as an adjective.
There are many ways to categorize nouns into various types, and the same noun can fall into multiple categories or even change types depending on context.
Some of the main types of nouns are:
- Common nouns and proper nouns
- Countable and uncountable nouns
- Concrete and abstract nouns
- Collective nouns
- Possessive nouns
- Attributive nouns
- Appositive nouns
- Generic nouns
Pronouns are words like ‘I’, ‘she’, and ‘they’ that are used in a similar way to nouns . They stand in for a noun that has already been mentioned or refer to yourself and other people.
Pronouns can function just like nouns as the head of a noun phrase and as the subject or object of a verb. However, pronouns change their forms (e.g., from ‘I’ to ‘me’) depending on the grammatical context they’re used in, whereas nouns usually don’t.
Common nouns are words for types of things, people, and places, such as ‘dog’, ‘professor’, and ‘city’. They are not capitalised and are typically used in combination with articles and other determiners.
Proper nouns are words for specific things, people, and places, such as ‘Max’, ‘Dr Prakash’, and ‘London’. They are always capitalised and usually aren’t combined with articles and other determiners.
A proper adjective is an adjective that was derived from a proper noun and is therefore capitalised .
Proper adjectives include words for nationalities, languages, and ethnicities (e.g., ‘Japanese’, ‘Inuit’, ‘French’) and words derived from people’s names (e.g., ‘Bayesian’, ‘Orwellian’).
The names of seasons (e.g., ‘spring’) are treated as common nouns in English and therefore not capitalised . People often assume they are proper nouns, but this is an error.
The names of days and months, however, are capitalised since they’re treated as proper nouns in English (e.g., ‘Wednesday’, ‘January’).
No, as a general rule, academic concepts, disciplines, theories, models, etc. are treated as common nouns , not proper nouns , and therefore not capitalised . For example, ‘five-factor model of personality’ or ‘analytic philosophy’.
However, proper nouns that appear within the name of an academic concept (such as the name of the inventor) are capitalised as usual. For example, ‘Darwin’s theory of evolution’ or ‘ Student’s t table ‘.
Collective nouns are most commonly treated as singular (e.g., ‘the herd is grazing’), but usage differs between US and UK English :
- In US English, it’s standard to treat all collective nouns as singular, even when they are plural in appearance (e.g., ‘The Rolling Stones is …’). Using the plural form is usually seen as incorrect.
- In UK English, collective nouns can be treated as singular or plural depending on context. It’s quite common to use the plural form, especially when the noun looks plural (e.g., ‘The Rolling Stones are …’).
The plural of “crisis” is “crises”. It’s a loanword from Latin and retains its original Latin plural noun form (similar to “analyses” and “bases”). It’s wrong to write “crisises”.
For example, you might write “Several crises destabilized the regime.”
Normally, the plural of “fish” is the same as the singular: “fish”. It’s one of a group of irregular plural nouns in English that are identical to the corresponding singular nouns (e.g., “moose”, “sheep”). For example, you might write “The fish scatter as the shark approaches.”
If you’re referring to several species of fish, though, the regular plural “fishes” is often used instead. For example, “The aquarium contains many different fishes , including trout and carp.”
The correct plural of “octopus” is “octopuses”.
People often write “octopi” instead because they assume that the plural noun is formed in the same way as Latin loanwords such as “fungus/fungi”. But “octopus” actually comes from Greek, where its original plural is “octopodes”. In English, it instead has the regular plural form “octopuses”.
For example, you might write “There are four octopuses in the aquarium.”
The plural of “moose” is the same as the singular: “moose”. It’s one of a group of plural nouns in English that are identical to the corresponding singular nouns. So it’s wrong to write “mooses”.
For example, you might write “There are several moose in the forest.”
Bias in research affects the validity and reliability of your findings, leading to false conclusions and a misinterpretation of the truth. This can have serious implications in areas like medical research where, for example, a new form of treatment may be evaluated.
Observer bias occurs when the researcher’s assumptions, views, or preconceptions influence what they see and record in a study, while actor–observer bias refers to situations where respondents attribute internal factors (e.g., bad character) to justify other’s behaviour and external factors (difficult circumstances) to justify the same behaviour in themselves.
Response bias is a general term used to describe a number of different conditions or factors that cue respondents to provide inaccurate or false answers during surveys or interviews . These factors range from the interviewer’s perceived social position or appearance to the the phrasing of questions in surveys.
Nonresponse bias occurs when the people who complete a survey are different from those who did not, in ways that are relevant to the research topic. Nonresponse can happen either because people are not willing or not able to participate.
In research, demand characteristics are cues that might indicate the aim of a study to participants. These cues can lead to participants changing their behaviors or responses based on what they think the research is about.
Demand characteristics are common problems in psychology experiments and other social science studies because they can bias your research findings.
Demand characteristics are a type of extraneous variable that can affect the outcomes of the study. They can invalidate studies by providing an alternative explanation for the results.
These cues may nudge participants to consciously or unconsciously change their responses, and they pose a threat to both internal and external validity . You can’t be sure that your independent variable manipulation worked, or that your findings can be applied to other people or settings.
You can control demand characteristics by taking a few precautions in your research design and materials.
Use these measures:
- Deception: Hide the purpose of the study from participants
- Between-groups design : Give each participant only one independent variable treatment
- Double-blind design : Conceal the assignment of groups from participants and yourself
- Implicit measures: Use indirect or hidden measurements for your variables
Some attrition is normal and to be expected in research. However, the type of attrition is important because systematic research bias can distort your findings. Attrition bias can lead to inaccurate results because it affects internal and/or external validity .
To avoid attrition bias , applying some of these measures can help you reduce participant dropout (attrition) by making it easy and appealing for participants to stay.
- Provide compensation (e.g., cash or gift cards) for attending every session
- Minimise the number of follow-ups as much as possible
- Make all follow-ups brief, flexible, and convenient for participants
- Send participants routine reminders to schedule follow-ups
- Recruit more participants than you need for your sample (oversample)
- Maintain detailed contact information so you can get in touch with participants even if they move
If you have a small amount of attrition bias , you can use a few statistical methods to try to make up for this research bias .
Multiple imputation involves using simulations to replace the missing data with likely values. Alternatively, you can use sample weighting to make up for the uneven balance of participants in your sample.
Placebos are used in medical research for new medication or therapies, called clinical trials. In these trials some people are given a placebo, while others are given the new medication being tested.
The purpose is to determine how effective the new medication is: if it benefits people beyond a predefined threshold as compared to the placebo, it’s considered effective.
Although there is no definite answer to what causes the placebo effect , researchers propose a number of explanations such as the power of suggestion, doctor-patient interaction, classical conditioning, etc.
Belief bias and confirmation bias are both types of cognitive bias that impact our judgment and decision-making.
Confirmation bias relates to how we perceive and judge evidence. We tend to seek out and prefer information that supports our preexisting beliefs, ignoring any information that contradicts those beliefs.
Belief bias describes the tendency to judge an argument based on how plausible the conclusion seems to us, rather than how much evidence is provided to support it during the course of the argument.
Positivity bias is phenomenon that occurs when a person judges individual members of a group positively, even when they have negative impressions or judgments of the group as a whole. Positivity bias is closely related to optimism bias , or the e xpectation that things will work out well, even if rationality suggests that problems are inevitable in life.
Perception bias is a problem because it prevents us from seeing situations or people objectively. Rather, our expectations, beliefs, or emotions interfere with how we interpret reality. This, in turn, can cause us to misjudge ourselves or others. For example, our prejudices can interfere with whether we perceive people’s faces as friendly or unfriendly.
There are many ways to categorize adjectives into various types. An adjective can fall into one or more of these categories depending on how it is used.
Some of the main types of adjectives are:
- Attributive adjectives
- Predicative adjectives
- Comparative adjectives
- Superlative adjectives
- Coordinate adjectives
- Appositive adjectives
- Compound adjectives
- Participial adjectives
- Proper adjectives
- Denominal adjectives
- Nominal adjectives
Cardinal numbers (e.g., one, two, three) can be placed before a noun to indicate quantity (e.g., one apple). While these are sometimes referred to as ‘numeral adjectives ‘, they are more accurately categorised as determiners or quantifiers.
Proper adjectives are adjectives formed from a proper noun (i.e., the name of a specific person, place, or thing) that are used to indicate origin. Like proper nouns, proper adjectives are always capitalised (e.g., Newtonian, Marxian, African).
The cost of proofreading depends on the type and length of text, the turnaround time, and the level of services required. Most proofreading companies charge per word or page, while freelancers sometimes charge an hourly rate.
For proofreading alone, which involves only basic corrections of typos and formatting mistakes, you might pay as little as £0.01 per word, but in many cases, your text will also require some level of editing , which costs slightly more.
It’s often possible to purchase combined proofreading and editing services and calculate the price in advance based on your requirements.
Then and than are two commonly confused words . In the context of ‘better than’, you use ‘than’ with an ‘a’.
- Julie is better than Jesse.
- I’d rather spend my time with you than with him.
- I understand Eoghan’s point of view better than Claudia’s.
Use to and used to are commonly confused words . In the case of ‘used to do’, the latter (with ‘d’) is correct, since you’re describing an action or state in the past.
- I used to do laundry once a week.
- They used to do each other’s hair.
- We used to do the dishes every day .
There are numerous synonyms and near synonyms for the various meanings of “ favour ”:
| Advocate | Adoration |
| Approve of | Appreciation |
| Endorse | Praise |
| Support | Respect |
There are numerous synonyms and near synonyms for the two meanings of “ favoured ”:
| Advocated | Adored |
| Approved of | Appreciated |
| Endorsed | Praised |
| Supported | Preferred |
No one (two words) is an indefinite pronoun meaning ‘nobody’. People sometimes mistakenly write ‘noone’, but this is incorrect and should be avoided. ‘No-one’, with a hyphen, is also acceptable in UK English .
Nobody and no one are both indefinite pronouns meaning ‘no person’. They can be used interchangeably (e.g., ‘nobody is home’ means the same as ‘no one is home’).
Some synonyms and near synonyms of every time include:
- Without exception
‘Everytime’ is sometimes used to mean ‘each time’ or ‘whenever’. However, this is incorrect and should be avoided. The correct phrase is every time (two words).
Yes, the conjunction because is a compound word , but one with a long history. It originates in Middle English from the preposition “bi” (“by”) and the noun “cause”. Over time, the open compound “bi cause” became the closed compound “because”, which we use today.
Though it’s spelled this way now, the verb “be” is not one of the words that makes up “because”.
Yes, today is a compound word , but a very old one. It wasn’t originally formed from the preposition “to” and the noun “day”; rather, it originates from their Old English equivalents, “tō” and “dæġe”.
In the past, it was sometimes written as a hyphenated compound: “to-day”. But the hyphen is no longer included; it’s always “today” now (“to day” is also wrong).
IEEE citation format is defined by the Institute of Electrical and Electronics Engineers and used in their publications.
It’s also a widely used citation style for students in technical fields like electrical and electronic engineering, computer science, telecommunications, and computer engineering.
An IEEE in-text citation consists of a number in brackets at the relevant point in the text, which points the reader to the right entry in the numbered reference list at the end of the paper. For example, ‘Smith [1] states that …’
A location marker such as a page number is also included within the brackets when needed: ‘Smith [1, p. 13] argues …’
The IEEE reference page consists of a list of references numbered in the order they were cited in the text. The title ‘References’ appears in bold at the top, either left-aligned or centered.
The numbers appear in square brackets on the left-hand side of the page. The reference entries are indented consistently to separate them from the numbers. Entries are single-spaced, with a normal paragraph break between them.
If you cite the same source more than once in your writing, use the same number for all of the IEEE in-text citations for that source, and only include it on the IEEE reference page once. The source is numbered based on the first time you cite it.
For example, the fourth source you cite in your paper is numbered [4]. If you cite it again later, you still cite it as [4]. You can cite different parts of the source each time by adding page numbers [4, p. 15].
A verb is a word that indicates a physical action (e.g., ‘drive’), a mental action (e.g., ‘think’) or a state of being (e.g., ‘exist’). Every sentence contains a verb.
Verbs are almost always used along with a noun or pronoun to describe what the noun or pronoun is doing.
There are many ways to categorize verbs into various types. A verb can fall into one or more of these categories depending on how it is used.
Some of the main types of verbs are:
- Regular verbs
- Irregular verbs
- Transitive verbs
- Intransitive verbs
- Dynamic verbs
- Stative verbs
- Linking verbs
- Auxiliary verbs
- Modal verbs
- Phrasal verbs
Regular verbs are verbs whose simple past and past participle are formed by adding the suffix ‘-ed’ (e.g., ‘walked’).
Irregular verbs are verbs that form their simple past and past participles in some way other than by adding the suffix ‘-ed’ (e.g., ‘sat’).
The indefinite articles a and an are used to refer to a general or unspecified version of a noun (e.g., a house). Which indefinite article you use depends on the pronunciation of the word that follows it.
- A is used for words that begin with a consonant sound (e.g., a bear).
- An is used for words that begin with a vowel sound (e.g., an eagle).
Indefinite articles can only be used with singular countable nouns . Like definite articles, they are a type of determiner .
Editing and proofreading are different steps in the process of revising a text.
Editing comes first, and can involve major changes to content, structure and language. The first stages of editing are often done by authors themselves, while a professional editor makes the final improvements to grammar and style (for example, by improving sentence structure and word choice ).
Proofreading is the final stage of checking a text before it is published or shared. It focuses on correcting minor errors and inconsistencies (for example, in punctuation and capitalization ). Proofreaders often also check for formatting issues, especially in print publishing.
Whether you’re publishing a blog, submitting a research paper , or even just writing an important email, there are a few techniques you can use to make sure it’s error-free:
- Take a break : Set your work aside for at least a few hours so that you can look at it with fresh eyes.
- Proofread a printout : Staring at a screen for too long can cause fatigue – sit down with a pen and paper to check the final version.
- Use digital shortcuts : Take note of any recurring mistakes (for example, misspelling a particular word, switching between US and UK English , or inconsistently capitalizing a term), and use Find and Replace to fix it throughout the document.
If you want to be confident that an important text is error-free, it might be worth choosing a professional proofreading service instead.
There are many different routes to becoming a professional proofreader or editor. The necessary qualifications depend on the field – to be an academic or scientific proofreader, for example, you will need at least a university degree in a relevant subject.
For most proofreading jobs, experience and demonstrated skills are more important than specific qualifications. Often your skills will be tested as part of the application process.
To learn practical proofreading skills, you can choose to take a course with a professional organisation such as the Society for Editors and Proofreaders . Alternatively, you can apply to companies that offer specialised on-the-job training programmes, such as the Scribbr Academy .
Though they’re pronounced the same, there’s a big difference in meaning between its and it’s .
- ‘The cat ate its food’.
- ‘It’s almost Christmas’.
Its and it’s are often confused, but its (without apostrophe) is the possessive form of ‘it’ (e.g., its tail, its argument, its wing). You use ‘its’ instead of ‘his’ and ‘her’ for neuter, inanimate nouns.
Then and than are two commonly confused words with different meanings and grammatical roles.
- Then (pronounced with a short ‘e’ sound) refers to time. It’s often an adverb , but it can also be used as a noun meaning ‘that time’ and as an adjective referring to a previous status.
- Than (pronounced with a short ‘a’ sound) is used for comparisons. Grammatically, it usually functions as a conjunction , but sometimes it’s a preposition .
| Examples: Then in a sentence | Examples: Than in a sentence |
|---|---|
| Mix the dry ingredients first, and add the wet ingredients. | Max is a better saxophonist you. |
| I was working as a teacher . | I usually like coaching a team more I like playing soccer myself. |
Use to and used to are commonly confused words . In the case of ‘used to be’, the latter (with ‘d’) is correct, since you’re describing an action or state in the past.
- I used to be the new coworker.
- There used to be 4 cookies left.
- We used to walk to school every day .
A grammar checker is a tool designed to automatically check your text for spelling errors, grammatical issues, punctuation mistakes , and problems with sentence structure . You can check out our analysis of the best free grammar checkers to learn more.
A paraphrasing tool edits your text more actively, changing things whether they were grammatically incorrect or not. It can paraphrase your sentences to make them more concise and readable or for other purposes. You can check out our analysis of the best free paraphrasing tools to learn more.
Some tools available online combine both functions. Others, such as QuillBot , have separate grammar checker and paraphrasing tools. Be aware of what exactly the tool you’re using does to avoid introducing unwanted changes.
Good grammar is the key to expressing yourself clearly and fluently, especially in professional communication and academic writing . Word processors, browsers, and email programs typically have built-in grammar checkers, but they’re quite limited in the kinds of problems they can fix.
If you want to go beyond detecting basic spelling errors, there are many online grammar checkers with more advanced functionality. They can often detect issues with punctuation , word choice, and sentence structure that more basic tools would miss.
Not all of these tools are reliable, though. You can check out our research into the best free grammar checkers to explore the options.
Our research indicates that the best free grammar checker available online is the QuillBot grammar checker .
We tested 10 of the most popular checkers with the same sample text (containing 20 grammatical errors) and found that QuillBot easily outperformed the competition, scoring 18 out of 20, a drastic improvement over the second-place score of 13 out of 20.
It even appeared to outperform the premium versions of other grammar checkers, despite being entirely free.
A teacher’s aide is a person who assists in teaching classes but is not a qualified teacher. Aide is a noun meaning ‘assistant’, so it will always refer to a person.
‘Teacher’s aid’ is incorrect.
A visual aid is an instructional device (e.g., a photo, a chart) that appeals to vision to help you understand written or spoken information. Aid is often placed after an attributive noun or adjective (like ‘visual’) that describes the type of help provided.
‘Visual aide’ is incorrect.
A job aid is an instructional tool (e.g., a checklist, a cheat sheet) that helps you work efficiently. Aid is a noun meaning ‘assistance’. It’s often placed after an adjective or attributive noun (like ‘job’) that describes the specific type of help provided.
‘Job aide’ is incorrect.
There are numerous synonyms for the various meanings of truly :
| Candidly | Completely | Accurately |
| Honestly | Really | Correctly |
| Openly | Totally | Exactly |
| Truthfully | Precisely |
Yours truly is a phrase used at the end of a formal letter or email. It can also be used (typically in a humorous way) as a pronoun to refer to oneself (e.g., ‘The dinner was cooked by yours truly ‘). The latter usage should be avoided in formal writing.
It’s formed by combining the second-person possessive pronoun ‘yours’ with the adverb ‘ truly ‘.
A pathetic fallacy can be a short phrase or a whole sentence and is often used in novels and poetry. Pathetic fallacies serve multiple purposes, such as:
- Conveying the emotional state of the characters or the narrator
- Creating an atmosphere or set the mood of a scene
- Foreshadowing events to come
- Giving texture and vividness to a piece of writing
- Communicating emotion to the reader in a subtle way, by describing the external world.
- Bringing inanimate objects to life so that they seem more relatable.
AMA citation format is a citation style designed by the American Medical Association. It’s frequently used in the field of medicine.
You may be told to use AMA style for your student papers. You will also have to follow this style if you’re submitting a paper to a journal published by the AMA.
An AMA in-text citation consists of the number of the relevant reference on your AMA reference page , written in superscript 1 at the point in the text where the source is used.
It may also include the page number or range of the relevant material in the source (e.g., the part you quoted 2(p46) ). Multiple sources can be cited at one point, presented as a range or list (with no spaces 3,5–9 ).
An AMA reference usually includes the author’s last name and initials, the title of the source, information about the publisher or the publication it’s contained in, and the publication date. The specific details included, and the formatting, depend on the source type.
References in AMA style are presented in numerical order (numbered by the order in which they were first cited in the text) on your reference page. A source that’s cited repeatedly in the text still only appears once on the reference page.
An AMA in-text citation just consists of the number of the relevant entry on your AMA reference page , written in superscript at the point in the text where the source is referred to.
You don’t need to mention the author of the source in your sentence, but you can do so if you want. It’s not an official part of the citation, but it can be useful as part of a signal phrase introducing the source.
On your AMA reference page , author names are written with the last name first, followed by the initial(s) of their first name and middle name if mentioned.
There’s a space between the last name and the initials, but no space or punctuation between the initials themselves. The names of multiple authors are separated by commas , and the whole list ends in a period, e.g., ‘Andreessen F, Smith PW, Gonzalez E’.
The names of up to six authors should be listed for each source on your AMA reference page , separated by commas . For a source with seven or more authors, you should list the first three followed by ‘ et al’ : ‘Isidore, Gilbert, Gunvor, et al’.
In the text, mentioning author names is optional (as they aren’t an official part of AMA in-text citations ). If you do mention them, though, you should use the first author’s name followed by ‘et al’ when there are three or more : ‘Isidore et al argue that …’
Note that according to AMA’s rather minimalistic punctuation guidelines, there’s no period after ‘et al’ unless it appears at the end of a sentence. This is different from most other styles, where there is normally a period.
Yes, you should normally include an access date in an AMA website citation (or when citing any source with a URL). This is because webpages can change their content over time, so it’s useful for the reader to know when you accessed the page.
When a publication or update date is provided on the page, you should include it in addition to the access date. The access date appears second in this case, e.g., ‘Published June 19, 2021. Accessed August 29, 2022.’
Don’t include an access date when citing a source with a DOI (such as in an AMA journal article citation ).
Some variables have fixed levels. For example, gender and ethnicity are always nominal level data because they cannot be ranked.
However, for other variables, you can choose the level of measurement . For example, income is a variable that can be recorded on an ordinal or a ratio scale:
- At an ordinal level , you could create 5 income groupings and code the incomes that fall within them from 1–5.
- At a ratio level , you would record exact numbers for income.
If you have a choice, the ratio level is always preferable because you can analyse data in more ways. The higher the level of measurement, the more precise your data is.
The level at which you measure a variable determines how you can analyse your data.
Depending on the level of measurement , you can perform different descriptive statistics to get an overall summary of your data and inferential statistics to see if your results support or refute your hypothesis .
Levels of measurement tell you how precisely variables are recorded. There are 4 levels of measurement, which can be ranked from low to high:
- Nominal : the data can only be categorised.
- Ordinal : the data can be categorised and ranked.
- Interval : the data can be categorised and ranked, and evenly spaced.
- Ratio : the data can be categorised, ranked, evenly spaced and has a natural zero.
Statistical analysis is the main method for analyzing quantitative research data . It uses probabilities and models to test predictions about a population from sample data.
The null hypothesis is often abbreviated as H 0 . When the null hypothesis is written using mathematical symbols, it always includes an equality symbol (usually =, but sometimes ≥ or ≤).
The alternative hypothesis is often abbreviated as H a or H 1 . When the alternative hypothesis is written using mathematical symbols, it always includes an inequality symbol (usually ≠, but sometimes < or >).
As the degrees of freedom increase, Student’s t distribution becomes less leptokurtic , meaning that the probability of extreme values decreases. The distribution becomes more and more similar to a standard normal distribution .
When there are only one or two degrees of freedom , the chi-square distribution is shaped like a backwards ‘J’. When there are three or more degrees of freedom, the distribution is shaped like a right-skewed hump. As the degrees of freedom increase, the hump becomes less right-skewed and the peak of the hump moves to the right. The distribution becomes more and more similar to a normal distribution .
‘Looking forward in hearing from you’ is an incorrect version of the phrase looking forward to hearing from you . The phrasal verb ‘looking forward to’ always needs the preposition ‘to’, not ‘in’.
- I am looking forward in hearing from you.
- I am looking forward to hearing from you.
Some synonyms and near synonyms for the expression looking forward to hearing from you include:
- Eagerly awaiting your response
- Hoping to hear from you soon
- It would be great to hear back from you
- Thanks in advance for your reply
People sometimes mistakenly write ‘looking forward to hear from you’, but this is incorrect. The correct phrase is looking forward to hearing from you .
The phrasal verb ‘look forward to’ is always followed by a direct object, the thing you’re looking forward to. As the direct object has to be a noun phrase , it should be the gerund ‘hearing’, not the verb ‘hear’.
- I’m looking forward to hear from you soon.
- I’m looking forward to hearing from you soon.
Traditionally, the sign-off Yours sincerely is used in an email message or letter when you are writing to someone you have interacted with before, not a complete stranger.
Yours faithfully is used instead when you are writing to someone you have had no previous correspondence with, especially if you greeted them as ‘ Dear Sir or Madam ’.
Just checking in is a standard phrase used to start an email (or other message) that’s intended to ask someone for a response or follow-up action in a friendly, informal way. However, it’s a cliché opening that can come across as passive-aggressive, so we recommend avoiding it in favor of a more direct opening like “We previously discussed …”
In a more personal context, you might encounter “just checking in” as part of a longer phrase such as “I’m just checking in to see how you’re doing”. In this case, it’s not asking the other person to do anything but rather asking about their well-being (emotional or physical) in a friendly way.
“Earliest convenience” is part of the phrase at your earliest convenience , meaning “as soon as you can”.
It’s typically used to end an email in a formal context by asking the recipient to do something when it’s convenient for them to do so.
ASAP is an abbreviation of the phrase “as soon as possible”.
It’s typically used to indicate a sense of urgency in highly informal contexts (e.g., “Let me know ASAP if you need me to drive you to the airport”).
“ASAP” should be avoided in more formal correspondence. Instead, use an alternative like at your earliest convenience .
Some synonyms and near synonyms of the verb compose (meaning “to make up”) are:
People increasingly use “comprise” as a synonym of “compose.” However, this is normally still seen as a mistake, and we recommend avoiding it in your academic writing . “Comprise” traditionally means “to be made up of,” not “to make up.”
Some synonyms and near synonyms of the verb comprise are:
- Be composed of
- Be made up of
People increasingly use “comprise” interchangeably with “compose,” meaning that they consider words like “compose,” “constitute,” and “form” to be synonymous with “comprise.” However, this is still normally regarded as an error, and we advise against using these words interchangeably in academic writing .
A fallacy is a mistaken belief, particularly one based on unsound arguments or one that lacks the evidence to support it. Common types of fallacy that may compromise the quality of your research are:
- Correlation/causation fallacy: Claiming that two events that occur together have a cause-and-effect relationship even though this can’t be proven
- Ecological fallacy : Making inferences about the nature of individuals based on aggregate data for the group
- The sunk cost fallacy : Following through on a project or decision because we have already invested time, effort, or money into it, even if the current costs outweigh the benefits
- The base-rate fallacy : Ignoring base-rate or statistically significant information, such as sample size or the relative frequency of an event, in favor of less relevant information e.g., pertaining to a single case, or a small number of cases
- The planning fallacy : Underestimating the time needed to complete a future task, even when we know that similar tasks in the past have taken longer than planned
The planning fallacy refers to people’s tendency to underestimate the resources needed to complete a future task, despite knowing that previous tasks have also taken longer than planned.
For example, people generally tend to underestimate the cost and time needed for construction projects. The planning fallacy occurs due to people’s tendency to overestimate the chances that positive events, such as a shortened timeline, will happen to them. This phenomenon is called optimism bias or positivity bias.
Although both red herring fallacy and straw man fallacy are logical fallacies or reasoning errors, they denote different attempts to “win” an argument. More specifically:
- A red herring fallacy refers to an attempt to change the subject and divert attention from the original issue. In other words, a seemingly solid but ultimately irrelevant argument is introduced into the discussion, either on purpose or by mistake.
- A straw man argument involves the deliberate distortion of another person’s argument. By oversimplifying or exaggerating it, the other party creates an easy-to-refute argument and then attacks it.
The red herring fallacy is a problem because it is flawed reasoning. It is a distraction device that causes people to become sidetracked from the main issue and draw wrong conclusions.
Although a red herring may have some kernel of truth, it is used as a distraction to keep our eyes on a different matter. As a result, it can cause us to accept and spread misleading information.
The sunk cost fallacy and escalation of commitment (or commitment bias ) are two closely related terms. However, there is a slight difference between them:
- Escalation of commitment (aka commitment bias ) is the tendency to be consistent with what we have already done or said we will do in the past, especially if we did so in public. In other words, it is an attempt to save face and appear consistent.
- Sunk cost fallacy is the tendency to stick with a decision or a plan even when it’s failing. Because we have already invested valuable time, money, or energy, quitting feels like these resources were wasted.
In other words, escalating commitment is a manifestation of the sunk cost fallacy: an irrational escalation of commitment frequently occurs when people refuse to accept that the resources they’ve already invested cannot be recovered. Instead, they insist on more spending to justify the initial investment (and the incurred losses).
When you are faced with a straw man argument , the best way to respond is to draw attention to the fallacy and ask your discussion partner to show how your original statement and their distorted version are the same. Since these are different, your partner will either have to admit that their argument is invalid or try to justify it by using more flawed reasoning, which you can then attack.
The straw man argument is a problem because it occurs when we fail to take an opposing point of view seriously. Instead, we intentionally misrepresent our opponent’s ideas and avoid genuinely engaging with them. Due to this, resorting to straw man fallacy lowers the standard of constructive debate.
A straw man argument is a distorted (and weaker) version of another person’s argument that can easily be refuted (e.g., when a teacher proposes that the class spend more time on math exercises, a parent complains that the teacher doesn’t care about reading and writing).
This is a straw man argument because it misrepresents the teacher’s position, which didn’t mention anything about cutting down on reading and writing. The straw man argument is also known as the straw man fallacy .
A slippery slope argument is not always a fallacy.
- When someone claims adopting a certain policy or taking a certain action will automatically lead to a series of other policies or actions also being taken, this is a slippery slope argument.
- If they don’t show a causal connection between the advocated policy and the consequent policies, then they commit a slippery slope fallacy .
There are a number of ways you can deal with slippery slope arguments especially when you suspect these are fallacious:
- Slippery slope arguments take advantage of the gray area between an initial action or decision and the possible next steps that might lead to the undesirable outcome. You can point out these missing steps and ask your partner to indicate what evidence exists to support the claimed relationship between two or more events.
- Ask yourself if each link in the chain of events or action is valid. Every proposition has to be true for the overall argument to work, so even if one link is irrational or not supported by evidence, then the argument collapses.
- Sometimes people commit a slippery slope fallacy unintentionally. In these instances, use an example that demonstrates the problem with slippery slope arguments in general (e.g., by using statements to reach a conclusion that is not necessarily relevant to the initial statement). By attacking the concept of slippery slope arguments you can show that they are often fallacious.
People sometimes confuse cognitive bias and logical fallacies because they both relate to flawed thinking. However, they are not the same:
- Cognitive bias is the tendency to make decisions or take action in an illogical way because of our values, memory, socialization, and other personal attributes. In other words, it refers to a fixed pattern of thinking rooted in the way our brain works.
- Logical fallacies relate to how we make claims and construct our arguments in the moment. They are statements that sound convincing at first but can be disproven through logical reasoning.
In other words, cognitive bias refers to an ongoing predisposition, while logical fallacy refers to mistakes of reasoning that occur in the moment.
An appeal to ignorance (ignorance here meaning lack of evidence) is a type of informal logical fallacy .
It asserts that something must be true because it hasn’t been proven false—or that something must be false because it has not yet been proven true.
For example, “unicorns exist because there is no evidence that they don’t.” The appeal to ignorance is also called the burden of proof fallacy .
An ad hominem (Latin for “to the person”) is a type of informal logical fallacy . Instead of arguing against a person’s position, an ad hominem argument attacks the person’s character or actions in an effort to discredit them.
This rhetorical strategy is fallacious because a person’s character, motive, education, or other personal trait is logically irrelevant to whether their argument is true or false.
Name-calling is common in ad hominem fallacy (e.g., “environmental activists are ineffective because they’re all lazy tree-huggers”).
Ad hominem is a persuasive technique where someone tries to undermine the opponent’s argument by personally attacking them.
In this way, one can redirect the discussion away from the main topic and to the opponent’s personality without engaging with their viewpoint. When the opponent’s personality is irrelevant to the discussion, we call it an ad hominem fallacy .
Ad hominem tu quoque (‘you too”) is an attempt to rebut a claim by attacking its proponent on the grounds that they uphold a double standard or that they don’t practice what they preach. For example, someone is telling you that you should drive slowly otherwise you’ll get a speeding ticket one of these days, and you reply “but you used to get them all the time!”
Argumentum ad hominem means “argument to the person” in Latin and it is commonly referred to as ad hominem argument or personal attack. Ad hominem arguments are used in debates to refute an argument by attacking the character of the person making it, instead of the logic or premise of the argument itself.
The opposite of the hasty generalization fallacy is called slothful induction fallacy or appeal to coincidence .
It is the tendency to deny a conclusion even though there is sufficient evidence that supports it. Slothful induction occurs due to our natural tendency to dismiss events or facts that do not align with our personal biases and expectations. For example, a researcher may try to explain away unexpected results by claiming it is just a coincidence.
To avoid a hasty generalization fallacy we need to ensure that the conclusions drawn are well-supported by the appropriate evidence. More specifically:
- In statistics , if we want to draw inferences about an entire population, we need to make sure that the sample is random and representative of the population . We can achieve that by using a probability sampling method , like simple random sampling or stratified sampling .
- In academic writing , use precise language and measured phases. Try to avoid making absolute claims, cite specific instances and examples without applying the findings to a larger group.
- As readers, we need to ask ourselves “does the writer demonstrate sufficient knowledge of the situation or phenomenon that would allow them to make a generalization?”
The hasty generalization fallacy and the anecdotal evidence fallacy are similar in that they both result in conclusions drawn from insufficient evidence. However, there is a difference between the two:
- The hasty generalization fallacy involves genuinely considering an example or case (i.e., the evidence comes first and then an incorrect conclusion is drawn from this).
- The anecdotal evidence fallacy (also known as “cherry-picking” ) is knowing in advance what conclusion we want to support, and then selecting the story (or a few stories) that support it. By overemphasizing anecdotal evidence that fits well with the point we are trying to make, we overlook evidence that would undermine our argument.
Although many sources use circular reasoning fallacy and begging the question interchangeably, others point out that there is a subtle difference between the two:
- Begging the question fallacy occurs when you assume that an argument is true in order to justify a conclusion. If something begs the question, what you are actually asking is, “Is the premise of that argument actually true?” For example, the statement “Snakes make great pets. That’s why we should get a snake” begs the question “are snakes really great pets?”
- Circular reasoning fallacy on the other hand, occurs when the evidence used to support a claim is just a repetition of the claim itself. For example, “People have free will because they can choose what to do.”
In other words, we could say begging the question is a form of circular reasoning.
Circular reasoning fallacy uses circular reasoning to support an argument. More specifically, the evidence used to support a claim is just a repetition of the claim itself. For example: “The President of the United States is a good leader (claim), because they are the leader of this country (supporting evidence)”.
An example of a non sequitur is the following statement:
“Giving up nuclear weapons weakened the United States’ military. Giving up nuclear weapons also weakened China. For this reason, it is wrong to try to outlaw firearms in the United States today.”
Clearly there is a step missing in this line of reasoning and the conclusion does not follow from the premise, resulting in a non sequitur fallacy .
The difference between the post hoc fallacy and the non sequitur fallacy is that post hoc fallacy infers a causal connection between two events where none exists, whereas the non sequitur fallacy infers a conclusion that lacks a logical connection to the premise.
In other words, a post hoc fallacy occurs when there is a lack of a cause-and-effect relationship, while a non sequitur fallacy occurs when there is a lack of logical connection.
An example of post hoc fallacy is the following line of reasoning:
“Yesterday I had ice cream, and today I have a terrible stomachache. I’m sure the ice cream caused this.”
Although it is possible that the ice cream had something to do with the stomachache, there is no proof to justify the conclusion other than the order of events. Therefore, this line of reasoning is fallacious.
Post hoc fallacy and hasty generalisation fallacy are similar in that they both involve jumping to conclusions. However, there is a difference between the two:
- Post hoc fallacy is assuming a cause and effect relationship between two events, simply because one happened after the other.
- Hasty generalisation fallacy is drawing a general conclusion from a small sample or little evidence.
In other words, post hoc fallacy involves a leap to a causal claim; hasty generalisation fallacy involves a leap to a general proposition.
The fallacy of composition is similar to and can be confused with the hasty generalization fallacy . However, there is a difference between the two:
- The fallacy of composition involves drawing an inference about the characteristics of a whole or group based on the characteristics of its individual members.
- The hasty generalization fallacy involves drawing an inference about a population or class of things on the basis of few atypical instances or a small sample of that population or thing.
In other words, the fallacy of composition is using an unwarranted assumption that we can infer something about a whole based on the characteristics of its parts, while the hasty generalization fallacy is using insufficient evidence to draw a conclusion.
The opposite of the fallacy of composition is the fallacy of division . In the fallacy of division, the assumption is that a characteristic which applies to a whole or a group must necessarily apply to the parts or individual members. For example, “Australians travel a lot. Gary is Australian, so he must travel a lot.”
Base rate fallacy can be avoided by following these steps:
- Avoid making an important decision in haste. When we are under pressure, we are more likely to resort to cognitive shortcuts like the availability heuristic and the representativeness heuristic . Due to this, we are more likely to factor in only current and vivid information, and ignore the actual probability of something happening (i.e., base rate).
- Take a long-term view on the decision or question at hand. Look for relevant statistical data, which can reveal long-term trends and give you the full picture.
- Talk to experts like professionals. They are more aware of probabilities related to specific decisions.
Suppose there is a population consisting of 90% psychologists and 10% engineers. Given that you know someone enjoyed physics at school, you may conclude that they are an engineer rather than a psychologist, even though you know that this person comes from a population consisting of far more psychologists than engineers.
When we ignore the rate of occurrence of some trait in a population (the base-rate information) we commit base rate fallacy .
Cost-benefit fallacy is a common error that occurs when allocating sources in project management. It is the fallacy of assuming that cost-benefit estimates are more or less accurate, when in fact they are highly inaccurate and biased. This means that cost-benefit analyses can be useful, but only after the cost-benefit fallacy has been acknowledged and corrected for. Cost-benefit fallacy is a type of base rate fallacy .
In advertising, the fallacy of equivocation is often used to create a pun. For example, a billboard company might advertise their billboards using a line like: “Looking for a sign? This is it!” The word sign has a literal meaning as billboard and a figurative one as a sign from God, the universe, etc.
Equivocation is a fallacy because it is a form of argumentation that is both misleading and logically unsound. When the meaning of a word or phrase shifts in the course of an argument, it causes confusion and also implies that the conclusion (which may be true) does not follow from the premise.
The fallacy of equivocation is an informal logical fallacy, meaning that the error lies in the content of the argument instead of the structure.
Fallacies of relevance are a group of fallacies that occur in arguments when the premises are logically irrelevant to the conclusion. Although at first there seems to be a connection between the premise and the conclusion, in reality fallacies of relevance use unrelated forms of appeal.
For example, the genetic fallacy makes an appeal to the source or origin of the claim in an attempt to assert or refute something.
The ad hominem fallacy and the genetic fallacy are closely related in that they are both fallacies of relevance. In other words, they both involve arguments that use evidence or examples that are not logically related to the argument at hand. However, there is a difference between the two:
- In the ad hominem fallacy , the goal is to discredit the argument by discrediting the person currently making the argument.
- In the genetic fallacy , the goal is to discredit the argument by discrediting the history or origin (i.e., genesis) of an argument.
False dilemma fallacy is also known as false dichotomy, false binary, and “either-or” fallacy. It is the fallacy of presenting only two choices, outcomes, or sides to an argument as the only possibilities, when more are available.
The false dilemma fallacy works in two ways:
- By presenting only two options as if these were the only ones available
- By presenting two options as mutually exclusive (i.e., only one option can be selected or can be true at a time)
In both cases, by using the false dilemma fallacy, one conceals alternative choices and doesn’t allow others to consider the full range of options. This is usually achieved through an“either-or” construction and polarised, divisive language (“you are either a friend or an enemy”).
The best way to avoid a false dilemma fallacy is to pause and reflect on two points:
- Are the options presented truly the only ones available ? It could be that another option has been deliberately omitted.
- Are the options mentioned mutually exclusive ? Perhaps all of the available options can be selected (or be true) at the same time, which shows that they aren’t mutually exclusive. Proving this is called “escaping between the horns of the dilemma.”
Begging the question fallacy is an argument in which you assume what you are trying to prove. In other words, your position and the justification of that position are the same, only slightly rephrased.
For example: “All freshmen should attend college orientation, because all college students should go to such an orientation.”
The complex question fallacy and begging the question fallacy are similar in that they are both based on assumptions. However, there is a difference between them:
- A complex question fallacy occurs when someone asks a question that presupposes the answer to another question that has not been established or accepted by the other person. For example, asking someone “Have you stopped cheating on tests?”, unless it has previously been established that the person is indeed cheating on tests, is a fallacy.
- Begging the question fallacy occurs when we assume the very thing as a premise that we’re trying to prove in our conclusion. In other words, the conclusion is used to support the premises, and the premises prove the validity of the conclusion. For example: “God exists because the Bible says so, and the Bible is true because it is the word of God.”
In other words, begging the question is about drawing a conclusion based on an assumption, while a complex question involves asking a question that presupposes the answer to a prior question.
“ No true Scotsman ” arguments aren’t always fallacious. When there is a generally accepted definition of who or what constitutes a group, it’s reasonable to use statements in the form of “no true Scotsman”.
For example, the statement that “no true pacifist would volunteer for military service” is not fallacious, since a pacifist is, by definition, someone who opposes war or violence as a means of settling disputes.
No true Scotsman arguments are fallacious because instead of logically refuting the counterexample, they simply assert that it doesn’t count. In other words, the counterexample is rejected for psychological, but not logical, reasons.
The appeal to purity or no true Scotsman fallacy is an attempt to defend a generalisation about a group from a counterexample by shifting the definition of the group in the middle of the argument. In this way, one can exclude the counterexample as not being “true”, “genuine”, or “pure” enough to be considered as part of the group in question.
To identify an appeal to authority fallacy , you can ask yourself the following questions:
- Is the authority cited really a qualified expert in this particular area under discussion? For example, someone who has formal education or years of experience can be an expert.
- Do experts disagree on this particular subject? If that is the case, then for almost any claim supported by one expert there will be a counterclaim that is supported by another expert. If there is no consensus, an appeal to authority is fallacious.
- Is the authority in question biased? If you suspect that an expert’s prejudice and bias could have influenced their views, then the expert is not reliable and an argument citing this expert will be fallacious.To identify an appeal to authority fallacy, you ask yourself whether the authority cited is a qualified expert in the particular area under discussion.
Appeal to authority is a fallacy when those who use it do not provide any justification to support their argument. Instead they cite someone famous who agrees with their viewpoint, but is not qualified to make reliable claims on the subject.
Appeal to authority fallacy is often convincing because of the effect authority figures have on us. When someone cites a famous person, a well-known scientist, a politician, etc. people tend to be distracted and often fail to critically examine whether the authority figure is indeed an expert in the area under discussion.
The ad populum fallacy is common in politics. One example is the following viewpoint: “The majority of our countrymen think we should have military operations overseas; therefore, it’s the right thing to do.”
This line of reasoning is fallacious, because popular acceptance of a belief or position does not amount to a justification of that belief. In other words, following the prevailing opinion without examining the underlying reasons is irrational.
The ad populum fallacy plays on our innate desire to fit in (known as “bandwagon effect”). If many people believe something, our common sense tells us that it must be true and we tend to accept it. However, in logic, the popularity of a proposition cannot serve as evidence of its truthfulness.
Ad populum (or appeal to popularity) fallacy and appeal to authority fallacy are similar in that they both conflate the validity of a belief with its popular acceptance among a specific group. However there is a key difference between the two:
- An ad populum fallacy tries to persuade others by claiming that something is true or right because a lot of people think so.
- An appeal to authority fallacy tries to persuade by claiming a group of experts believe something is true or right, therefore it must be so.
To identify a false cause fallacy , you need to carefully analyse the argument:
- When someone claims that one event directly causes another, ask if there is sufficient evidence to establish a cause-and-effect relationship.
- Ask if the claim is based merely on the chronological order or co-occurrence of the two events.
- Consider alternative possible explanations (are there other factors at play that could influence the outcome?).
By carefully analysing the reasoning, considering alternative explanations, and examining the evidence provided, you can identify a false cause fallacy and discern whether a causal claim is valid or flawed.
False cause fallacy examples include:
- Believing that wearing your lucky jersey will help your team win
- Thinking that everytime you wash your car, it rains
- Claiming that playing video games causes violent behavior
In each of these examples, we falsely assume that one event causes another without any proof.
The planning fallacy and procrastination are not the same thing. Although they both relate to time and task management, they describe different challenges:
- The planning fallacy describes our inability to correctly estimate how long a future task will take, mainly due to optimism bias and a strong focus on the best-case scenario.
- Procrastination refers to postponing a task, usually by focusing on less urgent or more enjoyable activities. This is due to psychological reasons, like fear of failure.
In other words, the planning fallacy refers to inaccurate predictions about the time we need to finish a task, while procrastination is a deliberate delay due to psychological factors.
A real-life example of the planning fallacy is the construction of the Sydney Opera House in Australia. When construction began in the late 1950s, it was initially estimated that it would be completed in four years at a cost of around $7 million.
Because the government wanted the construction to start before political opposition would stop it and while public opinion was still favorable, a number of design issues had not been carefully studied in advance. Due to this, several problems appeared immediately after the project commenced.
The construction process eventually stretched over 14 years, with the Opera House being completed in 1973 at a cost of over $100 million, significantly exceeding the initial estimates.
An example of appeal to pity fallacy is the following appeal by a student to their professor:
“Professor, please consider raising my grade. I had a terrible semester: my car broke down, my laptop got stolen, and my cat got sick.”
While these circumstances may be unfortunate, they are not directly related to the student’s academic performance.
While both the appeal to pity fallacy and red herring fallacy can serve as a distraction from the original discussion topic, they are distinct fallacies. More specifically:
- Appeal to pity fallacy attempts to evoke feelings of sympathy, pity, or guilt in an audience, so that they accept the speaker’s conclusion as truthful.
- Red herring fallacy attempts to introduce an irrelevant piece of information that diverts the audience’s attention to a different topic.
Both fallacies can be used as a tool of deception. However, they operate differently and serve distinct purposes in arguments.
Argumentum ad misericordiam (Latin for “argument from pity or misery”) is another name for appeal to pity fallacy . It occurs when someone evokes sympathy or guilt in an attempt to gain support for their claim, without providing any logical reasons to support the claim itself. Appeal to pity is a deceptive tactic of argumentation, playing on people’s emotions to sway their opinion.
Yes, it’s quite common to start a sentence with a preposition, and there’s no reason not to do so.
For example, the sentence “ To many, she was a hero” is perfectly grammatical. It could also be rephrased as “She was a hero to many”, but there’s no particular reason to do so. Both versions are fine.
Some people argue that you shouldn’t end a sentence with a preposition , but that “rule” can also be ignored, since it’s not supported by serious language authorities.
Yes, it’s fine to end a sentence with a preposition . The “rule” against doing so is overwhelmingly rejected by modern style guides and language authorities and is based on the rules of Latin grammar, not English.
Trying to avoid ending a sentence with a preposition often results in very unnatural phrasings. For example, turning “He knows what he’s talking about ” into “He knows about what he’s talking” or “He knows that about which he’s talking” is definitely not an improvement.
No, ChatGPT is not a credible source of factual information and can’t be cited for this purpose in academic writing . While it tries to provide accurate answers, it often gets things wrong because its responses are based on patterns, not facts and data.
Specifically, the CRAAP test for evaluating sources includes five criteria: currency , relevance , authority , accuracy , and purpose . ChatGPT fails to meet at least three of them:
- Currency: The dataset that ChatGPT was trained on only extends to 2021, making it slightly outdated.
- Authority: It’s just a language model and is not considered a trustworthy source of factual information.
- Accuracy: It bases its responses on patterns rather than evidence and is unable to cite its sources .
So you shouldn’t cite ChatGPT as a trustworthy source for a factual claim. You might still cite ChatGPT for other reasons – for example, if you’re writing a paper about AI language models, ChatGPT responses are a relevant primary source .
ChatGPT is an AI language model that was trained on a large body of text from a variety of sources (e.g., Wikipedia, books, news articles, scientific journals). The dataset only went up to 2021, meaning that it lacks information on more recent events.
It’s also important to understand that ChatGPT doesn’t access a database of facts to answer your questions. Instead, its responses are based on patterns that it saw in the training data.
So ChatGPT is not always trustworthy . It can usually answer general knowledge questions accurately, but it can easily give misleading answers on more specialist topics.
Another consequence of this way of generating responses is that ChatGPT usually can’t cite its sources accurately. It doesn’t really know what source it’s basing any specific claim on. It’s best to check any information you get from it against a credible source .
No, it is not possible to cite your sources with ChatGPT . You can ask it to create citations, but it isn’t designed for this task and tends to make up sources that don’t exist or present information in the wrong format. ChatGPT also cannot add citations to direct quotes in your text.
Instead, use a tool designed for this purpose, like the Scribbr Citation Generator .
But you can use ChatGPT for assignments in other ways, to provide inspiration, feedback, and general writing advice.
GPT stands for “generative pre-trained transformer”, which is a type of large language model: a neural network trained on a very large amount of text to produce convincing, human-like language outputs. The Chat part of the name just means “chat”: ChatGPT is a chatbot that you interact with by typing in text.
The technology behind ChatGPT is GPT-3.5 (in the free version) or GPT-4 (in the premium version). These are the names for the specific versions of the GPT model. GPT-4 is currently the most advanced model that OpenAI has created. It’s also the model used in Bing’s chatbot feature.
ChatGPT was created by OpenAI, an AI research company. It started as a nonprofit company in 2015 but became for-profit in 2019. Its CEO is Sam Altman, who also co-founded the company. OpenAI released ChatGPT as a free “research preview” in November 2022. Currently, it’s still available for free, although a more advanced premium version is available if you pay for it.
OpenAI is also known for developing DALL-E, an AI image generator that runs on similar technology to ChatGPT.
ChatGPT is owned by OpenAI, the company that developed and released it. OpenAI is a company dedicated to AI research. It started as a nonprofit company in 2015 but transitioned to for-profit in 2019. Its current CEO is Sam Altman, who also co-founded the company.
In terms of who owns the content generated by ChatGPT, OpenAI states that it will not claim copyright on this content , and the terms of use state that “you can use Content for any purpose, including commercial purposes such as sale or publication”. This means that you effectively own any content you generate with ChatGPT and can use it for your own purposes.
Be cautious about how you use ChatGPT content in an academic context. University policies on AI writing are still developing, so even if you “own” the content, you’re often not allowed to submit it as your own work according to your university or to publish it in a journal.
ChatGPT is a chatbot based on a large language model (LLM). These models are trained on huge datasets consisting of hundreds of billions of words of text, based on which the model learns to effectively predict natural responses to the prompts you enter.
ChatGPT was also refined through a process called reinforcement learning from human feedback (RLHF), which involves “rewarding” the model for providing useful answers and discouraging inappropriate answers – encouraging it to make fewer mistakes.
Essentially, ChatGPT’s answers are based on predicting the most likely responses to your inputs based on its training data, with a reward system on top of this to incentivise it to give you the most helpful answers possible. It’s a bit like an incredibly advanced version of predictive text. This is also one of ChatGPT’s limitations : because its answers are based on probabilities, they’re not always trustworthy .
OpenAI may store ChatGPT conversations for the purposes of future training. Additionally, these conversations may be monitored by human AI trainers.
Users can choose not to have their chat history saved. Unsaved chats are not used to train future models and are permanently deleted from ChatGPT’s system after 30 days.
The official ChatGPT app is currently only available on iOS devices. If you don’t have an iOS device, only use the official OpenAI website to access the tool. This helps to eliminate the potential risk of downloading fraudulent or malicious software.
ChatGPT conversations are generally used to train future models and to resolve issues/bugs. These chats may be monitored by human AI trainers.
However, users can opt out of having their conversations used for training. In these instances, chats are monitored only for potential abuse.
Yes, using ChatGPT as a conversation partner is a great way to practice a language in an interactive way.
Try using a prompt like this one:
“Please be my Spanish conversation partner. Only speak to me in Spanish. Keep your answers short (maximum 50 words). Ask me questions. Let’s start the conversation with the following topic: [conversation topic].”
Yes, there are a variety of ways to use ChatGPT for language learning , including treating it as a conversation partner, asking it for translations, and using it to generate a curriculum or practice exercises.
AI detectors aim to identify the presence of AI-generated text (e.g., from ChatGPT ) in a piece of writing, but they can’t do so with complete accuracy. In our comparison of the best AI detectors , we found that the 10 tools we tested had an average accuracy of 60%. The best free tool had 68% accuracy, the best premium tool 84%.
Because of how AI detectors work , they can never guarantee 100% accuracy, and there is always at least a small risk of false positives (human text being marked as AI-generated). Therefore, these tools should not be relied upon to provide absolute proof that a text is or isn’t AI-generated. Rather, they can provide a good indication in combination with other evidence.
Tools called AI detectors are designed to label text as AI-generated or human. AI detectors work by looking for specific characteristics in the text, such as a low level of randomness in word choice and sentence length. These characteristics are typical of AI writing, allowing the detector to make a good guess at when text is AI-generated.
But these tools can’t guarantee 100% accuracy. Check out our comparison of the best AI detectors to learn more.
You can also manually watch for clues that a text is AI-generated – for example, a very different style from the writer’s usual voice or a generic, overly polite tone.
Our research into the best summary generators (aka summarisers or summarising tools) found that the best summariser available in 2023 is the one offered by QuillBot.
While many summarisers just pick out some sentences from the text, QuillBot generates original summaries that are creative, clear, accurate, and concise. It can summarise texts of up to 1,200 words for free, or up to 6,000 with a premium subscription.
Try the QuillBot summarizer for free
Deep learning requires a large dataset (e.g., images or text) to learn from. The more diverse and representative the data, the better the model will learn to recognise objects or make predictions. Only when the training data is sufficiently varied can the model make accurate predictions or recognise objects from new data.
Deep learning models can be biased in their predictions if the training data consist of biased information. For example, if a deep learning model used for screening job applicants has been trained with a dataset consisting primarily of white male applicants, it will consistently favour this specific population over others.
A good ChatGPT prompt (i.e., one that will get you the kinds of responses you want):
- Gives the tool a role to explain what type of answer you expect from it
- Is precisely formulated and gives enough context
- Is free from bias
- Has been tested and improved by experimenting with the tool
ChatGPT prompts are the textual inputs (e.g., questions, instructions) that you enter into ChatGPT to get responses.
ChatGPT predicts an appropriate response to the prompt you entered. In general, a more specific and carefully worded prompt will get you better responses.
Yes, ChatGPT is currently available for free. You have to sign up for a free account to use the tool, and you should be aware that your data may be collected to train future versions of the model.
To sign up and use the tool for free, go to this page and click “Sign up”. You can do so with your email or with a Google account.
A premium version of the tool called ChatGPT Plus is available as a monthly subscription. It currently costs £16 and gets you access to features like GPT-4 (a more advanced version of the language model). But it’s optional: you can use the tool completely free if you’re not interested in the extra features.
You can access ChatGPT by signing up for a free account:
- Follow this link to the ChatGPT website.
- Click on “Sign up” and fill in the necessary details (or use your Google account). It’s free to sign up and use the tool.
- Type a prompt into the chat box to get started!
A ChatGPT app is also available for iOS, and an Android app is planned for the future. The app works similarly to the website, and you log in with the same account for both.
According to OpenAI’s terms of use, users have the right to reproduce text generated by ChatGPT during conversations.
However, publishing ChatGPT outputs may have legal implications , such as copyright infringement.
Users should be aware of such issues and use ChatGPT outputs as a source of inspiration instead.
According to OpenAI’s terms of use, users have the right to use outputs from their own ChatGPT conversations for any purpose (including commercial publication).
However, users should be aware of the potential legal implications of publishing ChatGPT outputs. ChatGPT responses are not always unique: different users may receive the same response.
Furthermore, ChatGPT outputs may contain copyrighted material. Users may be liable if they reproduce such material.
ChatGPT can sometimes reproduce biases from its training data , since it draws on the text it has “seen” to create plausible responses to your prompts.
For example, users have shown that it sometimes makes sexist assumptions such as that a doctor mentioned in a prompt must be a man rather than a woman. Some have also pointed out political bias in terms of which political figures the tool is willing to write positively or negatively about and which requests it refuses.
The tool is unlikely to be consistently biased toward a particular perspective or against a particular group. Rather, its responses are based on its training data and on the way you phrase your ChatGPT prompts . It’s sensitive to phrasing, so asking it the same question in different ways will result in quite different answers.
Information extraction refers to the process of starting from unstructured sources (e.g., text documents written in ordinary English) and automatically extracting structured information (i.e., data in a clearly defined format that’s easily understood by computers). It’s an important concept in natural language processing (NLP) .
For example, you might think of using news articles full of celebrity gossip to automatically create a database of the relationships between the celebrities mentioned (e.g., married, dating, divorced, feuding). You would end up with data in a structured format, something like MarriageBetween(celebrity 1 ,celebrity 2 ,date) .
The challenge involves developing systems that can “understand” the text well enough to extract this kind of data from it.
Knowledge representation and reasoning (KRR) is the study of how to represent information about the world in a form that can be used by a computer system to solve and reason about complex problems. It is an important field of artificial intelligence (AI) research.
An example of a KRR application is a semantic network, a way of grouping words or concepts by how closely related they are and formally defining the relationships between them so that a machine can “understand” language in something like the way people do.
A related concept is information extraction , concerned with how to get structured information from unstructured sources.
Yes, you can use ChatGPT to summarise text . This can help you understand complex information more easily, summarise the central argument of your own paper, or clarify your research question.
You can also use Scribbr’s free text summariser , which is designed specifically for this purpose.
Yes, you can use ChatGPT to paraphrase text to help you express your ideas more clearly, explore different ways of phrasing your arguments, and avoid repetition.
However, it’s not specifically designed for this purpose. We recommend using a specialised tool like Scribbr’s free paraphrasing tool , which will provide a smoother user experience.
Yes, you use ChatGPT to help write your college essay by having it generate feedback on certain aspects of your work (consistency of tone, clarity of structure, etc.).
However, ChatGPT is not able to adequately judge qualities like vulnerability and authenticity. For this reason, it’s important to also ask for feedback from people who have experience with college essays and who know you well. Alternatively, you can get advice using Scribbr’s essay editing service .
No, having ChatGPT write your college essay can negatively impact your application in numerous ways. ChatGPT outputs are unoriginal and lack personal insight.
Furthermore, Passing off AI-generated text as your own work is considered academically dishonest . AI detectors may be used to detect this offense, and it’s highly unlikely that any university will accept you if you are caught submitting an AI-generated admission essay.
However, you can use ChatGPT to help write your college essay during the preparation and revision stages (e.g., for brainstorming ideas and generating feedback).
ChatGPT and other AI writing tools can have unethical uses. These include:
- Reproducing biases and false information
- Using ChatGPT to cheat in academic contexts
- Violating the privacy of others by inputting personal information
However, when used correctly, AI writing tools can be helpful resources for improving your academic writing and research skills. Some ways to use ChatGPT ethically include:
- Following your institution’s guidelines
- Critically evaluating outputs
- Being transparent about how you used the tool
Ask our team
Want to contact us directly? No problem. We are always here for you.
- Chat with us
- Email [email protected]
- Call +44 (0)20 3917 4242
- WhatsApp +31 20 261 6040

Our support team is here to help you daily via chat, WhatsApp, email, or phone between 9:00 a.m. to 11:00 p.m. CET.
Our APA experts default to APA 7 for editing and formatting. For the Citation Editing Service you are able to choose between APA 6 and 7.
Yes, if your document is longer than 20,000 words, you will get a sample of approximately 2,000 words. This sample edit gives you a first impression of the editor’s editing style and a chance to ask questions and give feedback.
How does the sample edit work?
You will receive the sample edit within 24 hours after placing your order. You then have 24 hours to let us know if you’re happy with the sample or if there’s something you would like the editor to do differently.
Read more about how the sample edit works
Yes, you can upload your document in sections.
We try our best to ensure that the same editor checks all the different sections of your document. When you upload a new file, our system recognizes you as a returning customer, and we immediately contact the editor who helped you before.
However, we cannot guarantee that the same editor will be available. Your chances are higher if
- You send us your text as soon as possible and
- You can be flexible about the deadline.
Please note that the shorter your deadline is, the lower the chance that your previous editor is not available.
If your previous editor isn’t available, then we will inform you immediately and look for another qualified editor. Fear not! Every Scribbr editor follows the Scribbr Improvement Model and will deliver high-quality work.
Yes, our editors also work during the weekends and holidays.
Because we have many editors available, we can check your document 24 hours per day and 7 days per week, all year round.
If you choose a 72 hour deadline and upload your document on a Thursday evening, you’ll have your thesis back by Sunday evening!
Yes! Our editors are all native speakers, and they have lots of experience editing texts written by ESL students. They will make sure your grammar is perfect and point out any sentences that are difficult to understand. They’ll also notice your most common mistakes, and give you personal feedback to improve your writing in English.
Every Scribbr order comes with our award-winning Proofreading & Editing service , which combines two important stages of the revision process.
For a more comprehensive edit, you can add a Structure Check or Clarity Check to your order. With these building blocks, you can customize the kind of feedback you receive.
You might be familiar with a different set of editing terms. To help you understand what you can expect at Scribbr, we created this table:
| Types of editing | Available at Scribbr? |
|---|---|
| | This is the “proofreading” in Scribbr’s standard service. It can only be selected in combination with editing. |
| | This is the “editing” in Scribbr’s standard service. It can only be selected in combination with proofreading. |
| | Select the Structure Check and Clarity Check to receive a comprehensive edit equivalent to a line edit. |
| | This kind of editing involves heavy rewriting and restructuring. Our editors cannot help with this. |
View an example
When you place an order, you can specify your field of study and we’ll match you with an editor who has familiarity with this area.
However, our editors are language specialists, not academic experts in your field. Your editor’s job is not to comment on the content of your dissertation, but to improve your language and help you express your ideas as clearly and fluently as possible.
This means that your editor will understand your text well enough to give feedback on its clarity, logic and structure, but not on the accuracy or originality of its content.
Good academic writing should be understandable to a non-expert reader, and we believe that academic editing is a discipline in itself. The research, ideas and arguments are all yours – we’re here to make sure they shine!
After your document has been edited, you will receive an email with a link to download the document.
The editor has made changes to your document using ‘Track Changes’ in Word. This means that you only have to accept or ignore the changes that are made in the text one by one.
It is also possible to accept all changes at once. However, we strongly advise you not to do so for the following reasons:
- You can learn a lot by looking at the mistakes you made.
- The editors don’t only change the text – they also place comments when sentences or sometimes even entire paragraphs are unclear. You should read through these comments and take into account your editor’s tips and suggestions.
- With a final read-through, you can make sure you’re 100% happy with your text before you submit!
You choose the turnaround time when ordering. We can return your dissertation within 24 hours , 3 days or 1 week . These timescales include weekends and holidays. As soon as you’ve paid, the deadline is set, and we guarantee to meet it! We’ll notify you by text and email when your editor has completed the job.
Very large orders might not be possible to complete in 24 hours. On average, our editors can complete around 13,000 words in a day while maintaining our high quality standards. If your order is longer than this and urgent, contact us to discuss possibilities.
Always leave yourself enough time to check through the document and accept the changes before your submission deadline.
Scribbr is specialised in editing study related documents. We check:
- Graduation projects
- Dissertations
- Admissions essays
- College essays
- Application essays
- Personal statements
- Process reports
- Reflections
- Internship reports
- Academic papers
- Research proposals
- Prospectuses
Calculate the costs
The fastest turnaround time is 24 hours.
You can upload your document at any time and choose between four deadlines:
At Scribbr, we promise to make every customer 100% happy with the service we offer. Our philosophy: Your complaint is always justified – no denial, no doubts.
Our customer support team is here to find the solution that helps you the most, whether that’s a free new edit or a refund for the service.
Yes, in the order process you can indicate your preference for American, British, or Australian English .
If you don’t choose one, your editor will follow the style of English you currently use. If your editor has any questions about this, we will contact you.
- Maps & Floorplans
- Libraries A-Z

- Ellis Library (main)
- Engineering Library
- Geological Sciences
- Journalism Library
- Law Library
- Mathematical Sciences
- MU Digital Collections
- Veterinary Medical
- More Libraries...
- Instructional Services
- Course Reserves
- Course Guides
- Schedule a Library Class
- Class Assessment Forms
- Recordings & Tutorials
- Research & Writing Help
- More class resources
- Places to Study
- Borrow, Request & Renew
- Call Numbers
- Computers, Printers, Scanners & Software
- Digital Media Lab
- Equipment Lending: Laptops, cameras, etc.
- Subject Librarians
- Writing Tutors
- More In the Library...
- Undergraduate Students
- Graduate Students
- Faculty & Staff
- Researcher Support
- Distance Learners
- International Students
- More Services for...
- View my MU Libraries Account (login & click on My Library Account)
- View my MOBIUS Checkouts
- Renew my Books (login & click on My Loans)
- Place a Hold on a Book
- Request Books from Depository
- View my ILL@MU Account
- Set Up Alerts in Databases
- More Account Information...
Introduction to Literature Reviews
Introduction.
- Step One: Define
- Step Two: Research
- Step Three: Write
- Suggested Readings
A literature review is a written work that :
- Compiles significant research published on a topic by accredited scholars and researchers;
- Surveys scholarly articles, books, dissertations, conference proceedings, and other sources;
- Examines contrasting perspectives, theoretical approaches, methodologies, findings, results, conclusions.
- Reviews critically, analyzes, and synthesizes existing research on a topic; and,
- Performs a thorough “re” view, “overview”, or “look again” of past and current works on a subject, issue, or theory.
From these analyses, the writer then offers an overview of the current status of a particular area of knowledge from both a practical and theoretical perspective.
Literature reviews are important because they are usually a required step in a thesis proposal (Master's or PhD). The proposal will not be well-supported without a literature review. Also, literature reviews are important because they help you learn important authors and ideas in your field. This is useful for your coursework and your writing. Knowing key authors also helps you become acquainted with other researchers in your field.
Look at this diagram and imagine that your research is the "something new." This shows how your research should relate to major works and other sources.
Olivia Whitfield | Graduate Reference Assistant | 2012-2015
- Next: Step One: Define >>
- Last Updated: Aug 29, 2024 1:55 PM
- URL: https://libraryguides.missouri.edu/literaturereview

Research Methods
- Getting Started
- Literature Review Research
- Research Design
- Research Design By Discipline
- SAGE Research Methods
- Teaching with SAGE Research Methods
Literature Review
- What is a Literature Review?
- What is NOT a Literature Review?
- Purposes of a Literature Review
- Types of Literature Reviews
- Literature Reviews vs. Systematic Reviews
- Systematic vs. Meta-Analysis
Literature Review is a comprehensive survey of the works published in a particular field of study or line of research, usually over a specific period of time, in the form of an in-depth, critical bibliographic essay or annotated list in which attention is drawn to the most significant works.
Also, we can define a literature review as the collected body of scholarly works related to a topic:
- Summarizes and analyzes previous research relevant to a topic
- Includes scholarly books and articles published in academic journals
- Can be an specific scholarly paper or a section in a research paper
The objective of a Literature Review is to find previous published scholarly works relevant to an specific topic
- Help gather ideas or information
- Keep up to date in current trends and findings
- Help develop new questions
A literature review is important because it:
- Explains the background of research on a topic.
- Demonstrates why a topic is significant to a subject area.
- Helps focus your own research questions or problems
- Discovers relationships between research studies/ideas.
- Suggests unexplored ideas or populations
- Identifies major themes, concepts, and researchers on a topic.
- Tests assumptions; may help counter preconceived ideas and remove unconscious bias.
- Identifies critical gaps, points of disagreement, or potentially flawed methodology or theoretical approaches.
- Indicates potential directions for future research.
All content in this section is from Literature Review Research from Old Dominion University
Keep in mind the following, a literature review is NOT:
Not an essay
Not an annotated bibliography in which you summarize each article that you have reviewed. A literature review goes beyond basic summarizing to focus on the critical analysis of the reviewed works and their relationship to your research question.
Not a research paper where you select resources to support one side of an issue versus another. A lit review should explain and consider all sides of an argument in order to avoid bias, and areas of agreement and disagreement should be highlighted.
A literature review serves several purposes. For example, it
- provides thorough knowledge of previous studies; introduces seminal works.
- helps focus one’s own research topic.
- identifies a conceptual framework for one’s own research questions or problems; indicates potential directions for future research.
- suggests previously unused or underused methodologies, designs, quantitative and qualitative strategies.
- identifies gaps in previous studies; identifies flawed methodologies and/or theoretical approaches; avoids replication of mistakes.
- helps the researcher avoid repetition of earlier research.
- suggests unexplored populations.
- determines whether past studies agree or disagree; identifies controversy in the literature.
- tests assumptions; may help counter preconceived ideas and remove unconscious bias.
As Kennedy (2007) notes*, it is important to think of knowledge in a given field as consisting of three layers. First, there are the primary studies that researchers conduct and publish. Second are the reviews of those studies that summarize and offer new interpretations built from and often extending beyond the original studies. Third, there are the perceptions, conclusions, opinion, and interpretations that are shared informally that become part of the lore of field. In composing a literature review, it is important to note that it is often this third layer of knowledge that is cited as "true" even though it often has only a loose relationship to the primary studies and secondary literature reviews.
Given this, while literature reviews are designed to provide an overview and synthesis of pertinent sources you have explored, there are several approaches to how they can be done, depending upon the type of analysis underpinning your study. Listed below are definitions of types of literature reviews:
Argumentative Review This form examines literature selectively in order to support or refute an argument, deeply imbedded assumption, or philosophical problem already established in the literature. The purpose is to develop a body of literature that establishes a contrarian viewpoint. Given the value-laden nature of some social science research [e.g., educational reform; immigration control], argumentative approaches to analyzing the literature can be a legitimate and important form of discourse. However, note that they can also introduce problems of bias when they are used to to make summary claims of the sort found in systematic reviews.
Integrative Review Considered a form of research that reviews, critiques, and synthesizes representative literature on a topic in an integrated way such that new frameworks and perspectives on the topic are generated. The body of literature includes all studies that address related or identical hypotheses. A well-done integrative review meets the same standards as primary research in regard to clarity, rigor, and replication.
Historical Review Few things rest in isolation from historical precedent. Historical reviews are focused on examining research throughout a period of time, often starting with the first time an issue, concept, theory, phenomena emerged in the literature, then tracing its evolution within the scholarship of a discipline. The purpose is to place research in a historical context to show familiarity with state-of-the-art developments and to identify the likely directions for future research.
Methodological Review A review does not always focus on what someone said [content], but how they said it [method of analysis]. This approach provides a framework of understanding at different levels (i.e. those of theory, substantive fields, research approaches and data collection and analysis techniques), enables researchers to draw on a wide variety of knowledge ranging from the conceptual level to practical documents for use in fieldwork in the areas of ontological and epistemological consideration, quantitative and qualitative integration, sampling, interviewing, data collection and data analysis, and helps highlight many ethical issues which we should be aware of and consider as we go through our study.
Systematic Review This form consists of an overview of existing evidence pertinent to a clearly formulated research question, which uses pre-specified and standardized methods to identify and critically appraise relevant research, and to collect, report, and analyse data from the studies that are included in the review. Typically it focuses on a very specific empirical question, often posed in a cause-and-effect form, such as "To what extent does A contribute to B?"
Theoretical Review The purpose of this form is to concretely examine the corpus of theory that has accumulated in regard to an issue, concept, theory, phenomena. The theoretical literature review help establish what theories already exist, the relationships between them, to what degree the existing theories have been investigated, and to develop new hypotheses to be tested. Often this form is used to help establish a lack of appropriate theories or reveal that current theories are inadequate for explaining new or emerging research problems. The unit of analysis can focus on a theoretical concept or a whole theory or framework.
* Kennedy, Mary M. "Defining a Literature." Educational Researcher 36 (April 2007): 139-147.
All content in this section is from The Literature Review created by Dr. Robert Larabee USC
Robinson, P. and Lowe, J. (2015), Literature reviews vs systematic reviews. Australian and New Zealand Journal of Public Health, 39: 103-103. doi: 10.1111/1753-6405.12393

What's in the name? The difference between a Systematic Review and a Literature Review, and why it matters . By Lynn Kysh from University of Southern California

Systematic review or meta-analysis?
A systematic review answers a defined research question by collecting and summarizing all empirical evidence that fits pre-specified eligibility criteria.
A meta-analysis is the use of statistical methods to summarize the results of these studies.
Systematic reviews, just like other research articles, can be of varying quality. They are a significant piece of work (the Centre for Reviews and Dissemination at York estimates that a team will take 9-24 months), and to be useful to other researchers and practitioners they should have:
- clearly stated objectives with pre-defined eligibility criteria for studies
- explicit, reproducible methodology
- a systematic search that attempts to identify all studies
- assessment of the validity of the findings of the included studies (e.g. risk of bias)
- systematic presentation, and synthesis, of the characteristics and findings of the included studies
Not all systematic reviews contain meta-analysis.
Meta-analysis is the use of statistical methods to summarize the results of independent studies. By combining information from all relevant studies, meta-analysis can provide more precise estimates of the effects of health care than those derived from the individual studies included within a review. More information on meta-analyses can be found in Cochrane Handbook, Chapter 9 .
A meta-analysis goes beyond critique and integration and conducts secondary statistical analysis on the outcomes of similar studies. It is a systematic review that uses quantitative methods to synthesize and summarize the results.
An advantage of a meta-analysis is the ability to be completely objective in evaluating research findings. Not all topics, however, have sufficient research evidence to allow a meta-analysis to be conducted. In that case, an integrative review is an appropriate strategy.
Some of the content in this section is from Systematic reviews and meta-analyses: step by step guide created by Kate McAllister.
- << Previous: Getting Started
- Next: Research Design >>
- Last Updated: Jul 15, 2024 10:34 AM
- URL: https://guides.lib.udel.edu/researchmethods

Writing and Presenting Guide
Writing literature reviews, what is a literature review.
"A literature review discusses published information in a particular subject area, and sometimes information in a particular subject area within a certain time period. A literature review can be just a simple summary of the sources, but it usually has an organizational pattern and combines both summary and synthesis. A summary is a recap of the important information of the source, but a synthesis is a re-organization, or a reshuffling, of that information. It might give a new interpretation of old material or combine new with old interpretations. Or it might trace the intellectual progression of the field, including major debates. And depending on the situation, the literature review may evaluate the sources and advise the reader on the most pertinent or relevant." Source: The Writing Center at UNC-Chapel Hill. (2013). Literature Reviews. Retrieved from https://writingcenter.unc.edu/handouts/literature-reviews/ This link opens in a new window
Need help writing a literature review?
Check out these resources:
Helpful Books from the Library
Helpful Web Resources
- Literature Reviews (UNC Writing Center) This link opens in a new window
- Learn How to Write a Review of Literature (The Writing Center at the Univ. of Wisconsin) This link opens in
- The Literature Review (Univ. of Toronto) This link opens in a new window
- Write a Literature Review (University Library at Univ. Of California Santa Cruz) This link opens in a new wi
- Literature Reviews (Ithaca) This link opens in a new window
- << Previous: Writing Papers
- Next: APA Annotated Bibliography >>
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
The PMC website is updating on October 15, 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- J Grad Med Educ
- v.8(3); 2016 Jul
The Literature Review: A Foundation for High-Quality Medical Education Research
a These are subscription resources. Researchers should check with their librarian to determine their access rights.
Despite a surge in published scholarship in medical education 1 and rapid growth in journals that publish educational research, manuscript acceptance rates continue to fall. 2 Failure to conduct a thorough, accurate, and up-to-date literature review identifying an important problem and placing the study in context is consistently identified as one of the top reasons for rejection. 3 , 4 The purpose of this editorial is to provide a road map and practical recommendations for planning a literature review. By understanding the goals of a literature review and following a few basic processes, authors can enhance both the quality of their educational research and the likelihood of publication in the Journal of Graduate Medical Education ( JGME ) and in other journals.
The Literature Review Defined
In medical education, no organization has articulated a formal definition of a literature review for a research paper; thus, a literature review can take a number of forms. Depending on the type of article, target journal, and specific topic, these forms will vary in methodology, rigor, and depth. Several organizations have published guidelines for conducting an intensive literature search intended for formal systematic reviews, both broadly (eg, PRISMA) 5 and within medical education, 6 and there are excellent commentaries to guide authors of systematic reviews. 7 , 8
- A literature review forms the basis for high-quality medical education research and helps maximize relevance, originality, generalizability, and impact.
- A literature review provides context, informs methodology, maximizes innovation, avoids duplicative research, and ensures that professional standards are met.
- Literature reviews take time, are iterative, and should continue throughout the research process.
- Researchers should maximize the use of human resources (librarians, colleagues), search tools (databases/search engines), and existing literature (related articles).
- Keeping organized is critical.
Such work is outside the scope of this article, which focuses on literature reviews to inform reports of original medical education research. We define such a literature review as a synthetic review and summary of what is known and unknown regarding the topic of a scholarly body of work, including the current work's place within the existing knowledge . While this type of literature review may not require the intensive search processes mandated by systematic reviews, it merits a thoughtful and rigorous approach.
Purpose and Importance of the Literature Review
An understanding of the current literature is critical for all phases of a research study. Lingard 9 recently invoked the “journal-as-conversation” metaphor as a way of understanding how one's research fits into the larger medical education conversation. As she described it: “Imagine yourself joining a conversation at a social event. After you hang about eavesdropping to get the drift of what's being said (the conversational equivalent of the literature review), you join the conversation with a contribution that signals your shared interest in the topic, your knowledge of what's already been said, and your intention.” 9
The literature review helps any researcher “join the conversation” by providing context, informing methodology, identifying innovation, minimizing duplicative research, and ensuring that professional standards are met. Understanding the current literature also promotes scholarship, as proposed by Boyer, 10 by contributing to 5 of the 6 standards by which scholarly work should be evaluated. 11 Specifically, the review helps the researcher (1) articulate clear goals, (2) show evidence of adequate preparation, (3) select appropriate methods, (4) communicate relevant results, and (5) engage in reflective critique.
Failure to conduct a high-quality literature review is associated with several problems identified in the medical education literature, including studies that are repetitive, not grounded in theory, methodologically weak, and fail to expand knowledge beyond a single setting. 12 Indeed, medical education scholars complain that many studies repeat work already published and contribute little new knowledge—a likely cause of which is failure to conduct a proper literature review. 3 , 4
Likewise, studies that lack theoretical grounding or a conceptual framework make study design and interpretation difficult. 13 When theory is used in medical education studies, it is often invoked at a superficial level. As Norman 14 noted, when theory is used appropriately, it helps articulate variables that might be linked together and why, and it allows the researcher to make hypotheses and define a study's context and scope. Ultimately, a proper literature review is a first critical step toward identifying relevant conceptual frameworks.
Another problem is that many medical education studies are methodologically weak. 12 Good research requires trained investigators who can articulate relevant research questions, operationally define variables of interest, and choose the best method for specific research questions. Conducting a proper literature review helps both novice and experienced researchers select rigorous research methodologies.
Finally, many studies in medical education are “one-offs,” that is, single studies undertaken because the opportunity presented itself locally. Such studies frequently are not oriented toward progressive knowledge building and generalization to other settings. A firm grasp of the literature can encourage a programmatic approach to research.
Approaching the Literature Review
Considering these issues, journals have a responsibility to demand from authors a thoughtful synthesis of their study's position within the field, and it is the authors' responsibility to provide such a synthesis, based on a literature review. The aforementioned purposes of the literature review mandate that the review occurs throughout all phases of a study, from conception and design, to implementation and analysis, to manuscript preparation and submission.
Planning the literature review requires understanding of journal requirements, which vary greatly by journal ( table 1 ). Authors are advised to take note of common problems with reporting results of the literature review. Table 2 lists the most common problems that we have encountered as authors, reviewers, and editors.
Sample of Journals' Author Instructions for Literature Reviews Conducted as Part of Original Research Article a

Common Problem Areas for Reporting Literature Reviews in the Context of Scholarly Articles

Locating and Organizing the Literature
Three resources may facilitate identifying relevant literature: human resources, search tools, and related literature. As the process requires time, it is important to begin searching for literature early in the process (ie, the study design phase). Identifying and understanding relevant studies will increase the likelihood of designing a relevant, adaptable, generalizable, and novel study that is based on educational or learning theory and can maximize impact.
Human Resources
A medical librarian can help translate research interests into an effective search strategy, familiarize researchers with available information resources, provide information on organizing information, and introduce strategies for keeping current with emerging research. Often, librarians are also aware of research across their institutions and may be able to connect researchers with similar interests. Reaching out to colleagues for suggestions may help researchers quickly locate resources that would not otherwise be on their radar.
During this process, researchers will likely identify other researchers writing on aspects of their topic. Researchers should consider searching for the publications of these relevant researchers (see table 3 for search strategies). Additionally, institutional websites may include curriculum vitae of such relevant faculty with access to their entire publication record, including difficult to locate publications, such as book chapters, dissertations, and technical reports.
Strategies for Finding Related Researcher Publications in Databases and Search Engines

Search Tools and Related Literature
Researchers will locate the majority of needed information using databases and search engines. Excellent resources are available to guide researchers in the mechanics of literature searches. 15 , 16
Because medical education research draws on a variety of disciplines, researchers should include search tools with coverage beyond medicine (eg, psychology, nursing, education, and anthropology) and that cover several publication types, such as reports, standards, conference abstracts, and book chapters (see the box for several information resources). Many search tools include options for viewing citations of selected articles. Examining cited references provides additional articles for review and a sense of the influence of the selected article on its field.
Box Information Resources
- Web of Science a
- Education Resource Information Center (ERIC)
- Cumulative Index of Nursing & Allied Health (CINAHL) a
- Google Scholar
Once relevant articles are located, it is useful to mine those articles for additional citations. One strategy is to examine references of key articles, especially review articles, for relevant citations.
Getting Organized
As the aforementioned resources will likely provide a tremendous amount of information, organization is crucial. Researchers should determine which details are most important to their study (eg, participants, setting, methods, and outcomes) and generate a strategy for keeping those details organized and accessible. Increasingly, researchers utilize digital tools, such as Evernote, to capture such information, which enables accessibility across digital workspaces and search capabilities. Use of citation managers can also be helpful as they store citations and, in some cases, can generate bibliographies ( table 4 ).
Citation Managers

Knowing When to Say When
Researchers often ask how to know when they have located enough citations. Unfortunately, there is no magic or ideal number of citations to collect. One strategy for checking coverage of the literature is to inspect references of relevant articles. As researchers review references they will start noticing a repetition of the same articles with few new articles appearing. This can indicate that the researcher has covered the literature base on a particular topic.
Putting It All Together
In preparing to write a research paper, it is important to consider which citations to include and how they will inform the introduction and discussion sections. The “Instructions to Authors” for the targeted journal will often provide guidance on structuring the literature review (or introduction) and the number of total citations permitted for each article category. Reviewing articles of similar type published in the targeted journal can also provide guidance regarding structure and average lengths of the introduction and discussion sections.
When selecting references for the introduction consider those that illustrate core background theoretical and methodological concepts, as well as recent relevant studies. The introduction should be brief and present references not as a laundry list or narrative of available literature, but rather as a synthesized summary to provide context for the current study and to identify the gap in the literature that the study intends to fill. For the discussion, citations should be thoughtfully selected to compare and contrast the present study's findings with the current literature and to indicate how the present study moves the field forward.
To facilitate writing a literature review, journals are increasingly providing helpful features to guide authors. For example, the resources available through JGME include several articles on writing. 17 The journal Perspectives on Medical Education recently launched “The Writer's Craft,” which is intended to help medical educators improve their writing. Additionally, many institutions have writing centers that provide web-based materials on writing a literature review, and some even have writing coaches.
The literature review is a vital part of medical education research and should occur throughout the research process to help researchers design a strong study and effectively communicate study results and importance. To achieve these goals, researchers are advised to plan and execute the literature review carefully. The guidance in this editorial provides considerations and recommendations that may improve the quality of literature reviews.
- StudySkills@Sheffield
- Academic writing skills
- Critical writing
How to write a literature review
Are you writing a literature review as part of a final year project, dissertation, or thesis, or as a standalone piece of work? This page will work through a process of organising and synthesising your sources and then writing a clear and critical final review.
What is a literature review?
A literature review is an account of the current thinking in a specific area of study. Its purpose is to introduce the reader to what has gone before and often to provide you with a foundation that you can build on with your own research. This traditional form of review is sometimes also referred to as a narrative review.
A literature review will often form a section or chapter of a larger piece of research work, such as a dissertation, thesis, or final year project. It can also be a standalone piece of work.
A literature review will usually do some or all of the following:
- Introduce the reader to a specific area of interest.
- Organise relevant sources thematically, starting with the more general, broader themes and narrowing towards the most specific themes.
- Introduce key theories relevant to the area of study.
- Define your understanding of important terms or language used in the research.
- Include only the most relevant, important or influential sources, carefully selected. It is about quality not quantity!
- Identify gaps or limitations in existing research.
Considering a body of scholarship as a whole (or in relation to each of your themes) will allow you to 'synthesise' multiple sources and produce an overall summary.
Developing a literature review will help you to develop a level of expertise in your chosen area. By consulting and including a unique combination of sources, you will be able to formulate an informed and original perspective. Where relevant, this can drive forward your ongoing research.
Writing a Literature Review workshop: book here
A systematic review is a research methodology, often following a standardised and replicable search method and reporting structure that is specific to your discipline. Visit our guidance on systematic reviews for more information.
Organising your sources
As you encounter more and more relevant sources, you will face an ever-expanding amount of reading for yourself. It would take years to read through all of the literature in a specific field from start to finish.
Academic reading, and particularly the process of 'reading around' a topic, is about selective, or targeted reading. Visit our Reading and understanding information Hub to explore approaches to reading for different purposes.
Creating a Literature Matrix can help you to identify the key things that you want to take away from each source. A literature matrix is a simple spreadsheet where you select column titles to suit the aims of your literature review. Are you interested in the research methodology, the scale of the research, the main conclusions, or something else entirely?
Once you have scanned through a source and pulled out the points you are interested in, you can move onto the next source. Organising your reading in this way will also allow you to identify key themes that are emerging in your reading, which you will be able to use later on to plan your review.
You may want to use a reference management tool to help organise and produce your bibliography. Visit the University of Sheffield Library Reference Management pages here .
Make a copy of our Literature matrix template (Google Sheet) and add/delete columns based on the information you want to collect during your search. Using a spreadsheet means that you can filter and sort your sources, for example, into chronological order, or alphabetically by author.
This downloadable example literature matrix shows how you can lay out your columns.
Synthesising your sources
Once you have a number of sources to work with, you will start to identify key themes emerging. At this point you can start to organise your sources systematically to develop and explore those themes. Can you organise your themes from the broadest to the narrowest and most specific?
A synthesis matrix will help you to identify a thematic structure for your literature review and to understand how the sources that you have found relate to one another. A synthesis matrix is a further spreadsheet that organises your sources by theme and includes a synthesis column, where you can begin to draw out comparisons between the sources.
Once you have identified a number of sources for each theme in your matrix, you should be able to identify the following:
- Do the sources build on or develop one another? This may be a chronological process.
- Do the sources challenge or contradict one another? Do they reveal a debate within the field?
- Do the sources identify an area of particular interest or a gap in the field?
- Do the sources help to fill in gaps or complete a bigger picture?
Your synthesis column provides an opportunity for you to comment on multiple sources considered as a whole. It is a space for your critical voice and interpretation, which is a key part of writing a successful literature review.
Make a copy of our synthesis matrix (Google Sheet) to organise your themes and plan how the relevant sources can be synthesised.
Download a completed example synthesis matrix from NC State University (PDF, 34Kb)
Visit our Producing a literature review interactive tutorial - for further guidance.
Writing your review
Once you have done the background reading and organised your sources using a synthesis matrix, the job of writing your review is simply about adding flesh to the bones. You will need to write your review as a narrative account, but you can use your matrix as a framework to help you do so.
A literature review will usually follow a simple structure:
- Introduction: what is the overall topic area and how have you broken your review down into themes?
- Theme 1: the broadest, most top-level area (perhaps including some background theory that may have influenced your thinking).
- Theme 2, theme 3, theme 4, etc. Your themes should get progressively more specific and closer to the focus of your research.
- Conclusion: how has this informed your thinking and (if the review is part of a bigger project) what are your research aims and objectives?
Your review may be broken down by section headings or be a continuous flow with themes clearly separated in a paragraph structure. Each section or paragraph will describe that theme and finish by summarising your overview of a theme (the synthesis part of the matrix above, which includes your critical analysis).
Our web page How to structure a paragrap h has further guidance to ensure your paragraphs are clear and contain your synthesis and critical analysis.
For advice and feedback on your own review, including referencing, synthesis and academic arguments, please book a writing advisory service appointment.
Make an appointment (student login required)
- How to plan an effective information search
- How to plan a dissertation or final year project
- How to write critically

Use your mySkills portfolio to discover your skillset, reflect on your development, and record your progress.
Advertisement
Mitochondrial Health Markers and Obesity-Related Health in Human Population Studies: A Narrative Review of Recent Literature
- Published: 17 September 2024
Cite this article

- Pei Wen Tung 1 ,
- Vidhu V. Thaker 2 ,
- Dympna Gallagher 3 &
- Allison Kupsco 1
Purpose of Review
This narrative review summarizes current literature on the relationship of mitochondrial biomarkers with obesity-related characteristics, including body mass index and body composition.
Recent Findings
Mitochondria, as cellular powerhouses, play a pivotal role in energy production and the regulation of metabolic process. Altered mitochondrial functions contribute to obesity, yet evidence of the intricate relationship between mitochondrial dynamics and obesity-related outcomes in human population studies is scarce and warrants further attention.
We discuss emerging evidence linking obesity and related health outcomes to impaired oxidative phosphorylation pathways, oxidative stress and mtDNA variants, copy number and methylation, all hallmark of suboptimal mitochondrial function. We also explore the influence of dietary interventions and metabolic and bariatric surgery procedures on restoring mitochondrial attributes of individuals with obesity. Finally, we report on the potential knowledge gaps in the mitochondrial dynamics for human health for future study.
This is a preview of subscription content, log in via an institution to check access.
Access this article
Subscribe and save.
- Get 10 units per month
- Download Article/Chapter or eBook
- 1 Unit = 1 Article or 1 Chapter
- Cancel anytime
Price includes VAT (Russian Federation)
Instant access to the full article PDF.
Rent this article via DeepDyve
Institutional subscriptions

Data Availability
No datasets were generated or analysed during the current study.
Agha M, Agha R. The rising prevalence of obesity: part A: impact on public health. IJS Oncol. 2017;2: e17. https://doi.org/10.1097/IJ9.0000000000000017 .
Article Google Scholar
Bluher M. Obesity: global epidemiology and pathogenesis. Nat Rev Endocrinol. 2019;15:288–9. https://doi.org/10.1038/s41574-019-0176-8 .
Article PubMed Google Scholar
Sanyaolu A, Okorie C, Qi X, Locke J, Rehman S. Childhood and Adolescent Obesity in the United States: A Public Health Concern. Glob Pediatr Health 2019;6:2333794X19891305. https://doi.org/10.1177/2333794X19891305 .
Flegal KM, Kruszon-Moran D, Carroll MD, Fryar CD, Ogden CL. Trends in Obesity Among Adults in the United States, 2005 to 2014. JAMA. 2016;315:2284–91. https://doi.org/10.1001/jama.2016.6458 .
Article PubMed PubMed Central CAS Google Scholar
Ogden CL, Carroll MD, Kit BK, Flegal KM. Prevalence of Childhood and Adult Obesity in the United States, 2011–2012. JAMA. 2014;311:806–14. https://doi.org/10.1001/jama.2014.732 .
Hales CM, Fryar CD, Carroll MD, Freedman DS, Ogden CL. Trends in Obesity and Severe Obesity Prevalence in US Youth and Adults by Sex and Age, 2007–2008 to 2015–2016. JAMA. 2018;319:1723–5. https://doi.org/10.1001/jama.2018.3060 .
Article PubMed PubMed Central Google Scholar
Abdelaal M, le Roux CW, Docherty NG. Morbidity and mortality associated with obesity. Ann Transl Med 2017;5:161. https://doi.org/10.21037/atm.2017.03.107 .
Flegal KM, Williamson DF, Pamuk ER, Rosenberg HM. Estimating Deaths Attributable to Obesity in the United States. Am J Public Health. 2004;94:1486–9.
World Health Organization. Obesity and overweight. Obes Overweight - Fact Sheets 2021. https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight (accessed March 30, 2023).
World Obesity Federation. The World Obesity Atlas 2023. https://www.worldobesityday.org/policy-makers (accessed February 14, 2023).
Restrepo BJ. Obesity Prevalence Among U.S. Adults During the COVID-19 Pandemic. Am J Prev Med. 2022;63:102–6. https://doi.org/10.1016/j.amepre.2022.01.012 .
Spiegelman BM, Flier JS. Obesity and the Regulation of Energy Balance. Cell. 2001;104:531–43. https://doi.org/10.1016/S0092-8674(01)00240-9 .
Article PubMed CAS Google Scholar
de Ferranti S, Mozaffarian D. The perfect storm: obesity, adipocyte dysfunction, and metabolic consequences. Clin Chem. 2008;54:945–55. https://doi.org/10.1373/clinchem.2007.100156 .
Brand MD, Orr AL, Perevoshchikova IV, Quinlan CL. The role of mitochondrial function and cellular bioenergetics in ageing and disease. Br J Dermatol. 2013;169:1–8. https://doi.org/10.1111/bjd.12208 .
Bornstein R, Gonzalez B, Johnson SC. Mitochondrial pathways in human health and aging. Mitochondrion. 2020;54:72–84. https://doi.org/10.1016/j.mito.2020.07.007 .
Heinonen S, Buzkova J, Muniandy M, Kaksonen R, Ollikainen M, Ismail K, et al. Impaired Mitochondrial Biogenesis in Adipose Tissue in Acquired Obesity. Diabetes. 2015;64:3135–45. https://doi.org/10.2337/db14-1937 .
Lindinger A, Peterli R, Peters T, Kern B, von Flüe M, Calame M, et al. Mitochondrial DNA content in human omental adipose tissue. Obes Surg. 2010;20:84–92. https://doi.org/10.1007/s11695-009-9987-3 .
Rautenberg EK, Hamzaoui Y, Coletta DK. Mini-review: Mitochondrial DNA methylation in type 2 diabetes and obesity. Front Endocrinol. 2022;13: 968268. https://doi.org/10.3389/fendo.2022.968268 .
Gallagher D, Heymsfield SB, Heo M, Jebb SA, Murgatroyd PR, Sakamoto Y. Healthy percentage body fat ranges: an approach for developing guidelines based on body mass index. Am J Clin Nutr. 2000;72:694–701. https://doi.org/10.1093/ajcn/72.3.694 .
Lemos T, Gallagher D. Current body composition measurement techniques. Curr Opin Endocrinol Diabetes Obes. 2017;24:310–4. https://doi.org/10.1097/MED.0000000000000360 .
Gallagher D, Andres A, Fields DA, Evans WJ, Kuczmarski R, Lowe WL, et al. Body Composition Measurements from Birth through 5 Years: Challenges, Gaps, and Existing & Emerging Technologies—A National Institutes of Health workshop. Obes Rev Off J Int Assoc Study Obes. 2020;21: e13033. https://doi.org/10.1111/obr.13033 .
Cypess AM. Reassessing Human Adipose Tissue. N Engl J Med. 2022;386:768–79. https://doi.org/10.1056/NEJMra2032804 .
Gallagher D, Kuznia P, Heshka S, Albu J, Heymsfield SB, Goodpaster B, et al. Adipose tissue in muscle: a novel depot similar in size to visceral adipose tissue. Am J Clin Nutr. 2005;81:903–10.
Yim J-E, Heshka S, Albu JB, Heymsfield S, Gallagher D. Femoral-gluteal subcutaneous and intermuscular adipose tissues have independent and opposing relationships with CVD risk. J Appl Physiol. 2008;104:700–7. https://doi.org/10.1152/japplphysiol.01035.2007 .
Gallagher D, Kelley DE, Yim J-E, Spence N, Albu J, Boxt L, et al. Adipose tissue distribution is different in type 2 diabetes2. Am J Clin Nutr. 2009;89:807–14. https://doi.org/10.3945/ajcn.2008.26955 .
Zwick RK, Guerrero-Juarez CF, Horsley V, Plikus MV. Anatomical, Physiological, and Functional Diversity of Adipose Tissue. Cell Metab. 2018;27:68–83. https://doi.org/10.1016/j.cmet.2017.12.002 .
Gallagher D, Heshka S, Kelley DE, Thornton J, Boxt L, Pi-Sunyer FX, et al. Changes in Adipose Tissue Depots and Metabolic Markers Following a 1-Year Diet and Exercise Intervention in Overweight and Obese Patients With Type 2 Diabetes. Diabetes Care. 2014;37:3325–32. https://doi.org/10.2337/dc14-1585 .
Toro-Ramos T, Goodpaster BH, Janumala I, Lin S, Strain GW, Thornton JC, et al. Continued Loss in Visceral and Intermuscular Adipose Tissue in Weight-Stable Women Following Bariatric Surgery. Obes Silver Spring Md. 2015;23:62–9. https://doi.org/10.1002/oby.20932 .
Saely CH, Geiger K, Drexel H. Brown versus white adipose tissue: a mini-review. Gerontology. 2012;58:15–23. https://doi.org/10.1159/000321319 .
Zhu Q, An YA, Scherer PE. Mitochondrial regulation and white adipose tissue homeostasis. Trends Cell Biol. 2022;32:351–64. https://doi.org/10.1016/j.tcb.2021.10.008 .
Giralt M, Villarroya F. White, Brown, Beige/Brite: Different Adipose Cells for Different Functions? Endocrinology. 2013;154:2992–3000. https://doi.org/10.1210/en.2013-1403 .
Cypess AM, Lehman S, Williams G, Tal I, Rodman D, Goldfine AB, et al. Identification and Importance of Brown Adipose Tissue in Adult Humans. N Engl J Med. 2009;360:1509–17. https://doi.org/10.1056/NEJMoa0810780 .
Pfannenberg C, Werner MK, Ripkens S, Stef I, Deckert A, Schmadl M, et al. Impact of Age on the Relationships of Brown Adipose Tissue With Sex and Adiposity in Humans. Diabetes. 2010;59:1789–93. https://doi.org/10.2337/db10-0004 .
Abernathy RP, Black DR. Healthy body weights: an alternative perspective. Am J Clin Nutr. 1996;63:448S-451S. https://doi.org/10.1093/ajcn/63.3.448 .
Choe SS, Huh JY, Hwang IJ, Kim JI, Kim JB. Adipose Tissue Remodeling: Its Role in Energy Metabolism and Metabolic Disorders. Front Endocrinol. 2016;7:30. https://doi.org/10.3389/fendo.2016.00030 .
Fuster JJ, Ouchi N, Gokce N, Walsh K. Obesity-induced Changes in Adipose Tissue Microenvironment and Their Impact on Cardiovascular Disease. Circ Res. 2016;118:1786–807. https://doi.org/10.1161/CIRCRESAHA.115.306885 .
Greenberg AS, Obin MS. Obesity and the role of adipose tissue in inflammation and metabolism. Am J Clin Nutr. 2006;83:461S-465S. https://doi.org/10.1093/ajcn/83.2.461S .
Haczeyni F, Bell-Anderson KS, Farrell GC. Causes and mechanisms of adipocyte enlargement and adipose expansion. Obes Rev Off J Int Assoc Study Obes. 2018;19:406–20. https://doi.org/10.1111/obr.12646 .
Article CAS Google Scholar
Clemente-Suárez VJ, Redondo-Flórez L, Beltrán-Velasco AI, Martín-Rodríguez A, Martínez-Guardado I, Navarro-Jiménez E, et al. The Role of Adipokines in Health and Disease. Biomedicines. 2023;11:1290. https://doi.org/10.3390/biomedicines11051290 .
Ahima RS, Flier JS. Adipose Tissue as an Endocrine Organ. Trends Endocrinol Metab. 2000;11:327–32. https://doi.org/10.1016/S1043-2760(00)00301-5 .
Kershaw EE, Flier JS. Adipose Tissue as an Endocrine Organ. J Clin Endocrinol Metab. 2004;89:2548–56. https://doi.org/10.1210/jc.2004-0395 .
Li S, Shin HJ, Ding EL, van Dam RM. Adiponectin Levels and Risk of Type 2 Diabetes: A Systematic Review and Meta-analysis. JAMA. 2009;302:179–88. https://doi.org/10.1001/jama.2009.976 .
Gariballa S, Alkaabi J, Yasin J, Al EA. Total adiponectin in overweight and obese subjects and its response to visceral fat loss. BMC Endocr Disord. 2019;19:55. https://doi.org/10.1186/s12902-019-0386-z .
Fernández-Sánchez A, Madrigal-Santillán E, Bautista M, Esquivel-Soto J, Morales-González A, Esquivel-Chirino C, et al. Inflammation, oxidative stress, and obesity. Int J Mol Sci. 2011;12:3117–32. https://doi.org/10.3390/ijms12053117 .
de Mello AH, Costa AB, Engel JDG, Rezin GT. Mitochondrial dysfunction in obesity. Life Sci. 2018;192:26–32. https://doi.org/10.1016/j.lfs.2017.11.019 .
Bournat JC, Brown CW. Mitochondrial Dysfunction in Obesity. Curr Opin Endocrinol Diabetes Obes. 2010;17:446–52. https://doi.org/10.1097/MED.0b013e32833c3026 .
Vyas CM, Ogata S, Iii CFR, Mischoulon D, Chang G, Cook NR, et al. Lifestyle and behavioral factors and mitochondrial DNA copy number in a diverse cohort of mid-life and older adults. PLoS ONE. 2020;15: e0237235. https://doi.org/10.1371/journal.pone.0237235 .
Filograna R, Mennuni M, Alsina D, Larsson N-G. Mitochondrial DNA copy number in human disease: the more the better? FEBS Lett. 2021;595:976–1002. https://doi.org/10.1002/1873-3468.14021 .
Castellani CA, Longchamps RJ, Sumpter JA, Newcomb CE, Lane JA, Grove ML, et al. Mitochondrial DNA copy number can influence mortality and cardiovascular disease via methylation of nuclear DNA CpGs. Genome Med. 2020;12:84. https://doi.org/10.1186/s13073-020-00778-7 .
Hunter CA, Kartal F, Koc ZC, Murphy T, Kim JH, Denvir J, et al. Mitochondrial oxidative phosphorylation is impaired in TALLYHO mice, a new obesity and type 2 diabetes animal model. Int J Biochem Cell Biol. 2019;116: 105616. https://doi.org/10.1016/j.biocel.2019.105616 .
Brestoff JR, Wilen CB, Moley JR, Li Y, Zou W, Malvin NP, et al. Intercellular Mitochondria Transfer to Macrophages Regulates White Adipose Tissue Homeostasis and Is Impaired in Obesity. Cell Metab. 2021;33:270-282.e8. https://doi.org/10.1016/j.cmet.2020.11.008 .
Schöttl T, Kappler L, Fromme T, Klingenspor M. Limited OXPHOS capacity in white adipocytes is a hallmark of obesity in laboratory mice irrespective of the glucose tolerance status. Mol Metab. 2015;4:631–42. https://doi.org/10.1016/j.molmet.2015.07.001 .
Heinonen S, Muniandy M, Buzkova J, Mardinoglu A, Rodríguez A, Frühbeck G, et al. Mitochondria-related transcriptional signature is downregulated in adipocytes in obesity: a study of young healthy MZ twins. Diabetologia. 2017;60:169–81. https://doi.org/10.1007/s00125-016-4121-2 .
Honecker J, Ruschke S, Seeliger C, Laber S, Strobel S, Pröll P, et al. Transcriptome and fatty-acid signatures of adipocyte hypertrophy and its non-invasive MR-based characterization in human adipose tissue. eBioMedicine. 2022;79:104020. https://doi.org/10.1016/j.ebiom.2022.104020 .
Takamura T, Misu H, Matsuzawa-Nagata N, Sakurai M, Ota T, Shimizu A, et al. Obesity Upregulates Genes Involved in Oxidative Phosphorylation in Livers of Diabetic Patients. Obesity. 2008;16:2601–9. https://doi.org/10.1038/oby.2008.419 .
Chattopadhyay M, Khemka VK, Chatterjee G, Ganguly A, Mukhopadhyay S, Chakrabarti S. Enhanced ROS production and oxidative damage in subcutaneous white adipose tissue mitochondria in obese and type 2 diabetes subjects. Mol Cell Biochem. 2015;399:95–103. https://doi.org/10.1007/s11010-014-2236-7 .
Lefranc C, Friederich-Persson M, Palacios-Ramirez R, Nguyen Dinh Cat A. Mitochondrial oxidative stress in obesity: role of the mineralocorticoid receptor. J Endocrinol 2018;238:R143–59. https://doi.org/10.1530/JOE-18-0163 .
van der Kolk BW, Muniandy M, Kaminska D, Alvarez M, Ko A, Miao Z, et al. Differential Mitochondrial Gene Expression in Adipose Tissue Following Weight Loss Induced by Diet or Bariatric Surgery. J Clin Endocrinol Metab. 2021;106:1312–24. https://doi.org/10.1210/clinem/dgab072 .
Ngo DTM, Sverdlov AL, Karki S, Macartney-Coxson D, Stubbs RS, Farb MG, et al. Oxidative modifications of mitochondrial complex II are associated with insulin resistance of visceral fat in obesity. Am J Physiol-Endocrinol Metab. 2018;316:E168–77. https://doi.org/10.1152/ajpendo.00227.2018 .
Hadrava Vanova K, Kraus M, Neuzil J, Rohlena J. Mitochondrial complex II and reactive oxygen species in disease and therapy. Redox Rep Commun Free Radic Res n.d.;25:26–32. https://doi.org/10.1080/13510002.2020.1752002 .
Bezawork-Geleta A, Rohlena J, Dong L, Pacak K, Neuzil J. Mitochondrial Complex II: At the Crossroads. Trends Biochem Sci. 2017;42:312–25. https://doi.org/10.1016/j.tibs.2017.01.003 .
Varela-Rodríguez BM, Juiz-Valiña P, Varela L, Outeiriño-Blanco E, Bravo SB, García-Brao MJ, et al. Beneficial Effects of Bariatric Surgery-Induced by Weight Loss on the Proteome of Abdominal Subcutaneous Adipose Tissue. J Clin Med. 2020;9:213. https://doi.org/10.3390/jcm9010213 .
Yin X, Lanza IR, Swain JM, Sarr MG, Nair KS, Jensen MD. Adipocyte Mitochondrial Function Is Reduced in Human Obesity Independent of Fat Cell Size. J Clin Endocrinol Metab. 2014;99:E209–16. https://doi.org/10.1210/jc.2013-3042 .
Taylor RW, Turnbull DM. Mitochondrial DNA mutations in human disease. Nat Rev Genet. 2005;6:389–402. https://doi.org/10.1038/nrg1606 .
Parakatselaki M-E, Ladoukakis ED. mtDNA Heteroplasmy: Origin, Detection, Significance, and Evolutionary Consequences. Life. 2021;11:633. https://doi.org/10.3390/life11070633 .
Stewart JB, Chinnery PF. The dynamics of mitochondrial DNA heteroplasmy: implications for human health and disease. Nat Rev Genet. 2015;16:530–42. https://doi.org/10.1038/nrg3966 .
Rossignol R, Faustin B, Rocher C, Malgat M, Mazat J-P, Letellier T. Mitochondrial threshold effects. Biochem J. 2003;370:751–62. https://doi.org/10.1042/BJ20021594 .
Holt IJ, Harding AE, Petty RK, Morgan-Hughes JA. A new mitochondrial disease associated with mitochondrial DNA heteroplasmy. Am J Hum Genet. 1990;46:428–33.
PubMed PubMed Central CAS Google Scholar
Stewart JB, Chinnery PF. Extreme heterogeneity of human mitochondrial DNA from organelles to populations. Nat Rev Genet. 2021;22:106–18. https://doi.org/10.1038/s41576-020-00284-x .
Knoll N, Jarick I, Volckmar A-L, Klingenspor M, Illig T, Grallert H, et al. Mitochondrial DNA Variants in Obesity. PLoS ONE. 2014;9: e94882. https://doi.org/10.1371/journal.pone.0094882 .
Yang T-L, Guo Y, Shen H, Lei S-F, Liu Y-J, Li J, et al. Genetic Association Study of Common Mitochondrial Variants on Body Fat Mass. PLoS ONE. 2011;6: e21595. https://doi.org/10.1371/journal.pone.0021595 .
Demir D, Türkkahraman D, Samur AA, Lüleci G, Akçurin S, M. Alper Ö. Mitochondrial ATPase Subunit 6 and Cytochrome B Gene Variations in Obese Turkish Children. J Clin Res Pediatr Endocrinol 2014;6:209–15. https://doi.org/10.4274/jcrpe.1601 .
Okura T, Koda M, Ando F, Niino N, Tanaka M, Shimokata H. Association of the mitochondrial DNA 15497G/A polymorphism with obesity in a middle-aged and elderly Japanese population. Hum Genet. 2003;113:432–6. https://doi.org/10.1007/s00439-003-0983-8 .
Wang Y, Palmfeldt J, Gregersen N, Makhov AM, Conway JF, Wang M, et al. Mitochondrial fatty acid oxidation and the electron transport chain comprise a multifunctional mitochondrial protein complex. J Biol Chem. 2019;294:12380–91. https://doi.org/10.1074/jbc.RA119.008680 .
Furukawa S, Fujita T, Shimabukuro M, Iwaki M, Yamada Y, Nakajima Y, et al. Increased oxidative stress in obesity and its impact on metabolic syndrome. J Clin Invest. 2004;114:1752–61. https://doi.org/10.1172/JCI200421625 .
Flaquer A, Baumbach C, Kriebel J, Meitinger T, Peters A, Waldenberger M, et al. Mitochondrial Genetic Variants Identified to Be Associated with BMI in Adults. PLoS ONE. 2014;9: e105116. https://doi.org/10.1371/journal.pone.0105116 .
Grant SFA, Glessner JT, Bradfield JP, Zhao J, Tirone JE, Berkowitz RI, et al. Lack of relationship between mitochondrial heteroplasmy or variation and childhood obesity. Int J Obes. 2012;36:80–3. https://doi.org/10.1038/ijo.2011.206 .
Rivera MA, Pérusse L, Gagnon J, Dionne FT, Leon AS, Rao DC, et al. A mitochondrial DNA D-loop polymorphism and obesity in three cohorts of women. Int J Obes. 1999;23:666–8. https://doi.org/10.1038/sj.ijo.0800900 .
Mishmar D, Ruiz-Pesini E, Golik P, Macaulay V, Clark AG, Hosseini S, et al. Natural selection shaped regional mtDNA variation in humans. Proc Natl Acad Sci. 2003;100:171–6. https://doi.org/10.1073/pnas.0136972100 .
Van Oven M, Kayser M. Updated comprehensive phylogenetic tree of global human mitochondrial DNA variation. Hum Mutat. 2009;30:E386–94. https://doi.org/10.1002/humu.20921 .
PhyloTree.org | tree | main n.d. https://www.phylotree.org/tree/index.htm (accessed February 23, 2024).
Chalkia D, Chang Y-C, Derbeneva O, Lvova M, Wang P, Mishmar D, et al. Mitochondrial DNA associations with East Asian metabolic syndrome. Biochim Biophys Acta Bioenerg. 2018;1859:878–92. https://doi.org/10.1016/j.bbabio.2018.07.002 .
Fang EF, Lautrup S, Hou Y, Demarest TG, Croteau DL, Mattson MP, et al. NAD+ in Aging: Molecular Mechanisms and Translational Implications. Trends Mol Med. 2017;23:899–916. https://doi.org/10.1016/j.molmed.2017.08.001 .
Nardelli C, Labruna G, Liguori R, Mazzaccara C, Ferrigno M, Capobianco V, et al. Haplogroup T Is an Obesity Risk Factor: Mitochondrial DNA Haplotyping in a Morbid Obese Population from Southern Italy. BioMed Res Int. 2013;2013: 631082. https://doi.org/10.1155/2013/631082 .
Ebner S, Mangge H, Langhof H, Halle M, Siegrist M, Aigner E, et al. Mitochondrial Haplogroup T Is Associated with Obesity in Austrian Juveniles and Adults. PLoS ONE. 2015;10: e0135622. https://doi.org/10.1371/journal.pone.0135622 .
Castro MG, Terrados N, Reguero JR, Alvarez V, Coto E. Mitochondrial haplogroup T is negatively associated with the status of elite endurance athlete. Mitochondrion. 2007;7:354–7. https://doi.org/10.1016/j.mito.2007.06.002 .
Dashti M, Alsaleh H, Rodriguez-Flores JL, Eaaswarkhanth M, Al-Mulla F, Thanaraj TA. Mitochondrial haplogroup J associated with higher risk of obesity in the Qatari population. Sci Rep. 2021;11:1091. https://doi.org/10.1038/s41598-020-80040-7 .
Veronese N, Stubbs B, Koyanagi A, Vaona A, Demurtas J, Schofield P, et al. Mitochondrial genetic haplogroups and incident obesity: a longitudinal cohort study. Eur J Clin Nutr. 2018;72:587–92. https://doi.org/10.1038/s41430-018-0097-y .
Sharma P, Sampath H. Mitochondrial DNA Integrity: Role in Health and Disease. Cells. 2019;8:100. https://doi.org/10.3390/cells8020100 .
Gustafson MA, Sullivan ED, Copeland WC. Consequences of Compromised Mitochondrial Genome Integrity. DNA Repair. 2020;93: 102916. https://doi.org/10.1016/j.dnarep.2020.102916 .
Picard M. Blood Mitochondrial DNA Copy Number: What Are We Counting? Mitochondrion. 2021;60:1–11. https://doi.org/10.1016/j.mito.2021.06.010 .
Bordoni L, Smerilli V, Nasuti C, Gabbianelli R. Mitochondrial DNA methylation and copy number predict body composition in a young female population. J Transl Med. 2019;17:399. https://doi.org/10.1186/s12967-019-02150-9 .
Lee J-Y, Lee D-C, Im J-A, Lee J-W. Mitochondrial DNA Copy Number in Peripheral Blood Is Independently Associated with Visceral Fat Accumulation in Healthy Young Adults. Int J Endocrinol. 2014;2014: 586017. https://doi.org/10.1155/2014/586017 .
Meng S, Wu S, Liang L, Liang G, Giovannucci E, Vivo ID, et al. Leukocyte mitochondrial DNA copy number, anthropometric indices, and weight change in US women. Oncotarget 2016;7:60676–86. https://doi.org/10.18632/oncotarget.10325 .
Zheng LD, Linarelli LE, Liu L, Wall SS, Greenawald MH, Seidel RW, et al. Insulin resistance is associated with epigenetic and genetic regulation of mitochondrial DNA in obese humans. Clin Epigenetics. 2015;7:60. https://doi.org/10.1186/s13148-015-0093-1 .
Liu X, Longchamps RJ, Wiggins KL, Raffield LM, Bielak LF, Zhao W, et al. Association of mitochondrial DNA copy number with cardiometabolic diseases. Cell Genomics. 2021;1: 100006. https://doi.org/10.1016/j.xgen.2021.100006 .
Hang D, Nan H, Kværner AS, De Vivo I, Chan AT, Hu Z, et al. Longitudinal associations of lifetime adiposity with leukocyte telomere length and mitochondrial DNA copy number. Eur J Epidemiol. 2018;33:485–95. https://doi.org/10.1007/s10654-018-0382-z .
Gyllenhammer LE, Entringer S, Buss C, Wadhwa PD. Developmental programming of mitochondrial biology: a conceptual framework and review. Proc R Soc B Biol Sci. 2020;287:20192713. https://doi.org/10.1098/rspb.2019.2713 .
Peng J, Ramatchandirin B, Pearah A, Maheshwari A, He L. Development and Functions of Mitochondria in Early Life. Newborn Clarksville Md. 2022;1:131–41. https://doi.org/10.5005/jp-journals-11002-0013 .
Diaz-Vegas A, Sanchez-Aguilera P, Krycer JR, Morales PE, Monsalves-Alvarez M, Cifuentes M, et al. Is Mitochondrial Dysfunction a Common Root of Noncommunicable Chronic Diseases? Endocr Rev. 2020;41:bnaa005. https://doi.org/10.1210/endrev/bnaa005 .
Kaaman M, Sparks LM, van Harmelen V, Smith SR, Sjölin E, Dahlman I, et al. Strong association between mitochondrial DNA copy number and lipogenesis in human white adipose tissue. Diabetologia. 2007;50:2526–33. https://doi.org/10.1007/s00125-007-0818-6 .
Seo M, Kim H, Noh H, Jeon JS, Byun DW, Kim SH, et al. Effect of bariatric surgery on circulating and urinary mitochondrial DNA copy numbers in obesity with or without diabetes. BMJ Open Diabetes Res Care. 2020;8: e001372. https://doi.org/10.1136/bmjdrc-2020-001372 .
Lee H, Oh S, Yang W, Park R, Kim H, Jeon JS, et al. Bariatric Surgery Reduces Elevated Urinary Mitochondrial DNA Copy Number in Patients With Obesity. J Clin Endocrinol Metab. 2019;104:2257–66. https://doi.org/10.1210/jc.2018-01935 .
Mechta M, Ingerslev LR, Fabre O, Picard M, Barrès R. Evidence Suggesting Absence of Mitochondrial DNA Methylation. Front Genet 2017;8 https://doi.org/10.3389/fgene.2017.00166
Stoccoro A, Coppedè F. Mitochondrial DNA Methylation and Human Diseases. Int J Mol Sci. 2021;22:4594. https://doi.org/10.3390/ijms22094594 .
Bordoni L, Perugini J, Petracci I, Mercurio ED, Lezoche G, Guerrieri M, et al. Mitochondrial DNA in Visceral Adipose Tissue in Severe Obesity: From Copy Number to D-Loop Methylation. Front Biosci Landmark Ed 2022; 27:172. https://doi.org/10.31083/j.fbl2706172 .
Zong Y, Li H, Liao P, Chen L, Pan Y, Zheng Y, et al. Mitochondrial dysfunction: mechanisms and advances in therapy. Signal Transduct Target Ther. 2024;9:1–29. https://doi.org/10.1038/s41392-024-01839-8 .
Wu Z, Chen L, Guo W, Wang J, Ni H, Liu J, et al. Oral mitochondrial transplantation using nanomotors to treat ischaemic heart disease. Nat Nanotechnol 2024:1–11. https://doi.org/10.1038/s41565-024-01681-7 .
Lightowlers RN, Chrzanowska‐Lightowlers ZM, Russell OM. Mitochondrial transplantation—a possible therapeutic for mitochondrial dysfunction? EMBO Rep 2020 21:e50964. https://doi.org/10.15252/embr.202050964 .
Download references
The authors did not receive funding from any organization for the submitted work.
Author information
Authors and affiliations.
Department of Environmental Health Sciences, Mailman School of Public Health, Columbia University, New York, NY, USA
Pei Wen Tung & Allison Kupsco
Department of Pediatrics, Columbia University Irving Medical Center, New York, NY, USA
Vidhu V. Thaker
Department of Medicine, Columbia University Irving Medical Center , New York, NY, USA
Dympna Gallagher
You can also search for this author in PubMed Google Scholar
Contributions
PWT drafted the initial version of the manuscript and prepared the table and figure. All authors participated in the writing and reviewing of subsequent versions. All authors approved the submitted version of the manuscript.
Corresponding author
Correspondence to Pei Wen Tung .
Ethics declarations
Conflicts of interest.
The authors declare no competing interests.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
Reprints and permissions
About this article
Tung, P.W., Thaker, V.V., Gallagher, D. et al. Mitochondrial Health Markers and Obesity-Related Health in Human Population Studies: A Narrative Review of Recent Literature. Curr Obes Rep (2024). https://doi.org/10.1007/s13679-024-00588-7
Download citation
Accepted : 29 August 2024
Published : 17 September 2024
DOI : https://doi.org/10.1007/s13679-024-00588-7
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Mitochondrial DNA
- Bariatric Surgery
- Epidemiology
- Mitochondrial Biomarkers
- Find a journal
- Publish with us
- Track your research
Thank you for visiting nature.com. You are using a browser version with limited support for CSS. To obtain the best experience, we recommend you use a more up to date browser (or turn off compatibility mode in Internet Explorer). In the meantime, to ensure continued support, we are displaying the site without styles and JavaScript.
- View all journals
- Explore content
- About the journal
- Publish with us
- Sign up for alerts
Open access
- Published: 17 September 2024
Data access arrangements in genomic research consortia
- Dianne Nicol ORCID: orcid.org/0000-0002-6553-2839 1 ,
- Jane Nielsen 1 &
- Madeleine Archer 2
Scientific Reports volume 14 , Article number: 21685 ( 2024 ) Cite this article
Metrics details
- Medical genomics
- Personalized medicine
One of the most common terms that is used to describe entities responsible for sharing genomic data for research purposes is ‘genomic research consortium’. However, there is a lack of clarity around the language used by consortia to describe their data sharing arrangements. Calls have been made for more uniform terminology. This article reports on a review of the genomic research consortium literature illustrating a wide diversity in the language that has been used over time to describe the access arrangements of these entities. The second component of this research involved an examination of publicly available information from a dataset of 98 consortia. This analysis further illustrates the wide diversity in the access arrangements adopted by genomic research consortia. A total of 12 different access arrangements were identified, including four simple forms (open, consortium, managed and registered access) and eight more complex tiered forms (for example, a combination of consortium, managed and open access). The majority of consortia utilised some form of tiered access, often following the policy requirements of funders like the US National Institutes of Health and the UK Wellcome Trust. It was not always easy to precisely identify the access arrangements of individual consortia. Greater consistency, clarity and transparency is likely to be of benefit to donors, depositors and accessors alike. More work needs to be done to achieve this end.
Introduction
The genomic research landscape is teeming with hundreds of bodies, organisations, groups and teams which use a variety of terms to describe themselves. One of the most common terms that is used to describe many of these entities is ‘consortium’. This term emerged in the early 2000s to describe a particular type of research collaboration 1 . Core elements identified in the literature include: collaboration and/or partnership; pooling of resources; and efforts to reach a common/shared goal 2 , 3 , 4 , 5 , 6 , 7 . In this article, we rely on the following definition of genomic research consortia: ‘a group of scientists from multiple institutions who have agreed to cooperative research efforts involving, but not limited to, pooling of information from more than one study for the purpose of combined analyses and collaborative projects’ 5 .
The overarching purpose of genomic research consortia is to ensure that data generated by consortium members are shared for research purposes 8 . Establishing mechanisms to facilitate this, though vital to the genomics research effort, is not without scientific and technical challenges. The ongoing development of standards and policies for genomic data sharing by organisations like the Global Alliance for Genomics and Health (GA4GH) is addressing many of these challenges 9 . GA4GH also recognises these challenges are intimately interconnected with the regulatory and ethical concerns that arise whenever human genomic data is shared. The GA4GH Regulatory and Ethics Workstream (REWS) uses a global human rights framework to provide guidance on the regulatory, ethical, and social implications of genomic research and data sharing, and the development of standards and policies to address them 10 , 11 .
Funding agencies have also started to impose their own standards for the governance of genomic research funded by them. The US-based National Institutes of Health (NIH), for example formulated a policy on sharing genomic data in 2014 12 , which sits alongside its more recent broader data management and sharing policy 13 . One key feature is the expectation that researchers will ensure broad and responsible sharing. Investigators and their institutions are expected to provide the NIH with a Genomic Data Sharing Plan showing how the policy will be followed, and to submit large-scale human genomic and associated data to NIH-approved data repositories. Likewise, Wellcome in the UK has requirements regarding data access, including an explicit outputs management plan 14 .
GA4GH has been in existence for only eleven years and the NIH Genomic Data Sharing Policy came into effect shortly after that. Prior to their existence, the growth in genomic research consortia occurred largely organically. Although many of them are now bound by the policies of the NIH and other funding agencies, and/or are starting to adopt GA4GH standards, others continue to operate under their own governance arrangements. Assessing the adequacy and appropriateness of these governance arrangements is challenging, given the sheer number and diversity of entities that use this title. There are various reasons why it is important for genomic research consortia to be transparent in their governance arrangements, not least because they host data sourced from members of the public and generally obtained using public funding. In their examination of good governance of human genomic data, O’Doherty et al. 15 describe transparency as ‘a meta-function of good governance’.
The research reported in this article examined governance of data access by genomic research consortia. It included a review relevant general academic literature, and creation of a dataset of academic literature and other documentation relating to specific consortia.
Materials and methods
Preliminary reviews of information relating to governance of data access in genomic research consortia were undertaken within the authors’ existing library of over 800 academic articles and other documents. A search was then undertaken on PubMed using the terms: health/genetic/genomic/consortia/consortium. Eighty-nine documents were ultimately selected and compiled for analysis in 2019. These documents were supplemented by more recent literature during 2020 to 2024. This library was not intended to be a comprehensive catalogue of every published document about governance of data access in genomic research consortia. Rather, it was intended to provide us with a sufficiently large sample to show common themes and points of difference.
An initial list of genomic research consortia was drawn from a catalogue of genomic data sharing initiatives compiled by GA4GH (it should be noted that this catalogue is no longer available on the GA4GH website). We also scoured other publicly available lists of consortia, including: a compilation of data sharing repositories available on the NIH website 16 ; repositories recommended by the journal Nature; and a list of GA4GH driver projects 17 . We acknowledge that by using GA4GH and NIH as our primary sources, there might be some skewing of our datasets towards North America. However, given the dominance of the US in genomic research and the NIH in funding this research, it is inevitable that the vast majority of consortia on our list would have their origins in this jurisdiction. We also note that it was not our intention that these searches would yield a definitive list of all genomic research consortia currently in existence. Instead, our aim was to create a reasonably comprehensive dataset of entities that self-identify as genomic research consortia. We acknowledge, however, that we may have missed some consortia which may have developed interesting and novel data access arrangements.
Based on our reliance on the definition of genomic research consortia proposed by Burgio et al., 5 we excluded entities that were otherwise included in our search results on several grounds:
entities that do not engage in research into genomics at the molecular level (for example the Human Cell Atlas), on the basis that their primary focus is not genomics;
repositories, archives and databases that store genomic data, such as the US-based database of Genotypes and Phenotypes (dbGaP). dbGaP is a repository established by the NIH and other government agencies to facilitate sharing of genotypic and phenotypic information 18 . Although dbGaP and other repositories do not participate in genomic research per se, consortia that deposit data in these repositories may be bound by their data access policies. In this respect their policies are relevant to our analysis;
entities whose only role is to analyse data, on the basis that they are not engaged in collaborative research; and
funding bodies (such as NIH and Wellcome), and bodies whose role is to develop policies and standards for data sharing (such as GA4GH), given that their role is to facilitate data sharing rather than being actively involved in genomic research. The model data sharing policies and other documents developed by these bodies are nevertheless relevant because they are often adopted by genomic research consortia.
In total, 102 consortia were identified by one of us (MA) together with another research assistant. This dataset was subsequently analysed separately by DN and JN and reduced to 98 genomic research consortia. Four entries were removed because they were shown not to be actively involved in genomic research and one was removed because the consortium had been dissolved some years prior to our project and no information was available about its governance. Although other consortia have also completed their work, information on their governance arrangements is still available (as are their datasets). One entry was split into two (ICGC and ICGC-ARGO) on the basis that the nature of the consortium (including the data access arrangements) changed on the creation of ICGC-ARGO.
A dataset of foundational articles and governance policies, guidelines, agreements and other documentation made publicly available by individual genomic research consortia was created to facilitate examination of specific governance arrangements. Where preliminary searches failed to reveal details on data access arrangements, consortium administrators were contacted and asked to provide relevant links, which resulted in some further additions to the dataset. The dataset was reviewed and analysed separately by DN and JN in 2023 for details on access arrangements. We then jointly sorted access arrangements into categories to generate a shared terminology. Further online searches of consortia websites were undertaken where the original dataset did not reveal sufficient information. A full list of consortia, together with their purported access arrangements and other demographic features, is provided in Supplementary Materials. Access to the full dataset is available on request from the authors (except for some documents where the consortium administrators requested confidentiality).
Preliminary observations on terminology
The European Expert Advisory Group on Data Access expressed concern about the lack of a shared terminology in the data sharing landscape in 2015. In response, the group attempted to impose some consistency in the terms employed to describe data sharing processes and the actors involved in them 19 . In a further attempt to address concerns about the lack of common terminology, GA4GH developed a ‘Data Sharing Lexicon’ in 2016 20 . Some of the more well-resourced genomic research consortia also imposed their own requirements for consistency in language and have been highly transparent in defining and explaining this. An exemplar is the ICGC 21 .
Despite these attempts to introduce a shared terminology, a host of terms continue to be employed to describe consortia activities. In particular, diverse terms have been used to describe the procedures involved in granting or facilitating data access. Some of these include: controlled access 22 , 23 , 24 , 25 , managed access 21 , 26 , 27 , tiered access 22 , 24 , unrestricted access, open access 24 , 27 , 28 , registered access 21 , 24 , authenticated, charged, exclusive and password access 29 , a passport model of access 30 and more. There is a lack of clarity about the extent to which these terms are truly distinct, related, or interchangeable with one another.
Towards a shared terminology for access arrangements
Recognising the broad range of language that used to describe data access arrangements in genomic research consortia, we designated five major categories from our analysis: consortium access, open access, registered access, managed access and tiered access. We describe each category in more detail below.
Consortium access
Given the rationale for the establishment of genomic research consortia is to share data, we expected that members of genomic research consortia share data with other members on a reciprocal basis 8 . However, it does not necessarily follow that members will be willing to share their data outside of the consortium 31 .
We use the term consortium access (CA) to describe the circumstances where consortium members only share data openly within the consortium. This puts consortium members in a privileged position relative to other researchers. There are at least three circumstances when this privileged position could fall away. The first arises when consortium-generated genomic data is made openly available to all. The second arises when all that is required to become a consortium member is registration, after which broad data access is granted without the need to participate in joint research endeavours. The third is somewhat different; rather than making data access more open, a consortium may require an application to be made by anyone accessing consortium-generated genomic data, vetted by the consortium, irrespective of whether the user is a consortium member or not.
In contrast to the closed approach of CA, open access (OA) makes data publicly available without restriction 22 , 27 . The theory behind OA is that unfettered access assists in the verification and replication of data, broadens opportunities to pool data and generates results without the need to collect further data, leading to better quality results and establishment of community resources 27 , 32 . As noted above, when a consortium opts for OA this means that consortium members do not have privileged access.
The Human Genome Project (HGP) laid the foundation for OA. The HGP commenced in 1990, and from the outset, it was a collaborative venture, both between institutions and countries. The goals of the HGP were to map the genes and sequence the genetic code for the entire human genome. In 1996 HGP participants agreed in the Bermuda Declaration that primary genomic sequences should remain in the public domain and that they should be rapidly released 33 , 34 . GenBank was created as a publicly accessible repository of the sequence information produced by the HGP 35 .
By 2003, there was some relaxation of the high standards for OA imposed by the Bermuda Declaration. In particular, it was felt necessary to recognise the valuable input provided by data generators. The Fort Lauderdale agreement reflected this desire 34 . Further inroads were made into these pure OA principles through the HapMap Project and the Genetic Association Information Network, led by the NIH 34 . Recognition of the input of data generators, protection of the privacy of data sources and avoidance of data capture for commercialisation purposes are all reasons why it is difficult to apply OA principles to all aspects of genomic data sharing 36
Registered access
Registered access (RA) is used here to describe access that does not fully align with OA standards 23 , 24 . Researchers requesting access through this mechanism are not required to sign or abide by a formalised data transfer agreement. Rather, they may simply be required to accept the terms of use through a simple online agreement, by clicking ‘I agree’ in a checkbox or similar administratively ‘light’ procedure 24 . The GA4GH Data Sharing Lexicon describes RA as ‘a system of authentication and self-declaration prior to providing access to data.’ 20 The benefit of RA is that it creates a simple mechanism to verify the legitimacy of the user and to bind them to contractual terms regarding future uses of the data and other matters 23 , 24 . In this regard, it is less burdensome than managed access, considered below.
The HapMap Project marked the first step towards this RA approach. Its goal was to make sequence information available in a publicly accessible database 37 . The licence required users accessing the database to undertake that they would not restrict others from accessing or using the early-stage data they generated from the primary data. This obligation attracted some controversy, because it marked a significant change in philosophy from OA, although others saw it as an effective safeguard against capture 38 .
In some instances, consortia apply RA principles not just for data access but for consortium membership. This is another instance when there is no privileged access for consortium members who participate in joint research endeavours.
Managed access
Another broad descriptor of access arrangements is managed access (MA). The MA approach requires that data access is managed or controlled by the consortium. In some instances, consortium members are required to comply with the same formal MA arrangements as external users, which is another example of circumstances where privileged access to data for consortium members is lost. This can arise when consortium data is not held centrally but rather is held by the organisation generating the data. Arrangements of this nature are described as federated access 39 , 40 , 41 . The GA4GH Beacon Project is an example of a system designed to facilitate federated access (amongst other things) 42 .
By imposing restrictions on data access 24 , MA arrangements involve more regulatory action by the consortium. Conditions might include who can access, what they can access, and how and under what terms access may be granted (i.e. on an internal server or downloaded) [ 22 ]. The term MA is not used ubiquitously; ‘controlled access’ and ‘restricted access’ are also common 22 , 24 , 25 . For instance, the ICGC uses controlled access to describe its access system for ‘composite genomic and clinical data that are associated to a unique, but not directly identifiable, person’, contrasting with its OA system for non-identifiable data 22 . Dyke et al. appear to use the terms MA and controlled access interchangeably 23 . The GA4GH Lexicon suggests that restricted access and controlled access are equivalent 20 . On this basis, we conclude that these terms are variations on the same theme—managing who can access data and on what terms, and for this reason, we refer to them collectively as MA.
Commonly, this degree of control is justified by the nature of the data, or to comply with conditions imposed by participant consent forms or by research ethics committees 20 , 27 . Dyke et al. suggest that genomic research consortia that employ MA should, by definition, have a Data Access Committee (DAC) 23 . The primary functions of a DAC are to: provide broad oversight of data access and to facilitate and expedite the data access process; review applications for access; make determinations as to access of researchers and others to data, including by reference to the qualifications and legitimacy of the researchers and the purposes specified for their research; and impose and ensure compliance with conditions upon data use 19 , 26 , 43 . Despite these relatively common features of DACs, there is a significant degree of variation in their purposes and activities 43 , 44 .
In summary, although DACs are widely recognised as the oversight bodies to whom researchers must apply to access data, there is a lack of clarity about: the extent to which their requirements are mandatory, or universal 26 , 32 , 43 , 45 ; the level of substantive or non-substantive oversight they wield in relation to researcher requests for access to data; and the criteria they apply to decisions about data-access 19 , 32 , 43 , 44 , 45 , 46 . This uncertainty calls into question the extent to which having a DAC ensures accountability, security and compliance with conditions and restrictions on data access.
Tiered access
It might be assumed that the four categories of data access listed above conveniently describe the gamut of access arrangements used by genomic research consortia. Our research and the work of others shows that the reality is much more complex. Tiered access (TA) is used to describe these more complex access arrangements of genomic research consortia.
The TA model provides genomic research consortia with the opportunity to segment their datasets and choose different access arrangements that best suit the consortium, its members and data sources. For example, it may be used to allow consortium members to retain privileged access up to the point of publication of their early findings. The NIH Genomic Data Sharing Policy explicitly allows delayed access for these purposes 12 .
This approach may also be used to provide external researchers with OA to certain data types, but require them to go through a more formalised process for other data types. This approach can balance competing concerns relating to scientific progress and protecting donor privacy 22 . The OA model might be applied to a range of data types including: data that cannot be linked in order to identify donors; aggregate level data; or data that does not contain information that could allow donors to be identified 19 , 22 . By contrast, access to more sensitive data, particularly data that may allow donors to be identified, is more likely to be subjected to the controlled procedures of MA. This means that users are likely to be required to make an application to the consortium’s DAC and enter into a Data Access Agreement before they are able to use the sensitive data 19 , 22 .
The ICGC was one of the early adopters of this TA approach 21 . dbGaP also requires depositors to use a TA approach to data access by external users, applying OA to studies, study documents, phenotypic variables and genotype access, and MA (which it refers to as controlled access) to de-identified data, phenotypes and genotypes for individual study subjects and pedigrees 47 .
Analysis of specific genomic data access consortia arrangements
Each of the consortia in our dataset has expressed an explicit commitment to genomic data access in one way or another. Some provide clear guidance on the ways in which they share their data, through their websites and through other documentation, making classification relatively straightforward. For a surprisingly large number of consortia, however, it took us some time to clearly and precisely identify data access arrangements, requiring extensive searching of our datasets, further online searches and email requests to consortium administrators. For 32 consortia (33% of the dataset), we had to infer data access arrangements based on: funding sources (for example, consortia funded by the NIH or Wellcome have to comply with their policies); repositories within which their data were stored (for example, dbGaP has certain requirements); nature of the consortium; types of data that the consortium generates; and other factors. Information on the main sources used to determine data access is provided for each consortium in the Supplementary Materials.
In sum, we are reasonably confident that the express and inferred data access arrangements we have recorded provide a reasonably comprehensive account of the variety of arrangements across our consortium dataset, and the prevalence of some of these arrangements within the sector as a whole. In Table 1 , we list the options for genomic data access in genomic research consortia ranging from CA to highly sophisticated models using up to three access categories. It should be noted that permutations of access arrangements which were not observed in the dataset are not included in Table 1 . In each case where there is at least one genomic research consortium using the stated access options, we have identified an exemplar and listed the total number of consortia in our dataset which appear to use this arrangement, noting again our caution that the actual arrangements are more difficult to accurately identify for some consortia than others.
This study is testament to the growth of genomic research since the HGP. It illustrates that genomic research consortia are providing the essential engine rooms for this research effort, by providing access to large and diverse sets of genomic data. The Supplementary Materials provide ample evidence of volume and diversity of genomic datasets, with some consortia being highly disease specific, others focusing more generally on classes of disease (for example, cancers) and large-scale population-wide initiatives.
This study also illustrates an increasing sophistication in data access arrangements. The simple dichotomy between OA and closed CA has been replaced with more tiered approaches, with TA (CA-OA-MA) being most prevalent (with 41 consortia manifesting this structure). Some data access arrangements are relatively uncommon. Complete OA, for example, is unusual, seen only rarely post-HGP. Far more commonplace is the open sharing of summary results, generally post-publication. Somewhat unanticipated also was the lack of reliance on RA as a mechanism for controlling the movement of data. Even within a TA structure, mechanisms that provided greater control (through MA) appear to be favoured over systems that simply require a process of registration.
One thing that is clear is that consortia continue to be committed to making their datasets as open as possible. The Variant Interpretation for Cancer Consortium 48 provides a good example. Although it describes itself as an ‘open consortium’, consortium documents set out a commitment to ‘share… at least a minimal set of data elements for cancer variant interpretations including: gene symbol, variant name, cancer subtype (tumor type and organ), clinical implication (drug sensitivity, drug resistance, adverse response, diagnostic, or prognostic), source (e.g., PubMed identifier) and curation group.’ Justifiable concerns around the privacy of data donors and primary researcher interests no doubt motivate the adoption of a limited definition of ‘open’ access in this and other consortia.
The dominance of the TA(CA-OA-MA) model is not unexpected, given the mandates from funders like the NIH and Wellcome. This arrangement appropriately recognises the value in making some information freely available, whilst acknowledging that there is a need to provide appropriate protections to donors and their families. It further acknowledges the valuable contributions made by consortium members, by allowing them to publish the results of their initial analyses before data is made more broadly available. As consortia move towards more federated access models, it seems likely that tiered access arrangements of this nature will become the norm.
Table 1 illustrates the intricacies of data access arrangements in genomic research consortia. Despite calls for standardisation, the level of diversity is striking. These differences are, unsurprisingly, more pronounced with consortia unaffiliated with major funders, such as the NIH or Wellcome. This demonstrates that, absent mandated adherence to policy arrangements, consortia tend to adopt access arrangements that best suit the interests of members. Beyond this, what is more striking is the effort it took us to precisely identify data access arrangements for many of the consortia in our dataset. As noted earlier, transparency is recognised as one of the fundamental requirements for good governance in genomics 15 .
Transparency and accuracy in articulation of data access arrangements is important for a number of reasons. For consortium members, clear parameters around access are essential to ensure that they are fully cognisant of arrangements in respect of the data they contribute to the consortium. Whether data is truly openly available, for example, may influence a decision as to whether or not to contribute to a particular consortium. For data users, certain access structures undoubtedly complicate the process of requesting data. Managed access provides a level of protection to consortium members and donors, but is more administratively burdensome 22 . A lack of transparency around the process for requesting access is likely to constitute a significant disincentive for users.
The adoption of consistent data access arrangements by consortia funded by the NIH and other bodies is an important step in simplifying the genomic data sharing landscape. We are aware that some of the other consortia in our dataset are also in the process of updating their access arrangements to more closely reflect developing norms within the sector. Nevertheless, the analysis presented in this article highlights the need for more work to achieve a shared, consistent terminology for access arrangements within genomics consortia and for greater transparency about these access arrangements. Not only is this important for consortium members and users of consortium data, but it is also critical in recognising the valuable contributions made by donors.
Data availability
A list of all of the genomic research consortia in the dataset is provided in the supplementary materials. The full set of consortia-related documents is available from the authors on request.
Mittleman, B., Neil, G. & Cutcher-Gershenfeld, J. Precompetitive consortia in biomedicine—how are we doing?. Nat. Biotechnol. 31 , 979–985 (2013).
PubMed Google Scholar
Leonelli, S. (2009) Centralising labels to distribute data: The regulatory role of genomic consortia. In The Handbook of Genetics and Society: Mapping the New Genome Era (eds. Atkinson, P., Glasner, P., Lock, M.) 469–485 (Routledge, 2009).
Österle, H. & Otto, B. Consortium research. Bus. Inf . Syst. Eng. 2 , 283–293 (2010).
Google Scholar
Wallace, S. E. The needle in the haystack: international consortia and the return of individual research results. J. Law. Med. Ethics 39 , 631–639 (2011).
Burgio, M. R. et al. Collaborative cancer epidemiology in the 21st century: the model of cancer consortia. Cancer Epidemiol. Biomarkers Prev. 22 , 2148–2160 (2013).
PubMed PubMed Central Google Scholar
Papadaki, M. & Hirsch, G. Curing consortium fatigue. Science Trans. Med. 5 , 200fs35 (2013).
Teare, H. J. A. et al. The governance structure for data access in the DIRECT consortium: an innovative medicines initiative (IMI) project. Life Sci. Soc. Policy 14 , 1–17 (2018).
Burton, P. R. et al. Policies and strategies to facilitate secondary use of research data in the health sciences. Int. J. Epidemiol. 46 , 1729–1733 (2017).
Rehm, H. L. et al. GA4GH: International policies and standards for data sharing across genomic research and healthcare. Cell Genomics 1 , 100029. https://doi.org/10.1016/j.xgen.2021.100029 (2021).
Knoppers, B.M. (2014) Framework for responsible sharing of genomic and health-related data. HUGO J . 8 , Article 3 https://doi.org/10.1186/s11568-014-0003-1 (2014)
Joly, Y., Dove, E., Knoppers, B.M. & Nicol, D. The GA4GH Regulatory and Ethics Work Stream (REWS) at 10: An interdisciplinary, participative approach to international policy development in genomics. In The Law and Ethics of Data Sharing in Health Sciences. Perspectives in Law, Business and Innovation : (eds. Compagnucci, M.C., Minssen, T., Fenwick, M., Aboy, M. & Liddell. K.) 13–32 (Springer, 2024).
NIH, Genomic Data Sharing Policy (2014). Available at: https://sharing.nih.gov/genomic-data-sharing-policy (accessed 4 September 2024).
NIH, Policy for Data Management and Sharing (2023). Available at: https://oir.nih.gov/sourcebook/intramural-program-oversight/intramural-data-sharing/2023-nih-data-management-sharing-policy (accessed 4 September 2024)
Wellcome, Data, Software and Materials Management and Sharing Policy (undated). https://wellcome.org/grant-funding/guidance/policies-grant-conditions/data-software-materials-management-and-sharing-policy (accessed 4 September 2024)
O’Doherty, K. C. et al. Toward better governance of human genomic data. Nat. Genet. 53 , 2–8 (2021).
NIH, NIH-Supported Data Sharing Resources (undated). Available at: https://www.nlm.nih.gov/NIHbmic/nih_data_sharing_repositories.html (accessed 4 September 2024)
GA4GH, Driver Projects (undated). Available at: https://www.ga4gh.org/our-community/driver-projects/ # (accessed 4 September 2024)
Mailman, M. et al. The NCBI dbGaP database of genotypes and phenotypes. Nat. Genet. 39 , 1181–1186 (2007).
Expert Advisory Group on Data Access, Governance of Data Access (2015). Available at: https://wellcomecollection.org/works/zzr2qqpk/items (accessed 4 September 2024)
GA4GH, Global Alliance for Genomics and Health Data Sharing Lexicon (2016). Available at: https://www.ga4gh.org/document/archived-data-sharing-lexicon/ (accessed 4 September 2024)
International Cancer Genome Consortium, Goals, Structure, Policies and Guidelines, International Cancer Genome Consortium (2008). Available at: https://www.riken.jp/medialibrary/riken/pr/topics/2008/20081119_1/20081119_1_en.pdf (accessed 4 September 2024)
Joly, Y., Dove, E. S., Knoppers, B. M., Bobrow, M. & Chalmers, D. Data sharing in the post-genomic world: the experience of the International Cancer Genome Consortium (ICGC) Data Access Compliance Office (DACO). PLoS Comput. Biol. 8 , e1002549. https://doi.org/10.1371/journal.pcbi.1002549 (2012).
ADS PubMed PubMed Central Google Scholar
Dyke, S. et al. Registered access: a ‘Triple-A’ approach. Eur. J. Hum. Genet. 24 , 1676–1680 (2016).
Joly, Y., Dyke, S. O. M., Knoppers, B. M. & Pastinen, T. Are data sharing and privacy protection mutually exclusive?. Cell 167 , 1150–1154 (2016).
Learned, K. et al. Barriers to accessing public cancer genomic data. Sci. Data 6, Article 98, https://doi.org/10.1038/s41597-019-0096-4 (2019)
Kaye, J. & Hawkins, N. Data sharing policy design for consortia: challenges for sustainability. Genome Med, 6, Article 4, https://doi.org/10.1186/gm523
Muddyman, D., Smee, C., Griffin, H., Kaye, J. & UK10K Project. The UK10K Project. Implementing a successful data-management framework: the UK10K managed access model. Genome Med. 5, Article 100, https://doi.org/10.1186/gm504 (2013).
Joly, Y., Zeps, N. & Knoppers, B. M. Genomic databases access agreements: legal validity and possible sanctions. Hum. Genet. 130 , 441–449 (2011).
Fortin, S., Pathmasiri, S., Grintuch, R. & Deschênes, M. Access arrangements’ for biobanks: a fine line between facilitating and hindering collaboration. Public Health Genomics 14 , 104–114 (2011).
The All of Us Research Program Investigators. The “All of Us” research program. N. Engl. J. Med. 381 , 668–676 (2019).
PubMed Central Google Scholar
Villanueva, A. G. et al. Characterizing the biomedical data-sharing landscape. J. Law Med. Ethics 47 , 21–30 (2019).
Murtagh, M.J. et al. Better governance, better access: practising responsible data sharing in the METADAC governance infrastructure. Hum. Genomics 12, Article 24 , https://doi.org/10.1186/s40246-018-0154-6 (2018)
Bentley, D. R. Genomic sequence information should be released immediately and freely in the public domain. Science 274 , 533–534 (1996).
ADS PubMed Google Scholar
Cook-Deegan, R., Ankeny, R. A. & Maxson Jones, K. Sharing data to build a medical information commons: From Bermuda to the Global Alliance. Annu. Rev. Genomics Hum. Genet. 18 , 389–415 (2017).
National Centre for Biotechnology Information, GenBank overview (undated). Available at: https://www.ncbi.nlm.nih.gov/genbank/ (accessed 4 September 2024)
Gold, E.R. & Nicol, D. Beyond open source: patents, biobanks and sharing. In Comparative Issues in the Governance of Research Biobanks: Property, Privacy, Intellectual Property, and the Role of Technology. (eds. Pascuzzi, G., Izzo, U. & Macilotti, M.) 191–208 (Springer, 2013).
Chokshi, D.A. & Kwiatkowski D.P. Ethical challenges of genomic epidemiology in developing countries. Genomics, Society and Policy 1, Article 1 https://doi.org/10.1186/1746-5354-1-1-1 (2005).
Kent, A. Patients and IP – Should we care?. SCRIPT-ed 3 , 260–264 (2006).
Chaterji, S. et al. Federation in genomics pipelines: Techniques and challenges. Brief. Bioinform. 20 , 235–244 (2019).
Stark, Z. et al. Integrating genomics into healthcare: A global responsibility. Am. J. Hum. Genet. 104 , 13–20 (2019).
Thorogood, A. et al. International federation of genomic medicine databases using GA4GH standards. Cell Genomics 1 , 100032. https://doi.org/10.1016/j.xgen.2021.100032 (2021).
Fiume, M. et al. Federated discovery and sharing of genomic data using Beacons. Nat Biotechnol. 37 , 220–224 (2019).
Shabani, M., Thorogood, A. & Borry, P. Who should have access to genomic data and how should they be held accountable? Perspectives of Data Access Committee members and access. Eur. J. Hum. Genet. 24 , 1671–1675 (2016).
Lawson, J., Rahimzadeh, V., Baek, J. & Dove, E. S. Achieving procedural parity in managing access to genomic and related health data: A global survey of data access committee members. Biopreserv Biobank. 22 , 123–129 (2023).
Shabani, M., Dyke, S. O., Joly, Y. & Borry, P. Controlled access under review: improving the governance of genomic data access. PLoS Biol. 13 , e1002339. https://doi.org/10.1371/journal.pbio.1002339 (2015).
Cheah, P.Y. & Piasecki, J. Data access committees. BMC Med. Ethics 21 Article 12 https://doi.org/10.1186/s12910-020-0453-z (2020).
Tryka, K.A. et al. (2013) The Database of Genotypes and Phenotypes (dbGaP) and PheGenI. In: The NCBI Handbook [Internet]. 2nd edition. (National Center for Biotechnology Information (US), 2013). Available at: https://www.ncbi.nlm.nih.gov/books/NBK154410/ (accessed 4 September 2024)
VICC, Variant Interpretation for Cancer Consortium (undated). Available at: https://cancervariants.org/index.html (accessed 4 September 2024)
Download references
Acknowledgements
The authors acknowledge and thank other members of the Centre for Law and Genetics at the University of Tasmania for their encouragement and advice throughout this project and thank the Centre’s research assistants for their assistance with data collection, storage and preliminary analysis. We particularly acknowledge and thank Rachel Hay, who made a significant contribution to the early data collection and preliminary analysis, and Hugh Oxbrough, who assisted with finalising the consortium documentation.
This research was funded through the Australian Research Council’s Discovery Project scheme, DP180100269.
Author information
Authors and affiliations.
Centre for Law and Genetics, University of Tasmania, Hobart, TAS, Australia
Dianne Nicol & Jane Nielsen
Faculty of Business and Law, Australian Centre for Health Law Research, Queensland University of Technology, Brisbane, QLD, Australia
Madeleine Archer
You can also search for this author in PubMed Google Scholar
Contributions
DN and JN conceptualised the project and contributed equally to data collection post-2021, data analysis and writing of the manuscript. MA undertook data collection and preliminary analysis. She wrote summary of the literature and reviewed the final manuscript.
Corresponding author
Correspondence to Dianne Nicol .
Ethics declarations
Competing interests.
Dianne Nicol is co-lead of the Regulatory and Ethics Workstream of the Global Alliance for Genomics and Health. The authors have no other competing interests.
Ethics approval
This project received ethics approval from the University of Tasmania Human Research Ethics Committee (Ethics Project ID: 18556). Ethics approval was not required for the aspect of the project reported in this article as all information was publicly available. Other aspects of this project (not reported in this article) involved interviews with consortium administrators for which ethics approval was granted.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Supplementary information., rights and permissions.
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/ .
Reprints and permissions
About this article
Cite this article.
Nicol, D., Nielsen, J. & Archer, M. Data access arrangements in genomic research consortia. Sci Rep 14 , 21685 (2024). https://doi.org/10.1038/s41598-024-72653-z
Download citation
Received : 04 April 2024
Accepted : 09 September 2024
Published : 17 September 2024
DOI : https://doi.org/10.1038/s41598-024-72653-z
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Genomic research consortia
- Genomic data sharing
- Access to genomic data
By submitting a comment you agree to abide by our Terms and Community Guidelines . If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.
Quick links
- Explore articles by subject
- Guide to authors
- Editorial policies
Sign up for the Nature Briefing newsletter — what matters in science, free to your inbox daily.
- Open access
- Published: 14 September 2024
Development of an infertility perception scale for women (IPS-W)
- Miok Kim 1 &
- Minkyung Ban 2
BMC Women's Health volume 24 , Article number: 513 ( 2024 ) Cite this article
Metrics details
The purpose of this study was to develop an Infertility Perception Scale for Women (IPS-W).
Initial items were based on an extensive literature review and in-depth interviews with five infertile women and fifteen women not diagnosed with infertility. Forty-one items were derived from a pilot survey. Data were collected from 203 women who had experienced intrauterine insemination (IUI) and in-vitro fertilization (IVF) more than once. The data were analyzed to verify the reliability and validity of the scale.
Four factors containing 21 items were extracted from the exploratory factor analysis (EFA) to verify the construct validity. The four factors of infertility perception scale were perceived feelings, personal stigma, social stigma, and acceptance. These factors explained 59.3% of the total variance. The confirmatory factor analysis (CFA) confirmed a four-factor structure of the 21-item IPS-W. All fit indices were satisfactory (χ 2 /df ≤ 3, RMSEA < 0.08). These items were verified through convergent, discriminant, known group validity, concurrent validity testing. The internal consistency reliability was acceptable (Cronbach’s α = 0.90).
The scale reflects the perception of infertility within the cultural context of Korea. The findings can help nurses provide support that is appropriate for individual circumstances by examining how women experiencing infertility perceive infertility.
Peer Review reports
Introduction
Infertility, defined as the failure to achieve pregnancy within one year of regular unprotected sexual intercourse for couples of reproductive age, is perceived in the socio-cultural context of Korea as an impediment to an essential social rite of passage and a health problem that threatens family continuity [ 1 ]. In fact, Koreans struggling with infertility believe that giving birth to a child is a prerequisite for a stable marital relationship and that having children allows the development of family relationships [ 2 ].
Infertility is perceived negatively due to the uncertainty, loss of control, and stressful situations [ 3 ] it causes, having a negative impact on quality of life [ 4 ]. Accordingly, decisions about treatment procedures should be made by each individual and as a couple after exploring various options and with an appropriate social support system. However, individuals with infertility often decide on infertility treatment without an appropriate decision-making process, due to the fear of experiencing social prejudice and negative perceptions when revealing infertility problems [ 5 ].
The psychological difficulties faced by individuals with infertility are partly caused by negative social perceptions [ 5 , 6 ]. Approximately half of all infertile couples tend to hide their infertility problem out of fear of social stigma [ 7 ]. Such stigmatizing views of infertility create a vicious cycle leading infertile individuals to have a negative perception of their problem, avoid or prematurely discontinue infertility treatment, and feel isolated from society [ 5 ].
Harzif, Santawi, and Wijaya [ 8 ] compared differences in perceptions towards infertility treatment between urban and rural areas by examining the level of knowledge on the risk factors for infertility, attitudes towards infertility, the social impact of infertility, and other options for infertile couples. However, as yet, the perceptions of the individuals receiving infertility treatment have not been specifically measured [ 9 ]. Despite the limited tools available for measuring infertility perceptions, some studies have assessed the stigmatizing characteristics of infertility; however, in most cases, the term “infertility” does not appear in the generic tools for measuring stigma [ 7 , 10 , 11 ]. Taebe et al. [ 5 ] developed the female infertility stigma instrument (ISI-F) based on the premise that infertility represents one of the biggest challenges in female reproductive and sexual health in most societies. However, the development of ISI-F relied on females attempting natural pregnancy, including ovulation induction. Consequently, while it shares some of the stigmatizing characteristics of infertile individuals, this tool may not adequately reflect the psycho-emotional difficulties of individuals receiving infertility treatments. The Infertility Stigma Scale (ISS) developed by Fu et al. [ 12 ] is designed to measure the perceived self-stigmas that a female receiving infertility treatment places on herself. However, the scale only encompasses the stigmatizing characteristics of infertility, therefore it does not allow for the assessement of the general perception that females undergoing infertility treatment have about their infertility, especially in a Korean context. The concept of stigma refers to a psychological attitude linked to a series of negative outcomes [ 12 ]. In contrast, perception refers to the process of recognizing and interpreting the nature and meaning of all types of stimuli and may vary depending on how individuals interpret the situation and the society they live in. Perception can be used to explore problems and make decisions on what should be changed and the strategy ahead [ 13 ]. Self-perceived stigma acts as a stress factor that leads to negative social stigma about infertility and interferes with life adaptation [ 14 ]; hence, it is all the more important to improve the perceptions of infertility.
Therefore, this study aims to develop a sensitive tool to measure how women who experience infertility treatment perceive their infertility, positioning them as active agents in coping with infertility. The goal is to assess their personal perceptions of infertility and facilitate a positive shift in those perceptions.
The development and validation of the infertility perception scale was performed in accordance with the method proposed by Devellis [ 15 ]. This study adheres to the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines.
Development of the infertility perception scale
Development of preliminary items.
To identify the components of infertility perception, previous literature published in RISS, PUBMED, EMBASE, and NDSL were searched for relevant studies and existing tools in English or Korean. Only studies with full-text availability were included. The search keywords included “infertility,” “fertility,” “infertile women,” “infertility for women,” “infertility experiences,” “experiences of infertility,” “assisted reproductive technology,” “intrauterine insemination,” “in vitro fertilization,” “perception,” and “awareness.” Among articles from PubMed, EMBase, and RISS, a total 42 articles were selected and reviewed, excluding duplicate articles ( n = 102), studies with no women subjects ( n = 48), studies not relevant to perception ( n = 205), systematic reviews ( n = 6), and case studies ( n = 21).
In-depth interviews were then conducted to confirm the initially identified items of infertility perception. The interviews were conducted separately for women who had not experienced infertility and women who were receiving infertility treatment to avoid the possible influence of social perception on the perception of infertility among the women under treatment [ 16 ]. Moreover, the emotional ups and downs experienced by individuals receiving infertility treatment may vary significantly depending on the number of follicles, the number and quality of the collected eggs, the need to undergo repetitive infertility treatments, and added negative emotions from previous failed treatments.
The women without experience of infertility were married women aged 20–69 years (three women per age group) selected by purposive sampling with consideration of their education level, economic status, and type of residence. The interviews, which lasted between 20 and 40 min, were conducted between April 7 and April 20, 2020.
Subsequently, interviews were conducted on six women undergoing IVF procedures to identify the central concept of infertility perception. Announcements were posted inside treatment centers to recruit potential participants. The interviews, which lasted between 50 and 70 min, were conducted between May 10 and May 18, 2020.
The central question in the interviews was “How do you feel about infertility?” The supplementary question for women not diagnosed with infertility was “What did you think when you found out someone who was diagnosed with infertility or has experienced receiving infertility treatment?” The supplementary question for women receiving infertility treatment was “What feelings or thoughts did you have as you were diagnosed with infertility and undergoing infertility treatment?” The in-depth interviews were recorded with the consent of the participants, transcribed immediately, and analyzed according to the content analysis procedure proposed by Krippendorff [ 17 ].
After defining the conceptual framework through content analysis based on literature review and in-depth interviews, a total of 103 items were derived. Subsequently, duplicate items and those with unclear content were deleted, revised, or supplemented through a meeting with an expert with infertility nursing and research experience. As a result, a total of 66 preliminary items were derived, including 29, 18, and 19 items in personal, relational, and social dimensions, respectively.
To avoid central bias, during the instrument development process, the 4-point scale proposed by Lynn [ 18 ] was used to grade each item based on the level of agreement (1: “Strongly disagree” to 4: “Strongly agree”). The items in sections 1, 2, and 3 of the scale are reverse-scored, so that a higher total score indicates a more positive perception of infertility.
Content validity testing
In this study, content validity was tested twice by calculating the content validity index (CVI) based on expert opinion. The appropriateness of each item was assessed using a 4-point Likert scale (4: “Highly relevant”; 3: “Quite relevant”; 2: “Somewhat relevant”; and 1: “Not relevant”). Items with an Item-Content Validity Index (I-CVI) ≥ 0.78 were selected. The first content validity testing was conducted in September 2020 by a 10-member expert panel [ 18 ].
The second content validity testing was conducted by five members from the first 10-member expert panel. Items with I-CVI ≥ 0.78 were selected, leading to a total of 41 preliminary items.
Pilot study
A pilot study was conducted with 20 women living in city B who had been diagnosed with infertility and received at least one round of assisted reproductive therapy to assess the level of understanding about the instrument and the time required to complete the questionnaire. The number of participants was based on the sample size of 20–40 participants for pilot studies proposed by Devellis [ 15 ]. Item appropriateness was assessed through questions such as “Are there any items that are difficult to understand?”, “Are there any items with ambiguous expressions?”, and “Are there any items that you believe lack relevance to the perception of infertility?”
Instrument evaluation
The instrument was assessed through item analysis, exploratory factor analysis (EFA), confirmatory factor analysis (CFA), convergent validity, discriminant validity, criterion validity, and reliability testing.
The subjects were married women aged 20 and above diagnosed with infertility; had received at least one round of IUI or IVF; currently receiving infertility treatment; understood the study’s purpose; and signed an informed consent. Those who had difficulties in understanding and responding to the self-reported questionnaire; had problems with cognitive comprehension; or had other physical disorders in addition to infertility were excluded. Based on the criteria that a sample size more than 200 or approximately five times the number of items would be appropriate for factor analysis [ 15 , 19 ] and considering a dropout rate of 10%, a total of 212 subjects were recruited.
Data was collected from eligible, voluntary participants from two hospitals between November 30, 2020 and February 5, 2021. In our study, a high valid response rate of 94.9% (203 valid responses out of 214 recruited participants) was achieved. This was primarily attributed to the structured approach in participant recruitment and data collection. Participants were initially approached by a researcher or trained assistant at the infertility treatment hospital, who provided a detailed explanation of the study’s purpose, the voluntary nature of participation, and assurances of confidentiality. Only those who expressed voluntary willingness to participate were provided with a QR code to access an online survey, which took approximately 15 to 20 min to complete. Conducting the survey during patients’ waiting times further facilitated participation. These factors collectively ensured that participants felt informed and comfortable in participating in the study.
For the concurrent validity, ISS developed by Fu et al. [ 12 ] was used. After obtaining permission, ISS was translated into Korean and was reviewed. Subsequently, the translated version was translated back into the original language and compared with the original items. The final version consisted of 27 items in Korean. The self-reported instrument consisted of four domains (self-devaluation, social withdrawal, public stigma, and family stigma) in 5-point scale (1: “Do not agree at all” to 5: “Strongly agree”). At the time of development, the reliability of the scale was indicated by Cronbach’s alpha = 0.94. Cronbach’s alpha was 0.86, 0.77, 0.92, and 0.84 for self-devaluation, social withdrawal, public stigma, and family stigma, respectively. In this study, the reliability of the scale was indicated by Cronbach’s alpha = 0.97. Cronbach’s alpha was 0.94, 0.86, 0.95, and 0.91 for self-devaluation, social withdrawal, public stigma, and family stigma, respectively.
Based on the evidence that a stigmatizing perception of infertility is associated with greater experience of negative emotions such as depression and anxiety [ 20 ], the Korean version of the Center for Epidemiologic Studies Depression Scale-Revised (K-CESD-R) [ 21 ] was used for known-group validity. The scale measures the severity of depressive symptoms according to four levels based on the frequency of the symptoms experienced during the past week. Each item receives 0 point for occurring never or rarely (during less than 1 day), 1 point for occurring some or a little of the time (1–2 days), 2 points for occurring occasionally or a moderate amount of time (3–4 days), and 3 points for occurring most or all of the time (5–7 days). The total scores for all the items of 0–15, 16–24, and 25–60 points were defined as normal, probable depression, and definite depression, respectively. According to Cho & Kim [ 22 ], the reliability of the scale was indicated by Cronbach’s alpha = 0.90 in the normal group ( N = 540), 0.93 in the clinical patient group ( N = 164), and 0.89 in the major depression group ( N = 46). In this study, the reliability of the scale was indicated by Cronbach’s alpha = 0.94.
Collected data were analyzed using SPSS version 25.0 program (IBM Corp., Armonk, NY, USA). The general and infertility-related characteristics of the subjects were analyzed by descriptive statistics using the frequency, percentage, mean, and standard deviation (SD). Item analysis was performed using mean, SD, skewness, and kurtosis. Moreover, item-total correlation analysis was performed, and items with an item-total correlation coefficient inferior to 0.30 were reviewed and deleted [ 23 ]. The construct validity was tested by EFA and the appropriateness of factor analysis was identified using the Kaiser-Meyer-Olkin (KMO) test and Bartlett’s test of sphericity. Furthermore, principal component analysis was used for factor extraction, while varimax rotation was used for factor rotation. For determination of the number of factors, eigenvalue ≥ 1, factor loading ≥ 0.50, commonality ≥ 0.40, and scree plot were considered [ 24 ].
The concurrent validity was tested using the Pearson’s correlation between the developed instrument and ISS [ 12 ], while the known-groups validity was tested using K-CESD-R [ 26 ]. Meanwhile, the differences in the infertility perception scores among the normal, probable depression, and definite depression groups were analyzed using one-way ANOVA, while a post-hoc test was performed using Scheffe’s test. Cronbach’s alpha was calculated to test the reliability.
General characteristics
The subjects’ age averaged 37.03 ± 4.56. The most response to cause of infertility was “unexplained” (57.1%). Most subjects (83.7%) had no children. The current treatments were IVF (57.1%) and IUI (42.9%). The 31.5% considered the treatment as moderately affordable, 15.8% viewed it as hardly affordable. The 11.3% had experience counseling for infertility. The 68.5% answered that their spousal support to infertility treatment was passive (Table 1 ).
Item analysis
Analysis of the items in the scale showed that the mean value was 1.27-3.00 and the SD was 0.48–0.97. The absolute skew and kurtosis values were 0.03–1.93 and 0.07–4.32, respectively, satisfying the criteria of an absolute skew value ≤ 2.0 and absolute kurtosis value ≤ 7.0 [ 25 ]. Accordingly, since multivariate normality was confirmed, all items were used in the analysis. The item-total correlation coefficient was 0.04–0.77, with 12 out of 41 items (items #6, 8, 9, 15, 22, 25, 28, 33, 36, 37, 38, and 39) showing an item-total correlation coefficient ≤ 0.30. Since these items were assessed as offering little contribution to the scale, they were deleted, leaving remaining items in the scale.
Validity testing
Construct validity testing.
A KMO value of 0.91 for 29 items and a Bartlett’s test of sphericity χ² value of 3137.40 ( p < .001) wear measured, confirming that the data were appropriate for factor analysis. After the first EFA, two items that were double-loaded on two factors (items #30 and 31) were deleted. After the second EFA on the remaining 27 items, three items that were double-loaded on two factors (items #12, 29, and 35) and three items with factor loading < 0.50 (items #1, 23, and 34) were deleted. Subsequently, the third EFA was performed using 21 items. The results showed a KMO value of 0.89 and a Bartlett’s test of sphericity χ² value of 1997.07 ( p < .001). Moreover, the commonality was 0.40–0.81, factor loading was 0.51–0.89, and there were four factors with eigenvalue > 1, which had a cumulative explanatory power of 59.3% (Table 2 ).
Four factors extracted according to infertility perception explained 59.3% of the total variance. In social science, an explanation of 40–60% of the variance for multifactor patterns is considered to be sufficient [ 26 ]. Factor-1 was named “perceived feelings,” consisting of six items explaining 34.6% of the total variance. Factor-2 was named “personal stigma,” consisting of eight items explaining 12.0% of the total variance. Factor-3 was named “social stigma,” consisting of three items explaining 6.6% of the total variance. Factor-4 was named “acceptance,” consisting of four items explaining 6.1% of the total variance.
According to the results of the exploratory factor analysis, the 21-item IPS-W with 4 factors underwent confirmatory factor analysis. The model fit was evaluated against predefined cutoff values for each fit index (χ 2 /df ≤ 3, AGFI ≥ 0.90, GFI ≥ 0.90, CFI ≥ 0.90, RMSEA < 0.08) [ 27 ]. The model achieved the following fit indices: χ 2 /df = 2.09, AGFI = 0.81, GFI = 0.85, CFI = 0.90, RMSEA = 0.07 (Fig. 1 ).
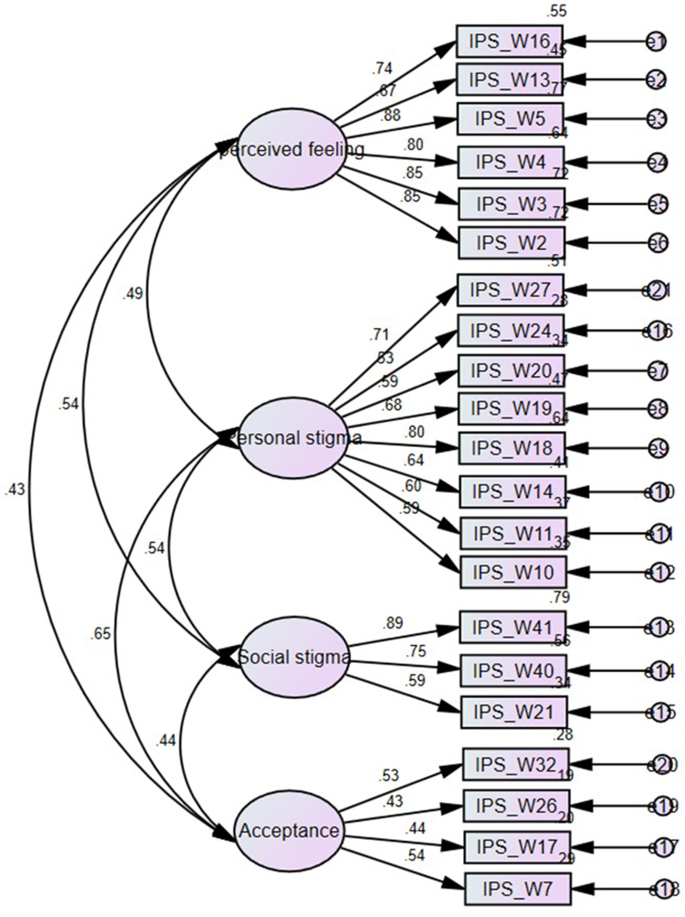
Measurement model of an infertility perception scale for women (IPS-W). χ 2 /df = 2.09, AGFI = 0.81, GFI = 0.85, CFI = 0.90, RMSEA = 0.07 χ 2 /df = Chi-square divided by degrees of freedom; AGFI = Adjustedm Goodness of Fit Index; GFI = Goodness of Fit Index; CFI = Comparative Fit Index; RMSEA = Root Mean Square Error of Approximation
Multi-trait/multi-item matrix analysis was performed. Convergent validity was validated since the correlation between each item and the total score in the corresponding subscale was 0.59–0.89, which satisfied the cut-off value of 0.40. Moreover, discriminant validity was also validated since the value derived by subtracting twice the standard error from the correlation coefficient between the item and the corresponding subscale was larger than the correlation coefficient of other sub-components.
Criterion validity testing
Concurrent validity was first tested based on the correlation of the scale with ISS. The results showed a positive correlation with a correlation coefficient of 0.63 ( p < .001), while also showing positive correlations between sub-factors with correlation coefficients ranging between 0.30 and 0.54. Accordingly, the concurrent validity of the scale was validated (Table 3 ).
Secondly, the known-groups validity was tested by dividing the subjects into groups by the level of depression based on CES-D cut-off points and analyzing the differences in infertility perception among the groups. Since the results showed significant differences in infertility perception according to the level of depression, the known-groups validity was validated (F = 18.84, p < .001; Table 4 ).
Reliability testing
The Cronbach’s alpha value of 21 infertility perception items was 0.90, and for each sub-domain, the Cronbach’s alpha value was 0.91, 0.85, 0.77, and 0.60 for Factor-1, 2, 3, and 4, respectively. According to the rationale by Hair et al. [ 19 ], a reliability ≥ 0.70 is considered acceptable for any new instrument (Table 2 ).
Factor-1 (perceived feelings) represents overall feelings about infertility, having a total explanatory power of 34.6%. Infertility not only causes psychological distress, such as sadness and loss of hope for the future [ 4 ], but it is also defined as an infertility crisis accompanied by physical, economic, and social stress [ 28 ]. The 50% of women considered this process as the most stressful experience in their life [ 29 ], while 84.2% of Korean women receiving infertility treatment experienced depression [ 4 ]. In Factor-1, the overall feeling about infertility was reflected by negative emotions including a sense of loss, anxiety, despair, depression, sadness, and guilt. Therefore, efforts are needed to understand the negative emotions of people who experience infertility and to alleviate these emotions.
Factor-2 refers to “personal stigma.” Infertility can be seen as the fault of the individual, while individuals who experience infertility perceive it as a void and a problem that is difficult to reveal. Personal stigma refers to the extent to which a person believes that negative stereotypes associated with a group they belong to will also be applied to them, while experiencing more personal stigma results in increased self-stigma, which is the feeling that the stigma is applicable to themselves [ 30 ]. Factor-2 reflects previous reports that women who marry but have not given birth are stigmatized as not fulfilling the role of a married woman and denying their own femininity [ 31 ]. Moreover, infertility diagnosis and treatment endlessly give women existential angst and hoping for a child is perceived as the attempt of women to understand their own existence even if they realize that such hope is in vain [ 32 ].
Infertility is understood differently depending on the socio-cultural context. A significant number of women diagnosed with infertility in Korea experience embarrassment and despair from their unexpected difficulties with fertility. Originally, they thought that having a child would be a natural process after getting married, and thus experience confusion about their sense of identity as a woman when this does not happen [ 33 , 34 ]. The perceptions of the Korean society surrounding infertility has been emphasized as an important factor influencing the sense of identity and emotions of individuals with infertility [ 35 ]. In other words, individuals currently undergoing infertility treatment have always perceived infertility negatively, rather than positively, as a member of the society before being diagnosed with infertility themselves. Such perception becomes palpable in their own lives once they are diagnosed with infertility, which adds stigmatizing characteristics to their perception of infertility.
Factor-3 (“social stigma”) includes stigmatizing characteristics about infertility at the societal level, believing that childbirth are an essential social rite of passage. But as they face difficulties with fertility, the views of other people become uncomfortable to women, leading them to withdraw from relationships. This could be interpreted as a factor similar to the “social withdrawal” mentioned by Fu et al. [ 12 ]. This process is well explained by studies reporting that, under the ideology of the Korean society, which regards motherhood as the main definer of a woman’s identity and has favorable views on having children, having friends or relatives that perpetrate a negative stigma around infertility and take a cruel view of women regardless of whether they are directly responsible for the infertility [ 36 ] can cause women with infertility to withdraw from relationships [ 33 ]. In fact, over 50% of Korean women who received infertility treatment experienced prejudice due to infertility and 43% reported serious withdrawal from relationships for this reason [ 34 ].
As previously described, infertility is not well understood and not adequately perceived within many societies [ 37 , 38 ]. Negative social perception about infertility can cause women who experience infertility to internalize social stigma, withdraw from interpersonal relationships, lose self-esteem, and experience decline in quality of life [ 14 ]. All items included in Factors 2 and 3 are close to problems stemming from perceived stigma, meaning one’s own belief that the society views them as a member of a stigmatized group [ 39 ].
Factor-4 reflects “acceptance,” whereby infertility is perceived as an acceptable problem that can be overcome together as a couple, rather than a problem that causes a negative outcome in life. Having no child due to infertility and the surrounding stigma can place a serious burden on the couple’s relationship and the difficulties may destroy the marriage or strengthen their bond [ 40 ]. The perception of infertility is deeply associated with the socio-cultural context due to the longstanding family norms in Korea. Recognizing infertility as a problem that can be overcome and understanding that individuals and the society must work together to resolve the problem.
Meanwhile, Factor-4 had a somewhat low reliability score of 0.60. This could be due to large differences in how positively individuals receiving infertility treatment think about infertility within their socio-cultural and familial context and how significant are their psycho-emotional changes, which may vary according to treatment stage, frequency of treatment, and outcomes during treatment (number of follicles, quality of eggs, number of embryos, quality of embryos, etc.). In the future, it may be necessary to repeat the measurements after unifying the infertility treatment on IUI or IVF or using the same measurement point like the start of treatment rather than during treatment to reduce the factors possibly acting as variables.
Validity and reliability
Concurrent validity test of the developed scale and ISS suggested that a more negative perception of infertility led to a higher perceived stigma about infertility [ 16 , 41 ]. Moreover, known-groups validity for comparing the level of infertility perception between groups showed that the depression groups perceived infertility more negatively than the normal group, consistent with a previous study [ 20 ], which validated the known-groups validity of the scale developed in the present study. The reliability of our scale corresponded to a Cronbach’s alpha of 0.90, indicating that the reliability was at an acceptable level and that all items were easily understood by women receiving infertility treatment.
Up to now, while there have been efforts to measure infertility perception, such efforts have focused mostly on the individual’s knowledge about infertility diagnosis and treatment or the stigmatizing characteristics of infertility within various socio-cultural contexts. In Korea, in particular, infertility has usually been perceived as having stigmatizing characteristics such as insufficiency and difficulty, but it is important to view infertility as a problem that can be overcome by working together, rather than a negative life event that can destroy the sense of identity of women and cause relationship problems among couples. The newly developed infertility perception scale also includes a significant number of the stigmatizing characteristics of infertility. Hence, efforts are needed to solve the issues surrounding inadequate beliefs through the understanding of the stigmatizing characteristics of infertility in order to transition towards a positive perception of infertility. Infertility not only causes individuals to experience various negative emotions but also impacts their life cycle, potentially increasing the risk of conditions such as coronary heart disease (CHD) [ 42 ] and elevating the likelihood of early menopause [ 43 ]. Therefore, a positive perception of infertility by those affected directly influences the individual, playing a crucial role in maintaining and promoting overall health.
Strengths, limitations, and future research
This study convenience sampled women receiving infertility treatment at two Korean hospitals specializing in infertility treatment, limiting the generalization of the findings. In addition, although we selected two institutions with similar treatment processes and patient education, there is a limitation in that we were unable to systematically analyze the similarities and differences. Prior to data collection, the authors informed the study participants that the survey was anonymous and that their responses would be kept confidential. However, there is a limitation that, due to social stigma, participants might have underreported or misreported their true opinions. Moreover, Cultural differences across countries can significantly influence perceptions of infertility, where what may be considered stigma or acceptable responses in one culture may not be the same in another. Therefore, it is essential to assess the validity and reliability across diverse populations, including different ethnic groups, and adjust the questionnaire accordingly to ensure cultural relevance and applicability. In future research, it is recommended that the validity and reliability of the scale be tested only among women who are at the IVF stage, as IVF is in the final stage of assisted reproductive therapy. Additionally, follow-up studies should aim to identify the level of infertility perception and to develop and test the impact of nursing interventions.
The infertility perception scale developed in the present study could predict the psycho-emotional state of women receiving infertility treatment by examining their infertility perception. These findings could be used for the development of nursing interventions that could help women experiencing infertility to approach positively the problem of infertility.
Conclusions
We developed and tested an infertility perception scale consisting in a 4-point Likert scale with 21 items under four factors. The scale has a score range of 21–84 points, with higher scores indicating more negative perceptions of infertility. The scale can be used to measure infertility perception among women who are experiencing infertility and their spouse, family, and friends. The findings can help nurses provide support that is appropriate for individual circumstances by examining how women experiencing infertility perceive infertility.
Data availability
Datasets used/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
Infertility Perception Scale for Women
Intrauterine insemination
in-Vitro Fertilization
Exploratory Factor Analysis
Confirmatory Factor Analysis
Female Infertility Stigma Instrument
Infertility Stigma Scale
Strengthening the Reporting of Observational Studies in Epidemiology
Content Validity Index
Item-Content Validity Index
Korean version of the Center for Epidemiologic Studies Depression Scale-Revised
Kaiser-Meyer-Olkin
Root-mean-square error of approximation
Adjusted Goodness-of-Fit Index
Goodness-of-Fit Index
Comparative Fit Index
Lee YH, Park JS. Factors affecting the infertility-related quality of life among the infertility women. J Korean Soc Maternal Child Health. 2019;23(3):191–201. https://doi.org/10.21896/jksmch.2019.23.3.191 .
Article Google Scholar
Podolska M, Bidzan M. Infertility as a psychological problem. Ginekologia Polska. 2011;82(1):44–9.
PubMed Google Scholar
Covington SN, Burns LH, editors. Infertility counseling: a comprehensive handbook for clinicians. Cambridge University Press; 2006.
Hwang NM. Factors related to the depression of infertile women. Health Social Welf Rev. 2013;33(3):161–87.
Taebi M, Kariman N, Montazeri A, et al. Development and psychometric evaluation of the female infertility stigma instrument (ISI-F): protocol for a mixed method study. Reproductive Health. 2020;17:70. https://doi.org/10.1186/s12978-020-0904-5 .
Article PubMed PubMed Central Google Scholar
Amiri M, Khosravi A, Chaman R, Sadeghi Z, Raei M, Jahanitiji MA, Mehrabian F. Social consequences of infertility on families in Iran. Global J Health Sci. 2016;8(5):89–94. https://doi.org/10.5539/gjhs.v8n5p89 .
Ergin RN, Polat A, Kars B, Öztekin D, Sofuoğlu K, Çalışkan E. Social stigma and familial attitudes related to infertility. Turkish J Obstet Gynecol. 2018;15(1):46–9. https://doi.org/10.4274/tjod.04307 .
Harzif AK, Santawi VPA, Wijaya S. Discrepancy in perception of infertility and attitude towards treatment options: Indonesian urban and rural area. Reproductive Health. 2019;16:126. https://doi.org/10.1186/s12978-019-0792-8 .
Meissner C, Schippert C, von Versen-Höynck F. Awareness, knowledge, and perceptions of infertility, fertility assessment, and assisted reproductive technologies in the era of oocyte freezing among female and male university students. J Assist Reprod Genet. 2016;33:719–29. https://doi.org/10.1007/s10815-016-0717-1 .
Article CAS PubMed PubMed Central Google Scholar
Jansen NA, Saint Onge JM. An internet forum analysis of stigma power perceptions among women seeking fertility treatment in the United States. Soc Sci Med. 2015;147:184–9. https://doi.org/10.1016/j.socscimed.2015.11.002 .
Article PubMed Google Scholar
Naab F, Brown R, Heidrich S. Psychosocial health of infertile Ghanaian women and their infertility beliefs. J Nurs Scholarsh. 2013;45(2):132–40. https://doi.org/10.1111/jnu.12013 .
Fu B, Qin N, Cheng L, Tang G, Cao Y, Yan C, Huang X, Yan P, Zhu S, Lei J. Development and validation of an infertility stigma scale for Chinese women. J Psychosom Res. 2015;79(1):69–75. https://doi.org/10.1016/j.jpsychores.2014.11.014 .
Introduction to perception. Retrieved from https://courses.lumenlearning.com/boundless-psychology/chapter/introduction-to-perception/
Gong JS. The effect of ex-prisoner’s perception of stigma on trust in international relationship. Korean Secur J. 2018;57:57–84.
Google Scholar
DeVellis RF. Scale development: theory and applications. 4th ed. Sage; 2016. pp. 39–199.
Seifer DB, Petok WD, Agrawal A, Glenn TL, Bayer AH, Witt BR, Burgin BD, Lieman HJ. Psychological experience and coping strategies of patients in the Northeast US delaying care for infertility during the COVID-19 pandemic. Reproductive Biology Endocrinol. 2021;19(1):28. https://doi.org/10.1186/s12958-021-00721-4 .
Article CAS Google Scholar
Krippendorff K. Content analysis: an introduction to its methodology. 2nd ed. Sage; 2004. pp. 1–413.
Lynn MR. Determination and quantification of content validity. Nurs Res. 1986;35(6):382–5.
Article CAS PubMed Google Scholar
Hair JF, Black WC, Babin BJ, Anderson RE. Multivariate data analysis: a global perspective. 7th ed. Pearson Education; 2010. pp. 111–3.
Davis M, Ventura JL, Wieners M, Covington SN, Vanderhoof VH, Ryan ME, et al. The psychosocial transition associated with spontaneous 46, XX primary ovarian insufficiency: illness uncertainty, stigma, goal flexibility, and purpose in life as factors in emotional health. Fertil Steril. 2010;93(7):2321–9. https://doi.org/10.1016/j.fertnstert.2008.12.122 .
Lee S, Oh ST, Ryu SY, Jun JY, Lee K, Lee E, et al. Validation of the Korean version of Center for epidemiologic studies Depression Scale-revised (K-CESD-R). Korean J Psychosom Med. 2016;24(1):83–93.
Cho MJ, Kim KH. Diagnostic validity of the CES-D (Korean version) in the assessment of DSM-III-R major depression. J Korean Neuropsychiatric Association. 1993;32(3):381–99.
Lee CY. (2016). Advanced nursing statistics (pp. 231–264). Soomunsa.
Noh GS. (2019). The proper methods of statistical analysis for dissertation: SPSS & AMOS 21 (pp. 141–193). Hanbit Academy.
Curran PJ, West SG, Finch JF. The robustness of test statistics to non-normality and specification error in confirmatory factor analysis. Psychol Methods. 1996;1(1):16–29. https://doi.org/10.1037/1082-989X.1.1.16 .
Sternke EA, Abrahamson K. Perceptions of women with infertility on stigma and disability. Sex Disabil. 2015;33:3–17. https://doi.org/10.1007/s11195-014-9348-6 .
Moon SB. Understanding and application of structural equation modeling. Seoul: Hakjisa; 2009.
Faramarzi M, Pasha H, Esmailzadeh S, Kheirkhah F, Heidary S, Afshar Z. The effect of cognitive behavioral therapy and pharmacotherapy on infertility stress: a randomized controlled trial. Int J Fertility Steril. 2013;7(3):199–206.
Herrmann D, Scherg H, Verres R, Von Hagens C, Strowitzki T, Wischmann T. Resilience in infertile couples acts as a protective factor against infertility-specific distress and impaired quality of life. J Assist Reprod Genet. 2011;28(11):1111–7. https://doi.org/10.1007/s10815-011-9637-2 .
Muñoz M, Finnegan K, Zeladita J, Caldas A, Sanchez E, Callacna M, et al. Community-based DOT-HAART accompaniment in an urban resource-poor setting. AIDS Behav. 2010;14(3):721–30. https://doi.org/10.1007/s10461-009-9559-5 .
Jeong KI. A study on hermeneutic grounded theory of women who experience infertility suffering and relief from pain. Korean J Social Welf Stud. 2014;45(4):5–35. https://doi.org/10.16999/KASWS.2014.45.4.5 .
Boz I, Okumus H. The everything about the existence experiences of Turkish women with infertility: solicited diaries in qualitative research. J Nurs Res. 2017;25(4):268–75. https://doi.org/10.1097/jnr.0000000000000166 .
Yang SN. The experience of infertility treatments among working women without children. Korean J Social Welf Educ. 2019;48:93–120. https://doi.org/10.1111/j.1467-9566.2009.01213.x .
Jeong YM, Kang SK. A phenomenological study on infertile experiences of women: Waiting for Meeting. Stud Life Cult. 2017;44:271–319.
Ryu SJ. A phenomenological study on infertility as the missing piece in socialization process: focusing on university students’ perception of infertility. Family Cult. 2021;33(2):38–65. https://doi.org/10.21478/family.33.2.202106.002 .
Ryu SJ. Infertility, the social context of deferred motherhood: a qualitative inquiry based on an online infertility community. J Asian Women. 2019;58(2):5–38.
Bunting L, Boivin J. Knowledge about infertility risk factors, fertility myths and illusory benefits of healthy habits in young people. Hum Reprod. 2008;23(8):1858–64. https://doi.org/10.1093/humrep/den168 .
Fido A. Emotional distress in infertile women in Kuwait. Int J Fertil Women’s Med. 2004;49(1):24–8.
LeBel TP. Perceptions of and responses to stigma. Sociol Compass. 2008;2(2):409–32. https://doi.org/10.1111/j.1751-9020.2007.00081.x .
Valsangkar S, Bodhare T, Bele S, Sai S. An evaluation of the effect of infertility on marital, sexual satisfaction indices and health-related quality of life in women. J Hum Reproductive Sci. 2011;4(2):80–5. https://doi.org/10.4103/0974-1208.86088 .
Sobral MP, Costa ME, Schmidt L, Martins MV. COMPI fertility problem stress scales is a brief, valid and reliable tool for assessing stress in patients seeking treatment. Hum Reprod. 2017;32(2):375–82. https://doi.org/10.1093/humrep/dew315 .
Farland LV, Wang YX, Gaskins AJ, Rich-Edwards JW, Wang S, Magnus MC, et al. Infertility and risk of cardiovascular disease: a prospective cohort study. J Am Heart Association. 2023;12(5):e027755. https://doi.org/10.1161/JAHA.122.027755 .
Liang C, Chung HF, Dobson AJ, Cade JE, Greenwood DC, Hayashi K, et al. Is there a link between infertility, miscarriage, stillbirth, and premature or early menopause? Results from pooled analyses of 9 cohort studies. Am J Obstet Gynecol. 2023;229(1):47e1. 47.e9.
Download references
Acknowledgements
This work was supported by the National Research Foundation of Korea (NRF) grant funded by the Korea government (MSIT) (No. 2019R1F1A106291912).
Author information
Authors and affiliations.
Department of Nursing, College of Nursing, Dankook University, Cheonan, South Korea
Department of Nursing, College of Nursing, Catholic University of Pusan, Busan, South Korea
Minkyung Ban
You can also search for this author in PubMed Google Scholar
Contributions
Conceptualization or/and Methodology: Kim Miok. Data curation or/and Analysis: Ban Minkyung. Funding acquisition: Kim MiokInvestigation: Ban Minkyung. Project administration or/and Supervision: Kim Miok. Resources or/and Software: Kim Miok, Ban Minkyung. Validation: Kim Miok. Visualization: Kim Miok, Ban Minkyung. Writing: original draft or/and review & editing: Kim Miok, Ban Minkyung.
Corresponding author
Correspondence to Minkyung Ban .
Ethics declarations
Ethics approval.
This study obtained an approval from the Institutional Review Board (IRB) of Dankook University (IRB approval no.: DKU 2021-01-022). Consent was obtained from the subjects after informing them about the purpose and procedures of the study and the protection of personal information. Only those who voluntarily consented to participate in the study were included. The subjects were given a small token of appreciation for their participation.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary Material 1
Rights and permissions.
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/ .
Reprints and permissions
About this article
Cite this article.
Kim, M., Ban, M. Development of an infertility perception scale for women (IPS-W). BMC Women's Health 24 , 513 (2024). https://doi.org/10.1186/s12905-024-03336-0
Download citation
Received : 21 September 2023
Accepted : 27 August 2024
Published : 14 September 2024
DOI : https://doi.org/10.1186/s12905-024-03336-0
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Infertility, female
- Social stigma
- Factor analysis, statistical
BMC Women's Health
ISSN: 1472-6874
- General enquiries: [email protected]

IMAGES
VIDEO
COMMENTS
In this post, we'll review the purpose of literature reviews, why they are so significant, and the specific elements to include in one. Literature reviews can: 1. Provide a foundation for current research. 2. Define key concepts and theories. 3. Demonstrate critical evaluation. 4. Show how research and methodologies have evolved.
The purpose of a literature review is to: Provide a foundation of knowledge on a topic; Identify areas of prior scholarship to prevent duplication and give credit to other researchers; Identify inconstancies: gaps in research, conflicts in previous studies, open questions left from other research;
What is the purpose of a literature review? There are several reasons to conduct a literature review at the beginning of a research project: To familiarize yourself with the current state of knowledge on your topic. To ensure that you're not just repeating what others have already done. To identify gaps in knowledge and unresolved problems ...
Writing a Literature Review. A literature review is a document or section of a document that collects key sources on a topic and discusses those sources in conversation with each other (also called synthesis). The lit review is an important genre in many disciplines, not just literature (i.e., the study of works of literature such as novels and ...
The introduction should clearly establish the focus and purpose of the literature review. Tip If you are writing the literature review as part of your dissertation or thesis, reiterate your central problem or research question and give a brief summary of the scholarly context. You can emphasize the timeliness of the topic ("many recent ...
What kinds of literature reviews are written? Narrative review: The purpose of this type of review is to describe the current state of the research on a specific topic/research and to offer a critical analysis of the literature reviewed. Studies are grouped by research/theoretical categories, and themes and trends, strengths and weakness, and gaps are identified.
The purpose of a literature review. The four main objectives of a literature review are:. Studying the references of your research area; Summarizing the main arguments; Identifying current gaps, stances, and issues; Presenting all of the above in a text; Ultimately, the main goal of a literature review is to provide the researcher with sufficient knowledge about the topic in question so that ...
A literature or narrative review is a comprehensive review and analysis of the published literature on a specific topic or research question. The literature that is reviewed contains: books, articles, academic articles, conference proceedings, association papers, and dissertations. It contains the most pertinent studies and points to important ...
A literature review is a survey of scholarly sources on a specific topic. It provides an overview of current knowledge, allowing you to identify relevant theories, methods, and gaps in the existing research. There are five key steps to writing a literature review: Search for relevant literature. Evaluate sources. Identify themes, debates and gaps.
What kinds of literature reviews are written? Narrative Review: The purpose of this type of review is to describe the current state of the research on a specific topic/research and to offer a critical analysis of the literature reviewed. Studies are grouped by research/theoretical categories, and themes and trends, strengths and weakness, and gaps are identified.
A literature review is a review and synthesis of existing research on a topic or research question. A literature review is meant to analyze the scholarly literature, make connections across writings and identify strengths, weaknesses, trends, and missing conversations. A literature review should address different aspects of a topic as it ...
Besides the obvious reason for students -- because it is assigned! -- a literature review helps you explore the research that has come before you, to see how your research question has (or has not) already been addressed. You identify: core research in the field. experts in the subject area. methodology you may want to use (or avoid)
The word "literature review" can refer to two related things that are part of the broader literature review process. The first is the task of reviewing the literature - i.e. sourcing and reading through the existing research relating to your research topic. The second is the actual chapter that you write up in your dissertation, thesis or ...
Narrative Reviews: The purpose of this type of review is to describe the current state of the research on a specific research topic and to offer a critical analysis of the literature reviewed. Studies are grouped by research/theoretical categories, and themes and trends, strengths and weaknesses, and gaps are identified.
A literature review is a critical analysis and synthesis of existing research on a particular topic. It provides an overview of the current state of knowledge, identifies gaps, and highlights key findings in the literature. 1 The purpose of a literature review is to situate your own research within the context of existing scholarship, demonstrating your understanding of the topic and showing ...
A literature review is a comprehensive summary of previous research on a topic. The literature review surveys scholarly articles, books, and other sources relevant to a particular area of research. ... "In writing the literature review, the purpose is to convey to the reader what knowledge and ideas have been established on a topic, and what ...
A literature review may consist of simply a summary of key sources, but in the social sciences, a literature review usually has an organizational pattern and combines both summary and synthesis, often within specific conceptual categories.A summary is a recap of the important information of the source, but a synthesis is a re-organization, or a reshuffling, of that information in a way that ...
A literature review and a theoretical framework are not the same thing and cannot be used interchangeably. While a theoretical framework describes the theoretical underpinnings of your work, a literature review critically evaluates existing research relating to your topic. You'll likely need both in your dissertation.
A literature review is a written work that: Compiles significant research published on a topic by accredited scholars and researchers; Surveys scholarly articles, books, dissertations, conference proceedings, and other sources; Examines contrasting perspectives, theoretical approaches, methodologies, findings, results, conclusions.
Literature Review is a comprehensive survey of the works published in a particular field of study or line of research, usually over a specific period of time, ... A literature review serves several purposes. For example, it. provides thorough knowledge of previous studies; introduces seminal works. ...
Therefore, this paper discusses the purposes of LRs in dissertations and theses. Second, the paper considers five steps for developing a review: defining the main topic, searching the literature, analyzing the results, writing the review and reflecting on the writing. Ultimately, this study proposes a twelve-item LR checklist.
PURPOSES OF A LITERATURE REVIEW 1. orient your reader by defining key concepts (theoretical) and/or providing relevant background (empirical) 2. ... The literature review is an opportunity to discover and craft your scholarly identity through the kinds of questions you engage, the discussions you enter, the critiques you launch, and the ...
A literature review can be just a simple summary of the sources, but it usually has an organizational pattern and combines both summary and synthesis. A summary is a recap of the important information of the source, but a synthesis is a re-organization, or a reshuffling, of that information. It might give a new interpretation of old material or ...
Purpose and Importance of the Literature Review. An understanding of the current literature is critical for all phases of a research study. Lingard 9 recently invoked the "journal-as-conversation" metaphor as a way of understanding how one's research fits into the larger medical education conversation. As she described it: "Imagine yourself joining a conversation at a social event.
What is a literature review? A literature review is an account of the current thinking in a specific area of study. Its purpose is to introduce the reader to what has gone before and often to provide you with a foundation that you can build on with your own research. This traditional form of review is sometimes also referred to as a narrative ...
Background: The purpose of this narrative review is to examine the literature investigating a causal relationship between stress and migraine and evaluate its implications for managing migraine. Methods: PubMed, PsycINFO and CINAHL were searched from 1988 to August 2021, identifying 2223 records evaluating the relationship between stress and migraine. Records were systematically screened. All ...
Purpose of Review This narrative review summarizes current literature on the relationship of mitochondrial biomarkers with obesity-related characteristics, including body mass index and body composition. Recent Findings Mitochondria, as cellular powerhouses, play a pivotal role in energy production and the regulation of metabolic process. Altered mitochondrial functions contribute to obesity ...
In line with Zheng et al. (Citation 2016) review, the literature search was conducted in online databases Embase, Medline Complete, CINAHL, and PsycInfo. Searches took place from July to August 2021. ... We fully appreciate that some software is intended for research purposes exclusively (as stated by 37.2% of survey respondents).
This article reports on a review of the genomic research consortium literature illustrating a wide diversity in the language that has been used over time to describe the access arrangements of ...
The purpose of this study was to develop an Infertility Perception Scale for Women (IPS-W). Initial items were based on an extensive literature review and in-depth interviews with five infertile women and fifteen women not diagnosed with infertility. Forty-one items were derived from a pilot survey. Data were collected from 203 women who had experienced intrauterine insemination (IUI) and in ...